Introduction
Nosocomial infections, also known as health-care-associated infections (HAIs), are still a menace for many healthcare providers in the US. HAIs occur when patients under treatment catch dangerous infections that potentially lead to death or sepsis. The most vulnerable department of every health care setting is the Intensive Care Unit (ICU) since treatment here requires surgery or the use of medical devices in the body. According to Edwardson and Cairns (2019), 1 in 10 individuals admitted to healthcare settings contract hospital-acquired infections. CDC (2019) reveals that 20 000 out of 119 000 patients infected with bloodstream staph had died in 2017. The list of typical HAIs includes urinary catheter-related infection, surgical site infection, central-line associated bloodstream infection (CLABSI), and ventilator-associated pneumonia. The improper use of invasive devices often causes such kinds of infections. The longer the ICU stays, the greater risk for patients. Thus, proper interventions driven by leadership and evidence-based practices (EBP) are needed to improve health care delivery.
The gap analysis revealed that the increase in hospital-acquired infection in the organization was mainly caused by a lack of staff education and motivation to follow all protective guidelines. A lot of medical mistakes were made by nurses who were tired and stressed due to the increased workload. For instance, some of them had often forgotten to change gloves between patients or to sanitize equipment. Similar mistakes and lack of infection control lead to the inferior quality of rendered healthcare services and low patient safety. Executive leaders and management should put all their efforts into providing staff with the needed equipment, current guidelines, and training.
High-Performing Health Organizations
High-performing health organizations are concentrated on practice improvement to provide better services to their patients. The Baldridge Criteria for Performance Excellence, which has a systems perspective, may help the hospital to evaluate improvement according to a set of core values and concepts (Huffstutler & Thomsen, 2015). The truth is that individuals should not be blamed for mistakes and HAI occurrences because any failure primarily comes from the system.
For that reason, visionary leadership is expected to be aware of current challenges and focus on the future. Excellence can be achieved only by fostering a value-driven culture based on ongoing personal and organizational learning. Members of ICU and other departments should have their values and objectives aligned with the organization’s ones. Health care leaders should encourage staff’s professional development to improve interpersonal and group communication, transparency, and engagement. To manage alignment, effective hospitals conduct the value screens before hiring a potential team member or physician. Comprehensive action plans are used to realize the organization’s strategic objectives. Competent and disciplined leaders provide needed tools to teams to fulfill daily tasks (Huffstutler & Thomsen, 2015). Benchmarking performance against successful competitors is also essential as it shows current accomplishments against desired outcomes.
Moreover, high-performing health institutions are patient-focused since their main customers are patients and their families. They create value and focus on results to improve patient outcomes, patient engagement, and satisfaction. It requires workforce capability development and high leadership results. The hospital should adopt the Baldridge Framework to improve organizational systems and pursue excellence in patient safety. What is more, Goll and Cahill (2014) state that the key to improved performance is front-line staff engagement? Professionals who believe in the hospital’s vision and stick to strategic plans demonstrate behaviors according to leadership expectations. Nursing managers play an important role at the unit level, creating structures and relationships that help staff focus on improvement rather than simple compliance.
The hospital’s main problem lies in the fact that local management/leadership failed to empower front-line staff to design and test interventions based on recent evidence. The Transforming Care at the Bedside program is an excellent solution to current problems (Goll & Cahill, 2014). It provides a methodology and structure that involves staff meetings and identifying current gaps in knowledge and quality. Following the identification of barriers, the team devises the hypothesis about which measures will improve performance and ultimately tests it. As a result, when the tested intervention is successful, its implementation is continued for sustainability. This approach has great potential to address HAI issues in both the ICU and the entire healthcare organization.
Methods to Improve Safety Outcomes
A study conducted in the ICU of Evangelismos hospital (Greece) revealed that even simple multifaceted infection control interventions are able to prevent CLABSI. Mitsogiani et al. (2016) reported that CVC insertion bundled with full barrier precautions significantly decreased the BSI rate indicating its preventability. The hospital must undergo similar infection prevention and control intervention consisting of proper catheter insertion/removal, environmental and personal hygiene, and ongoing staff training. Education and measures will ensure nurses and physicians regularly apply and change such precautions as sterile caps, masks, gloves, gowns, and draping when using various invasive devices. It is also better to avoid the femoral line if possible and use skin antisepsis preparation (Mitsogiani et al., 2016). In order to improve control and enhance compliance, a special checklist should be introduced that will see practitioners filling it at every new insertion.
Other necessary measures are hand hygiene promotion, regular inspection of the insertion site, and environmental infection control. Advanced EBPs regarding urinary catheter use should be introduced as well to reduce CAUTI. What is more, education should be provided to nurses and physicians to encourage proper catheter care, improve insertion techniques, early indwelling urinary catheter removal, and the use of non-invasive alternatives.
Outcome Measures
Typical quality and safety outcomes include shorter hospital stays, lower treatment costs, and decreased cases of drug-resistant infections. It improves the health care service quality and ultimately leads to higher patient satisfaction. Interviews with care providers and patients are needed to monitor the effectiveness of measures and reserve a room for timely procedure adjustments. Outcome measures are designed to identify the impact of the presented intervention and strategy on patients’ safety and health. Since its primary goal is the reduction of nosocomial infections in ICU, the related rates should be monitored and compared to the pre-intervention results. The interest field comprises the MRSA rate, incidence of HAI-VRE, CAUTI, and HAI-CDAD per 1000 patient days. The intervention will prove to be effective if its methods result in decreased HAI rates.
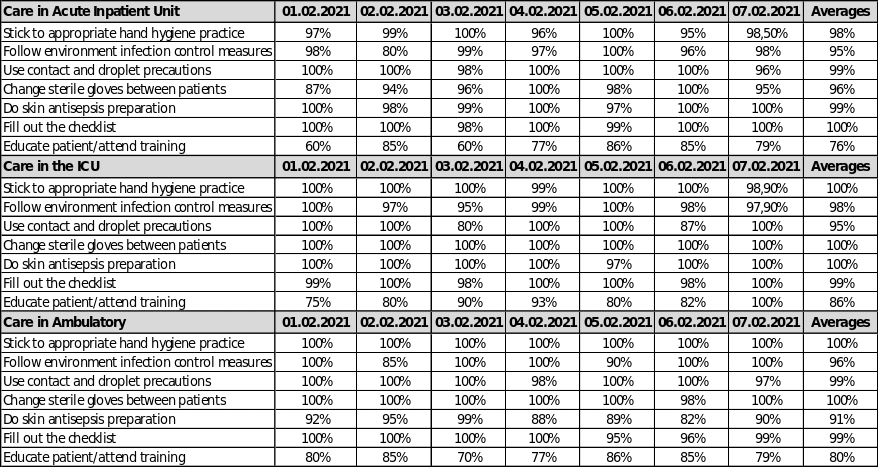
These outcome measures will monitor staff/team compliance in different hospital wards: appropriate hand hygiene, percentage of practitioners who follow environment infection control measures, and use of contact and droplet precautions. What is more, the spreadsheet takes into account regular changes of sterile gloves, antisepsis skin preparation, checks how nurses fill out checklists, and how often they educate patients. Table 1 in the Appendix shows how to measure compliance in Acute Inpatient Unit, ICU, and Ambulatory. It is essential to determine if practice change really occurs and if staff supports the new evidence-based practices to reduce HAI rates.
Performance Issues
Healthcare-associated infections are costly for care providers, especially under pay-for-performance systems. Vokes et al. (2018) reveal that the approximate annual incidence of nosocomial infections in inpatient hospital settings is 440 000 cases. Each year an estimated $9.8 billion is spent due to medical errors that lead to HAIs. Moreover, cases of nosocomial infections often have legal consequences and may decrease the perceived quality of service. The health care environment is always complex; thus, administrators are expected to coordinate the staff efforts in the fight with HAIs by allocating needed resources. The absence of cooperation between epidemiologists and clinicians also hinders the implementation of infection control programs and evidence-based guidelines.
Many similar studies addressed burnout as another performance issue. According to Cimiotti et al. (2012), there is a strong association between nurse staffing (patient-to-nurse ratio) and the occurrence of the surgical site and urinary tract infections. It is important to have enough nurses to provide needed services to patients avoiding staff burnout. The latter occurs when the practitioner works for excessive hours due to the lack of available staff and faces external mental demands (interruptions, feeling rushed, and divided attention).
Burnout in hospital settings usually stems from emotional exhaustion that makes nurses cognitively and emotionally detached from dealing with work demands. It was found that hospitals and units where every nurse cares for fewer patients are doing better in infection prevention (Cimiotti et al., 2012). On the contrary, the same study indicated that high nurse burnout caused by a more significant patient caseload increases the incidence of mistakes that cause HAIs. Cognitive detachment impedes adequate infection control practices such as hand hygiene. What is more, job-related burnout is negatively associated with job satisfaction. In its turn, the latter adversely affects employee turnover. Health care administrators and managers should reduce burnout through proper scheduling, staffing, and training to increase staff retention rate and job satisfaction. For instance, coping skills training can teach, develop, and improve resilience in nurses and physicians.
Outlined Strategy
Every change requires a well-designed leadership strategy to be implemented. The quality initiatives are deemed to fail in case of weak leadership since there are many barriers that should be circumvented. Nurses themselves, other practitioners, administration, and management can become a source of main barriers. Change theory suggests that successful change initiatives must have a structured approach. Kurt Lewin’s theory may be applied by management to foster the change process. It consists of three consequential stages: Unfreezing, Moving, and Refreezing (Mitchell, 2013). The first stage is about problem identification, assessment of resources, and motivation of change agents. The second stage requires actual actions and involvement of the staff. Refreezing is needed to sustain the change and reward desired outcomes. This simple theory can be helpful; however, it is better to use Lippitt’s or mixed theory for quality improvement interventions. The latter has 7 phases and is more detailed, making it more convenient for nursing managers to generate change (Mitchell, 2013). In terms of leadership styles, the implementation of change aimed at decreasing the HAI rate requires a democratic leadership style since it supports cooperation and coordination between groups.
Summary
To conclude, every healthcare provider should be patient-oriented and focused on the improvement of the services provided. HAI and related medical mistakes are current health care challenges that the hospital leadership should adequately address. Quality improvement and other interventions to implement evidence-based practices regarding catheter insertion, hand hygiene, and infection control measures are essential to foster patient safety. It is not easy to implement a change in large organizations without strong leadership. Lippitt’s and Lewin’s theories of change and the Baldridge Framework would help to cope with structural barriers.
References
CDC. (2019). Deadly staph infections still threaten the U.S. Web.
Cimiotti, J. P., Aiken, L. H., Sloane, D. M., & Wu, E. S. (2012). Nurse staffing, burnout, and healthcare-associated infection. American journal of infection control, 40(6), 486-490. Web.
Edwardson, S., & Cairns, C. (2019). Nosocomial infections in the ICU. Anaesthesia & Intensive Care Medicine, 20(1), 14-18. Web.
Goll, C., & Cahill, S. (2014). Enculturating the value of process improvement. American Nurse Today. Web.
Huffstutler, D. C., & Thomsen, D. (2015). A framework for performance excellence and success. Frontiers of Health Services Management, 32(1), 45-50.
Mitchell, G. (2013). Selecting the best theory to implement planned change. Nursing Management, 20(1), 32-37. Web.
Mitsogianni, M., Vasileiadis, I., Parisi, M., Tzanis, G., Kampisiouli, E., Psaroudaki, Z.,… & Tsiodras, S. (2016). A multifaceted intervention program to prevent bloodstream infection in an intensive care unit: An intervention for the reduction of bacteremia in ICU. Health Science Journal, 10(2), 1-6.
Vokes, R. A., Bearman, G., & Bazolli G. J. (2018). Hospital-acquired infections under pay-for-performance systems: an administrative perspective on management and change. Current Infectious Disease Reports, 20(9), 1-7. Web.
Appendix