An immune system is a set of protective measures that deals with pathogens – external threats to the organism. Humans and other jawed vertebrates have a well-developed and complex system consisting of several levels. Despite its complexity, the system remains vulnerable to several conditions, including the secondary immunodeficiency, with HIV being one of its most widespread causes.
The immune system of humans is usually viewed as comprised of two levels. The first is known as a non-specific, or innate immune system. It provides the immediate and non-specific protection from the pathogens such as bacteria, viruses, and parasites (Paul, 2012). The first component of the innate immune system is the physical barriers, such as skin, saliva, secretion of the gastrointestinal system, mucus, and the texture of the inner surface of lungs. They prevent the pathogens from entering the human body mechanically and chemically. If these defenses are bypassed, the next component, known as cell-mediated immunity, is activated. The two cells most often associated with the non-specific immunity are macrophages and natural killer cells. The former are the most wide-spread types of leukocytes (50 to 60% of total number) and target the foreign agent by producing the relevant chemicals which allow them to phagocytize the unknown pathogen (Paul, 2012). The latter target the cells which do not fit the recognizable pattern (e.g. the tumor cell or a cell infected by a virus) and destroy them.
All of the cells comprising the non-specific system are versatile and act immediately upon the location of the pathogen, but can be relatively ineffective in certain situations. Besides, the leukocytes do not have immunological memory, which means the response to the same pathogen will be the same in duration and efficiency each time. Finally, the inflammation is another part of a non-specific system. It results from the release of the eicosanoids and cytokines by the damaged cells and results in swelling, redness, and increased blood flow. The inflammation process attracts the leukocytes to the site of damage and alters some of the cellular processes, such as protein synthesis and growth rate, decreasing viral activity and boosting regeneration of tissue.
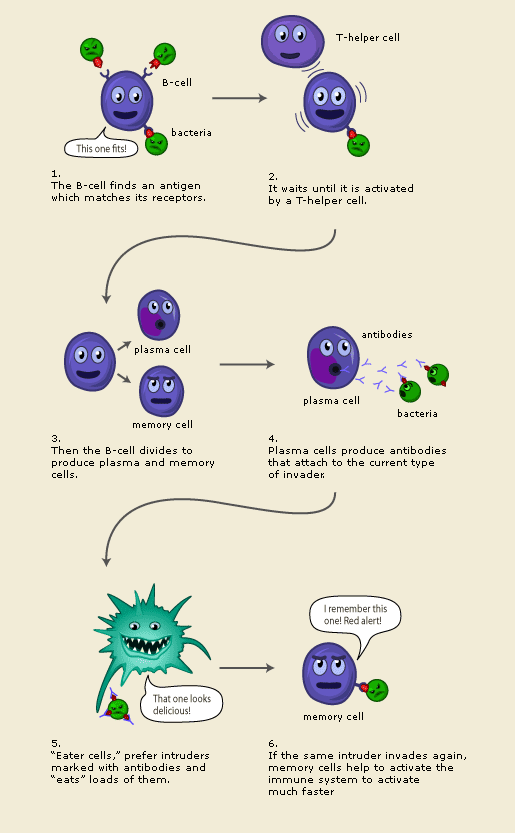
While the innate system is widely present in living organisms, the second level, known as specific, or adaptive immune system, is unique to jawed vertebrates, including humans (Acton, 2013). The adaptive system reacts to certain pathogens in a unique way and utilizes the humoral, or antibody-mediated immunity in addition to the cell-mediated one. The latter is primarily executed by the lymphocytes, more specifically, by the variety known as the Killer T-cells. These cells act in the same way as the NK cells but target only the cells which match the previously formed receptor instead of all of the cells that deviate from the norm. The efficiency of the specific cell-mediated response is higher due to the narrower focus but demands some time to form a receptor and produce the needed number of the Killer T-cells. On the other hand, the process has the immunological memory, so after the one-time exposure, the killer T-cells remain active in the organism, guaranteeing the decreased time of response in consecutive exposures. The antibody-mediated immunity is provided by the B-cells which produce the molecules known as antibodies. The antibodies can inhibit viral activities by restricting the interactions between the host cells and pathogens and transfer the information required for the killer T-cell generation. The information is carried by the Helper T-cells, involved in both the cell-mediated and antibody-mediated immunity.
The disorders of the immune system can be grouped in two categories. If the immune system is overactive, the leukocytes designed to attack foreign pathogens begin targeting healthy cells. This condition is known as autoimmunity. The examples of autoimmune disorders include rheumatoid arthritis, psoriasis, lupus, and diabetes mellitus type 1, among others. If on the other hand, the immune system is not active enough, this results in the immunodeficiency, when the response to the pathogens is either not strong enough or, in severe cases, absent (Ochs, Smith, & Puck, 2013). As a result, the organism becomes vulnerable to diseases. The immunodeficiency may be hereditary, or primary, but is more often acquired. The most recognized cause of secondary immunodeficiency is the human immunodeficiency virus (HIV). HIV impacts a certain variety of helper T-cells, CD4+ T cells, which leads to their gradual decline (Emini, 2002). As the helper T-cells are a crucial part of both the cell-mediated and antibody-mediated immunity, once their amount falls beneath a certain level, the immunity of the organism is compromised. This results in the condition known as acquired immunodeficiency syndrome (AIDS), during which the humans become vulnerable to the wide variety of infections and cancers (Emini, 2002). In essence, the HIV targets the protective system of the organism, stripping it of the means to defend against other threats.
The immune system of humans is a complex and multi-layered. It can be divided into specific and non-specific parts, which are interconnected and complement each other by providing a generalized immediate response after the breach and a more effective and focused non-specific one which also has a long-term preventive measure known as immunological memory. While most of the health conditions are the result of ineffective immune response, some are the caused by the oversensitivity of the system, while still other, such as HIV, are essentially “attacking the defenders” by disrupting crucial parts of the immunity.
References
Acton, A. (Ed.) (2013). Issues in immunology research. Atlanta, GA: ScholarlyEditions.
Antibody-mediated immunity. (n.d.). Web.
Emini, E. (2002). The Human Immunodeficiency Virus: Biology, immunology, and therapy. Princeton, NJ: Princeton University Press.
Macrophage phagocytizes the pathogen [Image]. (n.d.). Web.
Ochs, H., Smith, C., & Puck, J. (2013). Primary immunodeficiency diseases: a molecular and cellular approach. New York, NY: Oxford University Press.
Paul, W. (2012). Fundamental immunology. Philadelphia, PA: Lippincott Williams & Wilkins.

