Abstract
Non-adherence to antiretroviral treatment is one of the biggest challenges in the fight against HIV. In this study, the researcher was interested in determining the level and causes of non-adherence to ART among residents of Miami-Dade County. Current reports indicate that the county has registered the highest number of new infections for the last three years in the United States. It was necessary to find out why the fight against the spread of the virus was not yielding the desired success in the country. Data used in this study was obtained from primary and secondary sources. The study reviewed existing literature to understand the nature of the problem. Primary data was obtained from a sample of respondents. The researcher was also able to access data from the AIDS Healthcare Foundation within the county. The study found out that being new to chronic disease management, low levels of health literacy and health responsibility, psychological issues, nondisclosure of HIV status, and substance abuse issues are some of the main reasons why patients fail to take their drugs regularly. Other reasons include busy or irregular lifestyle, cost and insurance issues, difficulty with taking medication, and young age. The study suggests how these issues should be addressed to enhance the level of adherence.
Statement of Original Work
I declare that this is my original work and that it has never been submitted anywhere for academic or non-academic reasons. Plagiarism was avoided throughout the paper.
The Problem
Research Problem
The infection by the Human immunodeficiency virus (HIV) is one of the most feared epidemics in modern society. It has claimed millions of lives across the world since the 1980s, and medical researchers are yet to find ways of eradicating it. However, they have come up with antiretroviral (ARV) treatment that decreases the virus level in the blood. Once a person is infected with HIV, Karim (2015) explains that he or she needs to adhere to the treatment to ensure that the viral load is managed. Scientific studies have proven that one can lead a normal life if the viral load is maintained at the lowest level possible. It is also proven that when the viral load is maintained at very low levels, an infected individual has a tremendously reduced and very close to zero probability to transmit the virus to a healthy person. It explains why medical practitioners have been emphasizing the relevance of adherence to the antiretroviral therapies in the control of HIV.
It is worrying that an important portion of the patients does not adhere to the ARV medications as is needed and, as a consequence, the percentage of clients virally suppressed among the total identified HIV positive population is still too low to effectively reverse the HIV/AIDS outbreak (Cohen et al., 2016). Statistics show that in some states such as Florida, the rate of new infections is increasing despite the effort put in place by the local and federal government of the United States to fight this epidemic (McKinney et al., 2016). It is necessary to find a way of addressing this problem to help eradicate HIV from American society, especially in Miami-Dade County where the numbers indicate that there are a higher incidence and prevalence of HIV compared with other parts of the country. The research proposal will be centered on finding the main causes of non-adherence to the antiretroviral treatment in a group of HIV positive clients in Miami-Dade County as well as in reinforcing the role of the adherence to those regimens in the control of the HIV/AIDS epidemic.
Problem Background
The government of the United States has made a serious investment in the fight against HIV in terms of hiring medical experts and researchers and in the manufacture of ARV meds to help manage the problem. However, statistics show that although positive progress has been made in reducing the rate of new infections, the problem persists. According to McKinney et al. (2016), it is estimated that over 1 million people in the United States are currently living with the virus, some of whom are not even aware that they are infected. In 2014 alone, about 37,600 new cases of infection were reported in the country. It is reassuring that from 2008 to 2014, the country registered an overall drop in the rate of new infections by 18%. As the country makes progress towards the fight against this pandemic, some parts of the country still register poor performance. Collins-Bride (2017) observes that over 50% of new infections in the country are reported in the southern states. Miami Dade County is one of the southernmost parts of the United States, in Florida State; with a population of 2,712,945 people, it is the seventh-most populous county in the country and the most populous in Florida (The Insight Start Study Group, 2015). The beautiful beaches of Miami and the warm climate throughout the years have been attracting tourists from all over the world, leading to an economic boom. However, the increased number of visitors and the easy life that comes with the tourists have had a serious negative impact on the fight against the spread of HIV.
Since 2014, Miami-Dade Country has remained number one in terms of new cases of HIV infections in the entire country (Cohen et al., 2016). It is estimated that about 25,457 people in the county were living with diagnosed HIV in 2005, out of which 27% were born as women while 73% were born as men. The statistics also show that 44% of those living with the virus are Hispanics, 43% are black, and 11% were white (The Temprano ANRS 12136 Study Group, 2015). From 2011 to 2015, 80% of the newly diagnosed HIV patients were male, while 20% were women. In 2014, about 1,916 people diagnosed with HIV in Florida succumbed to various diseases because of their compromised immune system. The problem is becoming increasingly common among African Americans than any other race in the county. An urgent measure needs to be taken to ensure that this problem is eradicated or at least reduced significantly. The fight against this pandemic can take different approaches such as promoting safe sex, sensitizing the society about the importance of ARVs, and the use of Pre-exposure prophylaxis (or PrEP) among others. However, this study primarily focuses on the importance of adherence to antiretroviral treatment as a way of improving the current HIV/AIDS scenario.
Purpose of the Study
The purpose of this study is to analyze the leading reasons for non-adherence to the antiretroviral regimen in a specific group of HIV positive clients in the Miami-Dade area at the same time that expect to reinforce the value of the adherence to those treatments.
The primary goal of antiretroviral treatment is to strengthen the immune system. When the treatment regimen is taken as per the prescription, it suppresses the viral load in the body, making it easy for the immune system to function normally. Such a patient can live a normal life because HIV is more likely to respond to medication than in patients who do not adhere to the ARV therapies, allowing the body to prevent and/or recover from the damage that the virus produces (Friedman et al., 2016). According to Uusküla et al. (2018), adherence to ARV treatment (ART) also reduces the chances of an infected person transmitting the virus to a healthy individual. When the viral load is suppressed to the lowest level possible, the chances are high that one cannot transmit it to a partner even if they have unprotected sex, though such risky acts are discouraged. The study seeks to identify factors that limit adherence to the treatment in Miami-Dade and ways in which these hindrances can be eliminated. Hudelson and Cluver (2015) argue that lack of proper adherence to ARV treatment may be blamed on individual patients, healthcare centers that do not stock adequate drugs, nurses, and doctors who fail to explain to the patients the significance of taking their medicine regularly, or any other factor.
Significance of the Study
Recent reports indicate that Miami Dade County is currently recording the worst numbers of new HIV infections in the United States. The county is known for its beautiful beaches, good weather throughout the years, and relatively high levels of security (Bhatti, Usman, & Kandi, 2016). These factors have made it very attractive to the tourists who come to spend some time away from work and routines at home. The leisure and lifestyle of these visitors and the locals that frequent the beaches are largely blamed for the growing cases of new HIV infection. This study aims at promoting adherence to ARV therapies as a way of combating this disease. As Friedman et al. (2016) observe HIV/AIDS pandemic has been a major global health problem in the past three decades. A report by Temoshok (2016) shows that about 70% of the Americans infected with the virus stick to their treatment as advised by their doctors while 30% do not.
The county is still in danger of experiencing new infections because of the remaining 30% of the HIV patients who are not adhering to their treatment regularly. Through this study, it will be possible to identify reasons why some of these patients fail to adhere to their ARV regimen as religiously as would be expected. Sabin et al. (2016) argue that in most of the cases, it is the patients who flop to stick to their medication for various reasons. In some rare cases, the patients go to their assigned hospitals only to be told that their medicines are yet to arrive. Some studies also blame the medical practitioners who fail to emphasize to the patients the importance of adhering to the treatment without miscarrying (Bhatti et al., 2016). These factors limiting adherence to ART should be identified and eliminated to ensure that patients take their medication as oriented. The problem of non-adherence is one of the main reasons why the county has been leading in the new cases of HIV infections (Bhatti et al., 2016). The study will provide practical ways in which adherence to the treatment could be enhanced from 70% to the highest possible level (ideally 100%) to help in eliminating this epidemic.
Research Questions
The study will investigate the importance and means of enhancing adherence to HIV treatment as a way of fighting the pandemic. As such, it will be necessary to investigate adherence trends, reasons behind such trends, and ways in which it can be influenced to achieve the desired outcome. The researcher will rely on data that will be collected from the respondents and existing information available in books, journal articles, and trustworthy online sources. It is important to come up with research questions that will help in the process of collecting data from these sources. The following are the research questions that will guide this study:
- How does adherence to ART regimen help in the fight against HIV both for the infected and the uninfected persons?
- What are the fundamental reasons that lead to patients’ failure to adhere to their ARV treatment plans?
- What can be done by the health system, the medical providers, the nurses, the case managers, the social workers, the mass media, the local governments, the state government and institutions, and the society in general to enhance adherence to regular treatment among patients who are diagnosed with HIV/AIDS?
- What can be done or proposed to increase the community level of knowledge and awareness on these topics to finally decrease the level of newly infected cases in Miami-Dade every year and to improve the percentage of early diagnosis?
Limitations
When conducting this study, it is expected that several challenges will be encountered that may affect the ability to collect and analyze the required data within the right time. One of the biggest challenges in this study is the fact that it involves dealing with human subjects. Unlike inanimate objects that can be manipulated as per the desires of the researcher, human subjects must be handled based on their willingness to participate in the study. It was not easy finding the right participants to take part in this study. It can be time-consuming to identify and reach out to these participants to be part of the research. Most of the local hospitals are bound by the policy of patient-doctor confidentiality policy that makes it impossible to obtain a list of HIV positive patients in the region. The only way of reaching out to them is to use mass and social media and make a plea that those who are HIV positive should accept being participants in the study. It is not guaranteed that the message will reach the desired audience within the right time.
It is not also guaranteed that those targeted will be ready to be part of the research even if they get the information within the right time. As Helms et al. (2017) observe, most of these patients often consider their condition private and prefer not to reveal it to third parties. It means that it would be very difficult to identify these patients. The process might also take a very long time because the participants will need to be reassured that their identity will be kept anonymous. Günthard et al. (2016) argue that not all patients are truthful when reporting their level of adherence to antiretroviral drugs, especially when they are not talking to their doctors. That is a big challenge because it is possible to collect misleading data, especially when a patient deliberately lies that he or she is sticking to the medication while that is not the case.
Delimitations
In this study, the researcher can’t avoid human participants. Despite the above challenges, it was necessary to find ways of obtaining reliable data about the level of adherence to ARV therapies among the local HIV patients in Miami Dade County. In this academic research, time was of great essence. As such, we could not afford the long wait that would be necessary if data have to be collected from these patients. The financial burden of reaching out for these patients through mass and social media was beyond the budget of this study. The researcher decided to use data from various medical facilities and government databases within the county. Data from these sources do not identify specific patients by name but age, gender, race, sexual orientation, and other demographical factors relevant in this study. Reaching out to the management of these facilities and convincing them to release the data is not easy; however, the process is easier and more accurate than reaching out to the individual patients. This approach will also eliminate the problem of misinformation that may arise when patients deliberately provide misleading answers. In most of the cases, patients are always truthful to their doctors, as Montaner et al. (2014) state, because they want relief from their medical problem.
Definitions of Terms
It is important to explain all the technical terms and phrases that may not be clear to readers who do not specialize in any of the medical fields. The following words and phrases are used across the entire paper:
- Adherence. In medicine, adherence refers to strict compliance with the advice and medication/drug prescribed by the doctor (Ruan et al., 2017). In this paper, it is used to refer to the ability of a patient to take HIV medication at the right time, in the right manner, and regularly as prescribed by a doctor. Failure to comply with the directive is referred to in this paper as non-adherence. It may be a situation where a patient fails to take his or her medicine at the right time or regularly as advised by a doctor.
- HIV. It refers to the human immunodeficiency virus, a lentivirus, which is a subgroup of the retrovirus, responsible for causing HIV infection (Denison et al., 2016). The virus can be transmitted from an infected person to a healthy individual through sex, sharing of sharp objects, mother-to-child infection, and blood transfusion among other factors.
- AIDS. Acquired immunodeficiency syndrome is a condition where the immune system within the body is progressively compromised by the HIV when the infection drives to the CD4 count’s reduction below 200 cells/uL and/or when the percentage of CD4among the different CD cells falls below 14, which makes it easy for life-threatening opportunistic diseases to thrive in the body (Tran et al., 2016). When HIV is not properly managed, it progresses into AIDS, which puts the life of the patient is a great danger.
- ARV. Antiretroviral drugs are medication meant to reduce viral load in the body to help the patient lead a normal life, by increasing their CD4 count and to reduce the chances of infecting other people with the virus (Gama & Koup, 2018). Sometimes it may be referred to as ART, which means antiretroviral therapy.
- Regimen. It refers to a prescribed course of treatment that can restore one’s health (Gama & Koup, 2018). In this paper, it refers to the prescription given to HIV patients.
- Viral load. It is a measure of viral particles that are present in an organism (Adams & Simon, 2016). In this case, it refers to the measure of HIV in a person’s bloodstream.
- Viral suppression. It refers to the reduction of one’s viral load to a level which it cannot be detected in the bloodstream, it is called “undetectable” viral load (Menamo, 2015).
- Undetectable viral load. It denotes a viral load <20 copies/mL (Menamo, 2015).
- CD4. It is the cell of the human immune system used by HIV to copy itself (Tran et al., 2016).
- PEP. It is a method to impede HIV infection once a recent potential exposure to the virus has occurred, which means starting taking antiretroviral meds within 72 hours of being possibly exposed to HIV to prevent becoming positive. It must be used solely as emergency prophylaxis (Mayer & Krakower, 2016).
- PrEP. Pre-exposure prophylaxis is a preventive tactic for HIV negative people who are at very high risk of acquiring the virus, either because their partners have the virus or their profession regularly exposes them to it. A medicine called Truvada is taken regularly to lower their chances of acquiring the virus; the prophylactic method should include the use of condoms and a periodic medical follow up (Mayer & Krakower, 2016).
- Epidemic. It is a wide-ranging manifestation of an infectious disease, which in this case is HIV, within a given community and a given interval of time (Wright & Carnes, 2016).
- Pandemic. The epidemic is extended in an outsized zone (Wright & Carnes, 2016).
Access plan
The primary goal of this research is to determine the most common arguments for the non-adherence to the antiretroviral medication in a sample of HIV positive individuals and to promote the total compliance with those treatments among the locals in Miami Dade County and by and large in the entire country. As such, the information that will be obtained in this study must be made available to those who may need it within the country or at a global level. The document will first go through peer-reviewing to enhance its validity. It will then be made available in the local health-related publications to ensure that professionals within the healthcare sector can have access to it. The document will also be made available on online platforms to enhance its accessibility to the global society.
Review of the Literature
Introduction
The global society has been battling HIV/AIDs pandemic for over the last three decades. Millions of lives have been lost, children have been orphaned over that period, jobs lost, and the society has spent billions of dollars to find ways to stop the spread of the virus and its consequences. Kaplan (2014) states that despite the massive investment and time that has been dedicated by medical researchers and practitioners to find a cure for this infection, very little has been achieved. It is also very saddening that these researchers are yet to come up with vaccination that can help in protecting the population that remains not infected with the virus. However, Rhodes (2014) observes that the hard work of medical researchers has resulted in the emergence of ways of managing the problem among those living with the virus.
The introduction of antiretroviral therapies was one of the most important milestones that were achieved by medical researchers. Before their creation, being diagnosed with the virus was a sure death sentence because there were no ways of managing the problem (Gitterman, 2014). However, the emergence of the ART was a major accomplishment in the path towards managing this problem. Currently, scientific studies have shown that when one adheres to the antiretroviral treatment as prescribed by a doctor, he or she can lead a normal life for several years, just like a healthy person (Givens & Neilson, 2014). Complying with the treatment reduces the viral load in the body so significantly that it reduces or even eliminates chances that such a person can transmit the virus to an uninfected person (Muneer & Horenblas, 2016). Therefore, it is worrying that a section of those living with the virus fails to take their medication in time, posing a serious threat to themselves and other members of the society.
HIV Statistics in the United States
The United States is one of the developed nations that have made the most massive investment in the fight against HIV/AIDs for the last three decades. The prevalence of HIV among Americans is not as high as is the case in the majority of the developing economies, especially those in Africa (Crane, 2013). However, Elebo (2013) argues that one cannot ignore the fact that over 1.2 million Americans are currently living with the virus. Unfortunately, about 15% of this population in the country is not aware of their HIV status despite the state-of-the-art technologies that exist in the country’s healthcare sector (Feldman, Polverino, & Ramirez, 2014). This population stands the greatest chance of spreading the infection to other people within the country without their knowledge.
Appendix B provides detailed statistics of the current state of HIV infections in the country ordered by pathways through which the virus is acquired. The statistics show that from 2008 to 2014, the rate of new infections fell from over 45,700 to 37,600, which is an 18% decline in the rate of new infections (Smithers, 2017). In the same period, there was a 56% decline in infection caused by instruments used to inject drugs, a 36% drop among heterosexuals, 26% drop among gays and bisexual men aged over 35 years, and an 18% drop among gays aged below 24 years. Gays and bisexual men are the most affected population, accounting for 70% (26,200) new infections in the year 2014 alone. They are followed by the heterosexuals at 23% (8,600), people who inject drugs at 5% (1,700), and gays who inject drugs at 3% (1,100) (Collins-Bride, 2017). It is important to note that mother-to-child infection has been reduced to almost zero because of the use of ARV meds and other modern technologies in the country. The number of those who get infected through blood transfusion and in accidents is also negligible because of the current technologies in the country.
Also, Appendix C identifies the incidence of new HIV infections in 2016 based on the ethnic group, gender, and sexual preference. As shown in the figure, the black male-to-male sexual contact led to the greatest number of new infections in 2016; a total of 10,223 new infections were diagnosed in that group that year (Long, Prober, & Fischer, 2018). Hispanic/Latino male-to-male sexual contact was second at 7,425 new infections during the mentioned period. White male-to-male contact came third at 7,390 new infections while Black women heterosexuals contact came fourth at 4,189. Black men, heterosexual contact registered 1,926 new infections, white women heterosexual contact had 1,032 new infections while Hispanic/Latino women heterosexual contact registered 1,025 new infections that year (Wilson, 2015). The trend shows that male-to-male sexual contact is the leading pathway through which the virus is passed from infected people to healthy individuals, and the African American males are the most affected group.
On the other hand, Appendix D shows reported new cases of infection in 2016 based on age. The statistics show that young adults aged 20-29 are the most affected population, with over 14,740 new cases of infection reported in 2016. Middle-aged men from 30-39 come second at 9,943 new infections, while those aged 40-49 registered 6,490 new infections. Individuals in the age bracket of 50-59 had 4,882 new infections, and those over 60 showed 1,930 new infections. The least affected group was teenagers aged 13-19, that listed 1,675 new infections that year (Crane, 2013). The report indicated that the behavioral pattern of people directly influences the rate of new infections.
HIV Statistics in Miami-Dade County
Miami Dade County is one of the most populated countries in the United States, with about 2,496,420 residents. The majority of the residents are Hispanic/Latino at 65% (Zimmerman, 2013). 17.1% are African Americans, 15.4% are whites, and 1.4% in Asians, while other races account for about 1.1%. The county is known for its beautiful beaches and good climate that attract both local and international tourists. The economy of Florida State has been growing impressively over the recent past. However, recent reports about the incidence and prevalence of HIV in the county are worrying (Pilapil, DeLaet, Kuo, Peacock, & Sharma, 2016). According to a report by Oates (2017), although the entire country has registered a consistent drop in cases of new HIV infections over the recent past, it is worrying that the statistics show that the problem is on the rise in Miami-Dade County in Florida. The problem in Miami-Dade County is replicated in the neighboring Broward and Monroe counties in Florida.
Appendix E shows the percentage of people engaged in various selected stages of the HIV care continuum in Monroe County, in Florida. The statistics illustrate the number and percentage of people engaged in each of the five continuums of HIV care. In the county, 658 people were diagnosed as living with HIV in 2014, which represents 100% of the infected people in the county. 627 people (95%) are in even care after their diagnosis. 421 people (64%) are retained in care while 400 (61%) are on ART (Hudelson & Cluver, 2015). 382 people (58%) have suppressed viral load because they adhered to the ART. Kaplan (2014) argues that the statistics in Miami-Dade County are grimmer than they are in Monroe County. Those diagnosed with the virus in 2014 were 1,122, which is almost twice as much as the population of the affected people in Monroe County.
According to a report by Rhodes (2014), of those living with the virus in Miami Dade County, 19.9% of them have been diagnosed with AIDs. It is a sign that these individuals are not adhering to their antiretroviral drugs, which makes it easy for their condition to worsen and increases their chances of passing the virus to healthy individuals. Just like in other parts of the county, male-to-male sexual contact is the leading cause of the spread of HIV in Miami-Dade County. As Temoshok (2016) notes, it is worrying that even after the effort of state and county governments to address this problem, the county has remained in the number one spot in terms of new cases of HIV infection. The rate of new infections in the county is higher than it is in any other part of the country.
History of Antiretroviral Treatment
According to Gama and Koup (2018), the history of HIV/AIDs is often traced back to Africa, although it is not clear where and when the pandemic started spreading to the rest of the world. A study by Kaplan (2014) suggests that the initial infections must have occurred in the early 1930s in Congo. The virus, which is common among chimpanzees, must have found its way into the human system. The report explains that in Congo, it was common for the locals to hunt chimpanzees for meat. It is believed that during such hunts, the blood of chimpanzees came into contact with fresh wounds sustained by the hunters, making it possible for the virus to find its way into the human body system (Neal, 2016). Since then, the virus spread quickly through sexual contact and the exchange of body fluids, especially during a blood transfusion.
In the United States, a 16-year old Robert Rayford was the first person to be diagnosed with AIDs in 1968 (Mayer & Krakower, 2016). It was not clear how the teenager acquired the virus because he had never received a blood transfusion and never left the Midwest by the time he was diagnosed with the virus (Hudelson & Cluver, 2015). It strongly suggested that the virus was already spreading in the country without the knowledge of the medical experts. By the time medical doctors developed a clear understanding of the virus in the early 1980s, it is estimated that over 300,000 people had been already infected with the virus, with the number of fatalities being unclear (Collins-Bride, 2017). By the mid-1990s, HIV/AIDs had become a major pandemic in the United States, claiming the lives of over 50,000 Americans in 1995 alone. About 50% of those who lost their lives in 1995 because of the pandemic were African Americans (Crooks & Baur, 2014). However, the number of deaths and the rate at which the virus is spread in the country has dropped significantly since the discovery and widespread use of antiretroviral drugs in the country.
The first drug for HIV, known as zidovudine was introduced in 1987 (Philpott, 2015). After a decade of further research, a more efficient treatment called highly active antiretroviral therapy (HAART) was introduced in 1997, which led to a decline in deaths from the disease by 47%. By 2002, a testing kit had been approved by the Food and Drug Administration (FDA) to help speed up and simplify the diagnosis of the disease (Philpott, 2015). The kit was 99.6% accurate. In the early years, people had to purchase drugs to manage their condition. However, the funding from the federal government and other non-governmental (charitable) organizations made it possible to make the drugs freely available for infected individuals. Once diagnosed with the virus, people are encouraged to visit their nearest health centers to start regular treatment to manage the viral load. Temoshok (2016) argues that initially, the biggest problem in managing HIV through ART was a social stigma. People with the virus were considered immoral and dangerous to the rest of the population. However, public awareness campaigns have made American society more tolerant, making it easy for people to go for drugs regularly. The current estimates show that about 80% of the HIV patients in the country strictly adhere to the antiretroviral treatment as a way of managing the condition and protecting their loved ones (Bernstein & McMahon, 2018). However, the 20% who are not adhering to their medication poses a serious threat to them and exposes their loved ones to the virus if they engage in unprotected sex.
Developed Researches
The developed researches can help in enhancing an understanding of the nature of the problem. Scholars have investigated the issue for years to find how to manage the problem and free the global society from the socio-economic and emotional pains associated with HIV/AIDS. McKinney et al. (2016) in their report titled Evaluation of pill counts adherence with self-reported adherence in assessing antiretroviral therapy behavior of women living with HIV at a faith-based clinic in Malawi looked adherence to antiretroviral treatment among women in faith-based clinics. The report found out that these women were more likely to adhere to their medication than the other population using normal clinics. It was established that in these faith-based clinics, these women get emotional support from their colleagues and relevant religious leaders. These women reported the least level of self-rejection and stigmatization from the people around them. The study also shows that sometimes they are reminded by their colleagues to stick to the drug and to go for more drugs in time.
Karim (2015), in a report titled Overcoming impediments to global implementation of early antiretroviral therapy, looked at the fundamental challenges that affect early detection of the disease and proper administration of antiretroviral treatment as soon as one is diagnosed. The study shows that although people know a lot about HIV, most of them often fear going for voluntary testing even if they suspect that they might have come in contact with the virus. They feel that they cannot withstand the idea that they may turn to be positive because of the stereotypes often associated with the disease. It outlines ways in which these barriers can be eliminated to enhance early detection and proper administration of the drugs. An article by Uusküla et al. (2018) titled Effects of counseling on adherence to antiretroviral treatment among people with HIV in Estonia: A randomized controlled trial focused on the relevance of counseling as a way of promoting adherence to the ART treatment. The study shows that, in most cases, people tend to reject their condition. They need psychological help to understand that they can live a normal life without feeling that their death is near. Proper counseling is critical, as the study suggests, in the fight towards enhancing adherence to antiretroviral therapy.
Bhatti et al. (2016), in their report titled Current scenario of HIV/AIDS, treatment options, and major challenges with compliance to antiretroviral therapy, looked at the statistics about HIV/AIDs around the world and challenges faced when it comes to compliance with the medication. They found out that a significant number of those who fail to adhere to the medication did not receive proper counseling when they were first tested. They did not get to accept their condition, and as such, continue to lead a reckless lifestyle. Such individuals harbor pain in their hearts and feel that they were unfairly punished by those who infected them. As such, they feel they also have to ‘punish’ others by spreading the virus to others indiscriminately. They fail to understand their in so doing, they risk increasing their viral load or getting new strains of HIV. Such cases hinder the fight against the pandemic in the country.
Theoretical Framework
In this section of the paper, it is important to look at the relevant theories that can make it possible to explain reasons why a section of the patients diagnosed of HIV fail to take their medication regularly as would be expected. One theory that may help in understanding the nature and cause of this problem is Erving Goffman’s theory of social stigma (Mayer & Krakower, 2016). This theory holds that stigma is often attributed to one’s behavior, reputation, or state of being that is socially discrediting. As such, the individual will be subject to rejection and stereotyping because of the perceived social gap. HIV was largely popularized as a dangerous disease that equals to the death sentence. It was also associated with undesirable sexual immorality as its main cause. As explained by this theory, those who were diagnosed with AIDs were largely rejected by society because they were considered immoral. Many viewed them as a threat to society because of their likelihood of transferring the virus to a healthy population. The fear of stigmatization has made many people avoid seeking medication as recommended. Some even fear going for voluntary testing, fearing the outcome. Those with the virus consider death as a better alternative to rejection so they fail to inform their loved ones about their condition and avoid the drugs for fear of others finding out that they are on treatment.
The concept of self-rejection can also help in explaining non-adherence to antiretroviral treatment among a section of those living with the virus. Gama and Koup (2018) define the concept as a feeling of being unaccepted and undesirable to society. Unlike the stigma that is perpetrated by others against an individual, self-rejection is an inner feeling that a person develops against self. A sense of being worthless builds up within such a person and it is common for one to contemplate death. The behavior of such individuals may be erratic and sometimes dangerous to them and the people around them. Such individuals find no reasons to take medicine regularly (Hudelson & Cluver, 2015). Self-rejection is believed to be one of the leading reasons why some people still fail to take their medication regularly.
Further Research
The findings from the review of the literature indicate that it is important to conduct further studies in this field to help eradicate the problem of new HIV infection in the country and the world at large. Non-adherence to the antiretroviral treatment has been identified as one of the major impediments towards the fight against HIV/AIDs. The theoretical framework above has identified stigmatization and self-rejection as some of the main reasons why some people fail to take their drugs regularly. Future studies should focus on finding ways of addressing stigmatization and self-rejection in the fight against this pandemic.
Methodology
Introduction to Research Design
The primary goal of this research, as explained in chapter one of this report, was to determine the significance of adherence to the antiretroviral treatment as a way of controlling and managing HIV. Through this study, it was important to discover the differences between genders and various ethnic groups in terms of what every gender or ethnic group declared as the causes that affect the most or the less their adherence to treatment. The study explained the reasons behind the current position that Miami-Dade County has had from 2014 to 2017 as the top county in the entire US in the number of new cases of HIV diagnosed per year. The current trend is worrying and it is a clear indication that enough is yet to be done in this county to address the problem. Books and journal articles may help shed light on this problem. However, it is critical to collect data from participants to help in understanding the current state of the problem (Picardi & Masick, 2013). The participants provided the most current information about the problem, measures that have been taken to address it, level of success or lack of it for that matter that has been experienced, and the way forward based on the investigations that have been conducted.
The information collected from these participants shed light into the five steps of the HIV Care Continuum (percentage of diagnosed individuals, percentage of individuals linked to proper care, percentage of individuals engaged in care, percentage of individuals under prescribed antiretroviral treatment, and percentage of clients who are virally suppressed) as practiced in the local healthcare centers (Tracy, 2013). This chapter set the stage through which the research questions in chapter 1 answered through the information that was collected from the participants. Given the goal and objectives of this study as presented in the research questions, the most appropriate design was considered to be descriptive statistics as explained in the section below.
Methodology
The most appropriate research design for this research based on the central focus of the investigation was a descriptive study. The approach primarily focused on a survey (Alsos, Eide, & Madsen, 2014). When investigating the role and rate of the adherence to the antiretroviral treatment in the control of HIV, it was important to collect data that would help in explaining the trend over a given period (Bernard, 2013). Data was needed to explain how well HIV positive patients adhere to their medication and how their adherence affects them and the county at large. A specific region, Miami Dade County, has been identified as the area of study. Primary data was collected from specific institutions within this county that would help provide a true and most current data on the level of adherence to treatment. The hospitals were trusted to have accurate information because of several reasons.
First, most HIV-positive patients living in the county often take their medicine from various health centers within the region. These facilities keep records and they know when a patient is due for the next dose. The researcher focused on getting permission from the director of the health care organization to access the records. The researcher wrote a letter to the director, explaining the purpose of the study and the need to access the records. A patient who fails to adhere to the treatment is easily determined when they fail to come for the next dose at the scheduled date. Secondly, these hospitals often test the viral load of their patients to determine how the medication helps in reducing the viral load. It means that they can state, with high levels of precision, the role of adherence to the antiretroviral medication in the management of HIV. Finally, these facilities (especially the doctors or nurses who regularly interact with these patients) can explain why some of the patients fail to comply with the treatment based on the reports they receive from them.
Description of Participants
The limited-time available for the study made it necessary to come up with a sample population from which primary data was collected. All the participants that were sampled for this study were medical practitioners who have been directly working with HIV patients (Brennen, 2013). The researcher used a stratified sampling method to identify a target population of 4 medical doctors, 4 advanced registered nurse practitioners, and 1 physician assistant. The population was chosen because AHF is one of the biggest HIV-specialized agency in the whole country and the one that is managing the bigger caseload in Miami at present (HIV GOV, 2018). It was the reason why the researcher believed that the numbers gotten from this agency could be considered very representative of what’s happening in the entire Miami-Dade County. The researcher provided opportunities to voluntary participants at these facilities. A sampling of the participants was done after obtaining permission from the management of the selected hospitals.
AIDS Healthcare Foundation (AHF) currently has several medical providers in its five different health care centers in Miami-Dade County (McNabb, 2015). The centers include Jackson North HCC, Mount Sinai HCC, Mercy Hospital HCC, Homestead HCC, and Liberty City HCC (Clinard, 2016). The participants were from these health care centers. It was important to ensure that the participants sampled are a clear reflection of the current American society. It means that about half of the participants should be male while the other half should be female. The researcher was keen to ensure that at least one white, one African American, and one Hispanics are part of the sample. The age of the participants should also vary. Having such a diversified group of participants in the study helped in identifying and eliminating any possible bias in the response that was be obtained.
Access of Permissions
It is an ethical requirement for a researcher to contact the management of these hospitals to seek permission before contacting the individual participants. As Card (2016) observes, in some cases, a hospital may have policies and regulations that must be observed by researchers keen on obtaining data from their employees. Obtaining the permission was critical because other than collecting data from the sampled participants, it was equally important to access information in the databases to identify the trend and patterns in HIV management and prevalence within the country within the past four or five years (Fowler, 2013). An official letter was written to each of the administrators in the five institutions explaining the goal and significance of the study, the need to collect data from the institution, and reasons why these institutions were selected within Miami Dade County. The letter was delivered to these administrators electronically. In cases where some of them took the time to respond, the researcher visited such facilities and made a formal request while there.
Data Collection Method/Procedure and Instruments
In this study, finding an appropriate method of collecting data was critical in ensuring that the needed information was obtained from the respondents. A survey, as explained above, was considered the most appropriate method of collecting data (Gbadamosi, 2016). After developing a sample, the researcher contacted them through the phone and explained the relevance of the study and the reasons why they were selected. With their approval, the researcher sent a set of questions that they were expected to answer. They were requested to send them back through the same online platform. The questions were both closed-ended and open-ended to facilitate quantitative and qualitative data analysis. Closed-ended questions made it possible to convert the opinions of the respondents into numeric that can be analyzed mathematically (Reis & Judd, 2014). For instance, the frequency of the reasons for non-adherence to medication was evaluated statistically. On the other hand, open-ended questions enabled respondents to provide justifications for their arguments whenever necessary (Nestor & Schutt, 2014). The instrument that was used in the process was a questionnaire. It helped in standardizing the response from the participants.
Methodological Assumptions
Methodological assumptions are necessary to ensure that this research was completed as per the plan. The following are the fundamental assumptions that were made in this study:
- The information received from the participants is true to the best of their knowledge and that none of them deliberately misguided the researcher.
- The existing scientific research has proven that adherence to antiretroviral drugs is critical when it comes to controlling HIV.
- The impact of visitors, including tourists who regularly frequent the beaches of Miami, is negligible when it comes to adhering to the HIV medication.
Data Processing and Analysis
Data obtained from the facilities were analyzed to help in informing the conclusion and recommendations that were made in this study (Skott & Ward, 2013). Analysis of data took two approaches because triangulation was necessary. The first approach was the quantitative analysis of the primary data collected from the respondents that captured the level or rate of non-adherence to antiretroviral medication among HIV patients. The regression analysis identified frequently mentioned reasons why these patients do not comply with their prescribed drugs (Bryman & Bell, 2015). In this analysis, the researcher converted opinions into numeric values using a Likert scale (Yanow & Schwartz-Shea, 2014). Using ANOVA, it was possible to identify the correlations of the factors and variance in adherence to the medication. The second approach to analyze the conglomerate of records from the facilities to understand the rare of non-adherence.
Results
Results and Analysis
Chapter for this paper focuses on the analysis of data obtained from the institutions involved in the management of HIV/AID within Miami-Dade County, as explained in the previous chapter. The survey was critical in ensuring that the most current data was obtained on this issue. Information obtained from secondary sources explained the importance of adherence to antiretroviral therapy in the control of HIV. It is worrying that a section of those infected with the virus in the county is not adhering to their medication (Maningat, Gordon, & Breslow, 2013). The question below focused on determining the primary reasons why these patients fail to take their medicine regularly.
What are the fundamental reasons that lead to patients’ failure to adhere to their ARV treatment plans?
Data obtained from the selected HIV/AIDs management institutions within Miami-Date County identified a host of issues that make it difficult for the patients to adhere to their medication as regularly as would be required. The figure below shows the identified issues:
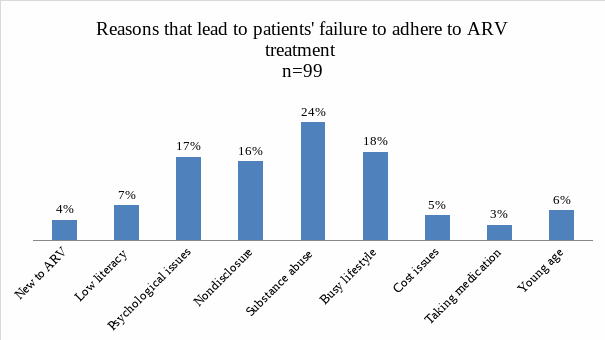
Reasons for Failure to Adhere to Medication
New to chronic disease management
One of the reasons that were identified as being a cause of non-adherence is being new to the antiretroviral disease. About 4% of the patients who fail to take their medication on time cited this reason. Once one is diagnosed with the virus, he or she will be put under medication immediately to help manage their condition. In many cases, these people find themselves in a situation where they suddenly have to start managing a chronic disease (Croome, Ahluwalia, Hughes, & Abas, 2017). Given that it was not part of their routine, they may miss taking their medication once in a while. The problem was more common among younger HIV patients than it was among the middle-aged and the aging population. It is important to note that the problem became less common among those who have been on antiretroviral therapies for over 12 months. It was a clear indication that as an individual continues to embrace antiretroviral therapies he or she becomes less likely to fail in taking their medication in time.
Low levels of health literacy and health responsibility. A section of the patients demonstrated limited health literacy levels in terms of their explanation of their failure to adhere to their medication. It was evident from the records that 7% of the patients fail to take their medication regularly because of the limited knowledge they have about the disease. HIV/AIDS as a topic has been on public discourse for decades (Liamputtong, 2013). In the United States, it is part of the syllabus at various stages of learning. Whenever contraceptives are discussed, HIV infection is always one of the main reasons given why they should be used by sexually-active individuals. Therefore, it would be expected that sexually-active Americans have the right knowledge about this health problem (Axelsson, Hallager, & Barfod, 2015). However, the statistics show that a small percentage of the population still have distorted information on how to manage the disease. Some of them stated that they visited their pastors who prayed for them and assured them that they are healed, hence they stopped their medications. Others stated that they resorted to traditional medication as a way of permanently treating the disease instead of taking ARVs that only manage the condition. Such answers indicate that it is necessary to conduct further HIV awareness among the locals to fight illiteracy and misconceptions.
Psychological issues. Some of the fundamental causes of non-adherence to HIV treatment among patients within Miami-Dade County are psychological problems. The records obtained from the facilities indicate that 17% of the patients who do not take their medication as prescribed have psychological problems (Liamputtong, 2013). Denial is one of the major psychological problems, especially among those who have just been diagnosed with the disease. Within the first few days or months of gaining knowledge about their status, these patients find it difficult to accept their conditions (Mathibe, Hendricks, & Bergh, 2015). They feel that there was a mistake in the diagnosis. They avoid taking the medicine hoping that their next tests would reveal that they are negative. With time, they get to accept their condition. Depression is another psychological problem that comes soon after the denial stage. At this stage, the patient develops a deep sense of loss. They feel that they are of no value and find no reason for taking their medication.
The stage is very dangerous because a patient may become reckless in their actions. Some may want to spread the virus to as many people as possible because of various selfish reasons. Others may contemplate taking their own life because of their inability to face the reality and deal with it. Low social support may also have a psychological impact on a patient. People diagnosed with cancer often receive sympathy and support from society. The same is not the case with those diagnosed with HIV. Revealing such status would lead to one losing close friends as they are considered a threat. The psychological trauma that comes with the rejection and stereotyping may be so great that adhering to the medication becomes a major problem. Some of them fail to visit the clinics because of the feeling that they might meet people they know at these facilities.
Nondisclosure of HIV status. Accepting the fact that one is HIV-positive is still one of the biggest challenges in the fight against this pandemic. Statistics show that 16% of the respondents fail to take their medication regularly because of the non-disclosure of HIV status. These are patients who are keen on hiding their HIV status to people close to them, sometimes including their sex partners. Some of these patients explained that they would insist on using protective sex with these partners without explaining the reason as a way of protecting them from the virus. During the period they are with these loved ones, they may be forced to hide their medicine, only taking them when they are certain they are alone. These patients value social status so much that they may risk their health to protect it (Schaecher, 2013). The problem was identified to be common among the rich and the working class within the society. Some stated that revealing their status may lead to serious marginalization at the workplace. The fear of one losing his or her job or close friends forces them to hide their status to the extent that they fail to adhere to their medication.
Substance abuse issues. Substance abuse tops the list of causes of non-adherence to HIV therapy among HIV patients in Miami-Dade County. Statistics show that 24% of the cases of non-adherence to antiretroviral therapy are due to drug abuse. According to Hall (2014), drug abuse in Miami-Dade County is a common socio-economic problem that the government has been trying to deal with for decades. Some of the HIV patients in this county are drug and alcohol addicts. After taking these drugs, they become mentally-impaired. They do not remember to take their medication at the prescribed hour. Some miss their dosage for several days when hospitalized for various medical problems relating to drug abuse.
Busy or irregular lifestyle. Some of the patients have very busy schedules that limit their capacity to adhere to their medication. Data collected shows that this problem is responsible for 18% of cases of non-adherence to the medication. Some are forced to stay in the office or conferences for long hours that they skip their medication once in a while (Dipirro, 2015). The problem was common among corporate employees, especially in the finance and marketing sectors. Young adults who attend evening classes after work were also more likely to fail to take their medicine than their colleagues who are not attending evening classes.
Cost and insurance issues. A few of the respondents, about 5%, cited issues relating to costs and insurance. For a long time, most of the insurance providers avoided covering HIV because of the belief that they have a shorter lifespan compared with those who are not infected. When one is forced to pay for his or her medical bills from the pocket, the pressure may sometimes be unbearable to them.
Difficulty with taking medication. A significantly small portion of the patients (3%) often cited difficulty with taking medication as their reason for failing to take medicine in time. Some claim that the size of the medicine and the reason why they take it is a major hindrance. The problem became less common among those who have been taking the medicine for a while.
Young age. Unfortunately, some young individuals find themselves infected with the virus through various means. Many of them rely on the support of their parents or people close to them to take their medication as required. 6% of the patients in this county cite this as one of the main problems they find when trying to adhere to antiretroviral therapies. The problem was more common among patients below 16 years.
What can be done to enhance adherence to regular treatment among patients who are diagnosed with HIV/AIDS?
The fundamental reasons why some HIV patients fail to adhere to the antiretroviral medication has been outlined in the section above. Finding solutions involve addressing these issues. In this question, the researcher sought to determine how the issue can be addressed based on the information available in the health institutions visited. The figure below shows the outcome of the analysis of their responses.
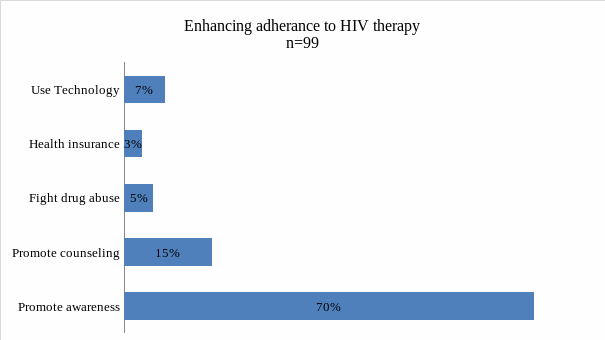
Patients who adhere to the antiretroviral medication often have their viral load reduced to undetectable levels that enable them to lead a normal life, just like uninfected individuals. It was important to find ways of fighting non-adherence among HIV patients in Miami-Dade County and the country at large. The following were some of the main ways identified to help promote adherence to the medication.
Promoting Adherence to the Medication
Promote awareness. An overwhelming majority stated that awareness creation is one of the most important ways of promoting adherence. People need to understand that beyond any form of prejudice in the society, tight schedule at work, difficulty in taking medication, or psychological problems, they have a responsibility to maintain good health. They must know that their ability to overcome this health problem depends largely on their attitude.
Promote counseling. It also emerged that registered nurses and doctors handling patients should ensure that their patients go through proper counseling to help them deal with their condition. Sometimes they may need the help of a psychologist, especially for patients who are going through denials and depression (Shapshak, Levine, Foley, Somboonwit, & Singer, 2017). Psychological support plays a critical role in enhancing the level of adherence to the medication.
Fight drug abuse. The society should unite in the fight against drug and alcohol abuse. The study has shown that HIV patients tend to be more reckless with their lives and less likely to adhere to a medication when they are drunk than when they remain sober. It is necessary to reduce substance abuse among these patients as much as possible.
Health insurance. The government should ensure that all health insurance providers in the country do not discriminate against HIV patients. The cost of medication should be affordable to everyone irrespective of one’s social status.
Use of Technology. It may be necessary to use technology to help in constantly reminding the patients to stick to their medication. Patients can join online groups where their identity can be protected so that they can get social support and be reminded regularly to take their drugs.
What can be done or proposed to increase the community level of knowledge and in Miami-Dade County?
The community has a role to play in ensuring that HIV patients in Miami-Dade County adhere to their ART treatment to help fight this pandemic. One of the biggest responsibilities of the society, as stated by the medical practitioners, is to fight discrimination against infected individuals. The perception that those with the virus are immoral and a danger to society should stop (Storey et al., 2014). Instead, these people should get the social and economic support they need from the people around them. The society also needs to talk about the benefits of these drugs and the need to take them for those infected. People taking these drugs do not need sympathy. They need understanding and normal treatment. They should be made to feel that they can overcome challenges associated with the virus if they stick to their ART therapies.
How does adherence to ART regimen help in the fight against HIV both for the infected and the uninfected persons?
The participants (nurses and doctors) stated that when taken as per the prescriptions, ART reduces the viral load to undetectable levels (<40 copies/mL). Viral suppression within the body means that the affected individual can lead a normal life because the immune system will be strong enough to fight opportunistic diseases (Sebong, Sulistio, & Mahendradhata, 2017). When the viral load is low, the chances of an infected person passing the virus to a healthy individual is low. It means that cases of new infections, which are currently higher in Miami-Dade County than anywhere else in the country, will be reduced.
Summary
Adherence to antiretroviral therapies is defined as the ability of a patient to take his or her medicine at the right time, in the right manner, and to follow all the recommendations that may be provided by the doctor such as dieting and regular exercise. The study found out that the majority of residents of Miami-Dade County (about 70%) adhere to the ART treatment. It means that the rate of non-adherence in the county is 30%. Primary data collected from the identified healthcare institutions identified several factors that cause non-adherence to antiretroviral treatment. Drug and alcohol abuse was one of the main reasons. Regular illicit drug users are more likely to fail in taking their drugs regularly than those who avoid drugs. Individuals with very busy schedules were also more likely to miss their daily dose of the drug once in a while. Some of these patients cited forgetfulness as one of the reasons why sometimes they fail to take drugs (Alistar, Long, Brandeau, & Beck, 2014). Non-disclosure of HIV status, psychological factors such as denial and depression, age, and low literacy levels were the other hindrance identified. The study strongly suggests that these issues must be identified. The medical practitioners interviewed argue that the entire society has a role to play in this fight, including those who are not infected with the disease. The war against HIV/AIDS cannot be won if these patients fail to adhere to their medication as expected.
Conclusion
Managing HIV/AIDS is one of the biggest financial burdens that the United States has to deal with in every financial year. The government spends money on hiring more medical practitioners to handle the patients, on ARVs, and research. Families are also affected, especially when the breadwinners are unable to go to work because of the disease. The highest number of new cases of HIV infection has been registered in Miami-Dade County for the past three years consecutively. Unfortunately, the efforts put in place by the county and state government to fight the epidemic in the county have not yielded the desired outcome. The county is known for its popular beaches that attract tourists from all over the world and the current statistics about new HIV infections are worrying. Non-adherence to ART treatment has been identified as one of the reasons why the spread of the virus is high in this region. Most of the patients who fail to take their medicine in time cite drug use, busy work schedule, forgetfulness, young age, low literacy levels, and fear of social stigma among other factors as reasons why they are not consistent when it comes to taking their medicine as prescribed by their doctors. Discrimination is currently one of the main factors that affect the ability to fight this pandemic. The society must understand that a proper solution can only be realized if a united approach against the problem is embraced. Cases of discrimination should be eliminated. Proper public education is needed and all stakeholders must appreciate the fact that regardless of their HIV status, the problem affects everyone either directly or indirectly.
Implication for Practice
The study clearly shows that nurses and doctors who manage HIV patients have a major role to play in fighting the HIV epidemic. It is worrying that in the modern American society where information is readily available in the digital platform some people still have limited knowledge about this disease. Blaming the patients for their failure to take medication may not solve the current problem. Nurses and doctors need to find ways of educating these patients to ensure that they do not resort to traditional or spiritual means of managing the virus. The society also needs sensitization to ensure that they understand their role in fighting the spread of HIV. Nurses should work closely with psychologists to ensure that patients are properly counseled to enable them to deal with their unique medical conditions.
Recommendations
Non-adherence to antiretroviral therapies is a major challenge in the fight against the spread of HIV. Stakeholders in Miami-Dade County must now face the reality that cases of new infection are highest in their county than anywhere else in the country. The following recommendations should be taken into consideration:
- The county government, working closely with the medical practitioners, should use both mass and social media to sensitize the society about the importance of adherence to ART in the fight against HIV.
- Public awareness campaigns should also focus on fighting stigmatization and discrimination of HIV positive people to help enhance adherence to ART treatment.
- Antiretroviral drugs should be made available to all infected individuals in an affordable manner.
- Further research in the field of HIV/AIDS management and treatment is critical to find ways of treating patients and vaccinating healthy people against the virus.
References
Adams, L., & Simon, J. (2016). The need for multi-level mitigation of medical mistrust: Comment on Bogart et al. (2016), medical mistrust among social network members may contribute to antiretroviral treatment non-adherence in African Americans living with HIV. Social Science & Medicine Journal, 159(1), 58-60. doi:10.1016/j.socscimed.2016.04.025
Alistar, S. S., Long, E. F., Brandeau, M. L., & Beck, E. J. (2014). HIV epidemic control—a model for optimal allocation of prevention and treatment resources. Health Care Management Science, 17(2), 162-81.
Alsos, A., Eide, D., & Madsen, L. (2014). Handbook of research on innovation in tourism industries. Berlin, Germany: McGraw Hill.
Axelsson, J.M., Hallager, S., & Barfod, T.S. (2015). Antiretroviral therapy adherence strategies used by patients of a large HIV clinic in Lesotho. Journal of Health, Population and Nutrition, 33, 10.
Bernard, H. (2013). Social research methods: Qualitative and quantitative approaches. Los Angeles, CA: SAGE Publications.
Bernstein, M., & McMahon, K. (2018). Nutrition across life stages. Burlington, MA: Jones & Bartlett Learning.
Bhatti, A., Usman, M., & Kandi, V. (2016). Current scenario of HIV/AIDS, treatment options, and major challenges with compliance to antiretroviral therapy. Cureus, 8(3), e515. doi:10.7759/cureus.515
Brennen, B. (2013). Qualitative research methods for media studies. Oxford, UK: Oxford University Press.
Bryman, A., & Bell, E. (2015). Business research methods. Oxford, UK: Oxford University Press.
Card, A. (2016). Applied meta-analysis for social science research. New York, NY: The Guilford Press.
Clinard, M. B. (2016). Sociology of deviant behavior. Boston, MA: Cengage Learning.
Cohen, M., Chen, Y., McCauley, M., Gamble, T., Hosseinipour, M., Kumarasamy, N., … Hakim, J. (2016). Antiretroviral therapy for the prevention of HIV-1 transmission. The New England Journal of Medicine, 375(1), 830-839. doi:10.1056/NEJMoa1600693
Collins-Bride, G. M. (2017). Clinical guidelines for advanced practice nursing: An inter-professional approach. Burlington, MA: Jones & Bartlett Learning.
Crane, J. (2013). Scrambling for Africa: AIDS, expertise, and the rise of American global health science. Ithaca, NY: Cornell University Press.
Crooks, R., & Baur, K. (2014). Our sexuality. Belmont, CA: Wadsworth/Cengage Learning.
Croome, N., Ahluwalia, M., Hughes, L., Abas, M. (2017). Patient-reported barriers and facilitators to antiretroviral adherence in sub-Saharan Africa. AIDS, 31(7), 995-1002.
Denison, J., Koole, O., Tsui, S., Menten, J., Torpey, K., Praag, E., … Mukadi, Y. (2016). Incomplete adherence among treatment-experienced adults on antiretroviral therapy in Tanzania, Uganda and Zambia. AIDS, 29(3), 361–371. doi:10.1097/QAD.0000000000000543
Dipirro, D. (2015). The positively present guide to life: How to make the very best of every moment. London, UK: Watkins Media Ltd.
Elebo, C. (2013). The defeat of the once-deadly disease: HIV/AIDS. Bloomington, IN: Xlibris.
Feldman, C., Polverino, E., & Ramirez, J. A. (2014). Pulmonary complications of HIV: European respiratory monograph 66. Sheffield, UK: European Respiratory Society.
Fowler, F. (2013). Survey research methods. Thousand Oaks, CA: SAGE Publications.
Friedman, R., Stall, R., Plankey, M., Wei, C., Shoptaw, S., Herrick, A.,… Surkan, P. (2016). Effects of syndemics on HIV viral load and medication adherence in the multicenter aids cohort study. The Journal of Clinical Pharmacology, 29(9), 1087–1096. doi: 10.1097/QAD.0000000000000657
Gama, L., & Koup, R. (2018). New-generation high-potency and designer antibodies: Role in HIV-1 treatment. Annual Review of Medicine, 69(1), 409-419.
Gbadamosi, A. (2016). Handbook of research on consumerism and buying behavior in developing nations. Hershey, PA: Business Science Reference.
Gitterman, A. (2014). Handbook of social work practice with vulnerable and resilient populations. New York, NY: Columbia University Press
Givens, T., & Neilson, L. (2014). The Columbia sourcebook of Mormons in the United States. New York, NY: Columbia University Press.
Günthard, H., Saag, M., Benson, C., Rio, C., Eron, J., Gallant, J., … Hoy, J. (2016). Antiretroviral drugs for treatment and prevention of HIV infection in adults: 2016 recommendations of the international antiviral society–USA panel. The Journal of the American Medical Association, 316(2), 191-210. doi:10.1001/jama.2016.8900
Hall, J.N. (2014). Drug abuse trends in Miami-Dade and Broward Counties, South Florida: 2014. Web.
Helms, B., Turan, J., Atkins, G., Kempf, M., Clay, O., Raper, J., … Mugavero, M. (2017). Interpersonal mechanisms contributing to the association between HIV-related internalized stigma and medication adherence. AIDS and Behavior, 21(1), 238–247.
HIV GOV. (2018). Data and trends: U.S. statistics. Web.
Hudelson, C., & Cluver, L. (2015). Factors associated with adherence to antiretroviral therapy among adolescents living with HIV/AIDS in low- and middle-income countries: A systematic review. Psychological and Socio-Medical Aspects of AIDS/HIV, 27(7), 805-816. doi.org/10.1080/09540121.2015.1011073
The Insight Start Study Group. (2015). Initiation of antiretroviral therapy in early asymptomatic HIV infection. The New England Journal of Medicine, 373(1), 795-807. doi:10.1056/NEJMoa1506816
Kaplan, L. (2014). People living with HIV in the USA and Germany: A comparative study of biographical experiences of chronic illness. Wiesbaden, German: Springer.
Karim, S. (2015). Overcoming impediments to global implementation of early antiretroviral therapy. The New England Journal of Medicine, 373(1), 875-876. doi:10.1056/NEJMe1508527
Liamputtong, P. (2013). Stigma, discrimination and living with HIV/AIDS: A cross-cultural perspective. New York, NY: Springer.
Long, S., Prober, C., & Fischer, M. (2018). Principles and practice of pediatric infectious diseases. Philadelphia, PA: Elsevier.
Maningat, P., Gordon, P.R., Breslow, J.L. (2013). How do we improve patient compliance and adherence to long-term statin therapy? Current Atherosclerosis Reports, 15(1), 291.
Mathibe, M. D., Hendricks, S. J. H., & Bergh, A. (2015). Clinician perceptions and patient experiences of antiretroviral treatment integration in primary health care clinics, Tshwane, South Africa: Original research. Curationis, 38(1), 1-11.
Mayer, K., & Krakower, D. (2016). Editorial commentary: Can we afford to control the HIV epidemic with antiretroviral? Can we afford not to do so? Clinical Infectious Diseases, 63(11), 1505–1507.
McKinney, O., Pearce, D., Banta, J., Mataya, R., Muula, A., Crounse, J., … Mukaire, P. (2016). Evaluation of pill counts adherence with self-reported adherence in assessing antiretroviral therapy behavior of women living with HIV at a faith-based clinic in Malawi. HIV Current Research, 1(3), 1-6.
McNabb, D. (2015). Research methods for political science: Quantitative and qualitative methods. New York, NY: M.E. Sharpe.
Menamo, E. D. (2015). Impact of household food insecurity on adherence to antiretroviral therapy (ART) among urban PLHIV: The case of Hawassa City, SNNPR State, Ethiopia. Hamburg, Germany: Anchor Academic Publishing.
Montaner, J., Lima, V., Harrigan, R., Lourenço, L., Yip, B., Nosyk, B., … Wood, E. (2014). Expansion of HAART coverage is associated with sustained decreases in HIV/AIDS morbidity, mortality and HIV transmission: The HIV treatment as prevention experience in a Canadian setting. Public Library of Science, 9(2), 87872. doi:10.1371/journal.pone.0087872
Muneer, A., & Horenblas, S. (2016). Textbook of penile cancer. Cham, Switzerland: Springer.
Neal, Z. (2016). Handbook of applied system science. London, UK: Taylor & Francis Group.
Nestor, P., & Schutt, R. (2014). Research methods in psychology: Investigating human behaviour. Thousand Oaks, CA: SAGE Publications.
Oates, E. (2017). Mending broken branches: When god reclaims your dysfunctional family tree. Grand Rapids, MI: Kregel Publications.
Philpott, D. (2015). Critical government documents on health care. Lanham, MD: Bernan Press.
Picardi, C. A., & Masick, K. D. (2013). Research methods: Designing and conducting research with a real-world focus. Thousand Oaks, CA: SAGE Publications.
Pilapil, M., DeLaet, D. Kuo, A., Peacock, C., & Sharma, N. (2016). Care of adults with chronic childhood conditions: A practical guide. Cham, Switzerland: Springer International Publishing.
Reis, H., & Judd, C. (2014). Handbook of research methods in social and personality psychology. Cambridge, UK: Cambridge University Press.
Rhodes, D. (2014). Innovations in HIV prevention research and practice through community engagement. New York, NY: Springer.
Ruan,Y., Xiao, X., Chen, J., Li, X., Williams, A., & Wang, H. (2017). Acceptability and efficacy of interactive short message service intervention in improving HIV medication adherence in Chinese antiretroviral treatment-naïve individuals. Patient Prefer Adherence, 11(1), 221–228. doi:10.2147/PPA.S120003
Sabin, L., DeSilva, B., Gill, C., Li, Z., Vian, T., Wubin, X., … Feng, C. (2016). Improving adherence to antiretroviral therapy with triggered real time text message reminders: The China through technology study. Journal of Acquired Immune Deficiency Syndromes, 69(5), 551–559. doi:10.1097/QAI.0000000000000651
Schaecher, K.L. (2013). The importance of treatment adherence in HIV. American Journal of Managed Care, 19(12), 231-7.
Sebong, P., Sulistio, D., & Mahendradhata, Y. (2017). Sustainability capacity of HIV/AIDS programs in Yogyakarta, Indonesia. International Journal of Public Health Science, 6(4), 314-323. doi:10.11591/ijphs.v6i4.pp314-323
Shapshak, P., Levine, A. J., Foley, B. T., Somboonwit, C., & Singer, E. (2017). Global virology II – HIV and neuro-AIDS. New York, NY: Springer.
Skott, B., & Ward, M. (2013). Active learning exercises for research methods in social sciences. Thousand Oaks, CA: SAGE Publications.
Smithers, G. D. (2017). Science, sexuality, and race in the United States and Australia, 1780-1940. Lincoln, UK: University of Nebraska Press
Storey, D., Seifert-Ahanda, K., Andaluz, A., Tsoi, B., Matsuki, J., & Cutler, B. (2014). What is health communication and how does it affect the HIV/AIDS continuum of care? A brief primer and case study from New York City. Journal of Acquired Immune Deficiency Syndromes, 15(66), 241-9.
Temoshok L. (2016). Adherence to antiretroviral therapy among patients attending an inner-city HIV primary care clinic: Non-obvious factors are most important. Journal of Human Virology & Retrovirology, 4(1), 1-8. doi:10.15406/jhvrv.2016.04.00121
The Temprano ANRS 12136 Study Group. (2015). A trial of early antiretroviral and isoniazid preventive therapy in Africa. The New England Journal of Medicine, 373(1), 808-822. doi: 10.1056/NEJMoa1507198
Tracy, S. J. (2013). Qualitative research methods: Collecting evidence, crafting analysis, communicating impact. Chichester, UK: Wiley-Blackwell.
Tran, B., Hwang, J., Nguyen, L., Nguyen, A., Latkin, N., Tran, N., … Thuc, V. (2016). Impact of socioeconomic inequality on access, adherence, and outcomes of antiretroviral treatment services for people living with HIV/AIDS in Vietnam. PLOS One, 4(1), 1-6.
Uusküla, A., Laisaar, K., Raag, M., Lemsalu, L., Lõhmus, L., Rüütel, K., … Amico, R. (2018). Effects of counseling on adherence to antiretroviral treatment among people with HIV in Estonia: A randomized controlled trial. HIV-Bridge Study Group, 22(1), 224–233.
Wilson, C. B. (2015). Remington and Klein’s infectious diseases of the fetus and newborn infant. Philadelphia, PA: Saunders publishers.
Wright, E. R., & Carnes, N. (2016). Understanding the HIV/AIDS epidemic in the United States: The role of syndemics in the production of health disparities. Cham, Switzerland: Springer International Publishing.
Yanow, D., & Schwartz-Shea, P. (2014). Interpretation and method: Empirical research methods and the interpretive turn. London, UK: M.E. Sharpe.
Zimmerman, Y. C. (2013). Other dreams of freedom: Religion, sex, and human trafficking. Oxford, UK: Oxford University Press.

