Introduction
It is imperative to mention that many scholars have focused on the research of pressure ulcers and possible preventive measures over the years and some of the techniques suggested are quite comprehensive. However, it is still an enormous problem that needs to be resolved because many individuals suffer from this condition every single year. Furthermore, it is necessary to analyze available data to identify particular trends and the ways in which they may affect the implementation of a new project.
Discussion
Prevalence
The most important trend that should not be overlooked is that the pressure ulcers are becoming less common every year because of increased attention to this problem, and preventive measures are viewed as much more efficient. Reported rates of prevalence in America should be analyzed because a particular trend can be identified. It is possible to see that the percentage of such incident is much lower in long-term care when compared to acute treatment. The fact that prevalence rates vary from zero to twenty-nine percents at homes also should not be overlooked (Aslan & Van Giersbergen, 2016). The finding is vital because it may be necessary to modify the approach for every method of treatment to minimize the possibility of the introduction of complications (see Figure 1).
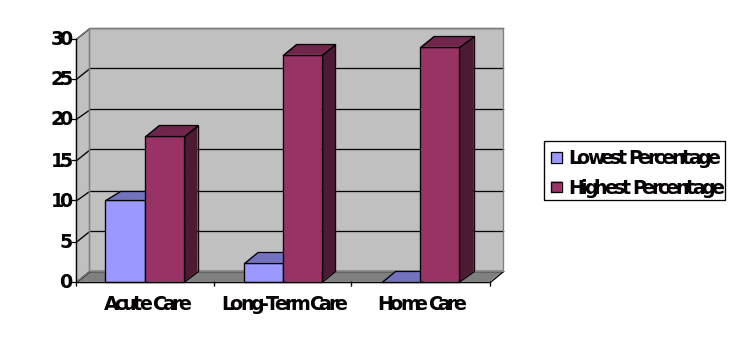
The data suggest that a pressure ulcer is less likely to occur when health care professional is focused on the patient and has enough time to take various aspects into consideration in some cases. However, numerous risks are also introduced, and it complicates the situation. Another trend that can be identified is that the number of risk assessment tools utilized in practice is steady reducing over the years. Moreover, such changes are crucial because the ones that are not efficient are eliminated, and only the ones that have proven to be effective are used. Kottner and Balzer (2010) have analyzed forty scales to determine their level of efficiency. Moreover, they suggest that they could be improved because accuracy and sensitivity scores are rather low. A more recent guideline supports this idea. The authors argue that only four scales are appropriate, but their accuracy is moderate at best (Qaseem, Mir, Starkey, & Denberg, 2015).
Such trend is quite worrying because the rate at which assessment tools are improved is rather small. However, it would be beneficial to focus on Braden, Cubbin and Jackson, Norton, and Waterlow scales because they provide best results. Another trend that is also highlighted in this case is the focus on evidence-based practice (De Chesnay, 2014). However, health care professionals at NYU Langone Medical Center have managed to reduce the prevalence of pressure ulcers by six percents over three years and achieved a 1,6% rate by using some approaches with different levels of evidence (Delmore, Lebovits, Baldock, Suggs, & Ayello, 2011). Such results are quite intriguing, but the article can be regarded outdated, and it will be reasonable to review some of the techniques and their cost.
Nurse Encounters
A study by Aslan and Van Giersbergen (2016) suggest that the biggest number of participants that worked in medical clinics had to deal with pressure ulcers rather rarely. However, the data also indicates that every health care professional had such encounter at least once. The research has been conducted in Turkey, but such trend is intriguing. The sample size was sufficient in this case to state that such findings are statistically significant (see Figure 2).
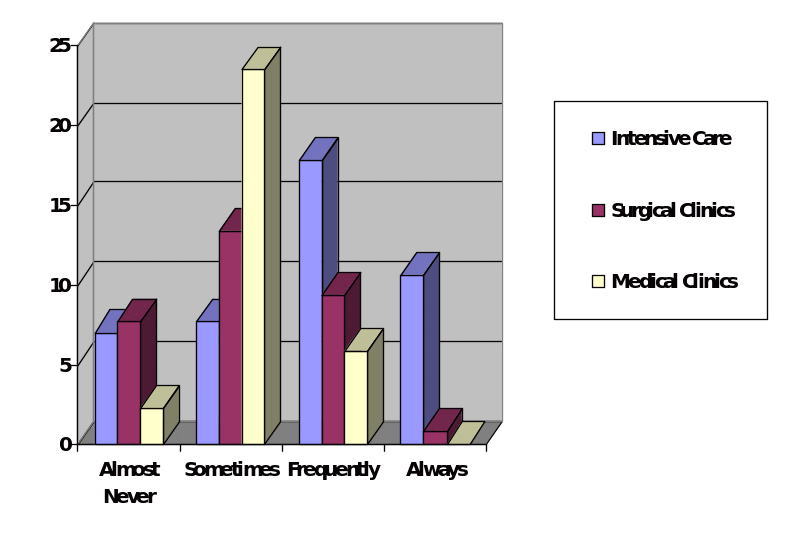
The complication that may occur is that it is not an easy task to justify the implementation of such approach when the number of such incidents is rather limited. Moreover, one may argue that nurses should be aware of only standard techniques. A particular gap is present in this case, and it would be reasonable to determine if the same situation is common in the United States. Almost all the articles suggest that the most significant problem is the lack of training and experience. It is paramount to assess the level of knowledge in the medical center, and the implementation strategy may have to be altered. Many scholars state that it is reasonable to question the words of a patient. It would be beneficial to conduct examinations and order tests when there is suspicion (Posthauer, 2014). Also, it is possible to state that scholars have recognized that it is a significant problem for all age groups, and they are aware of the fact that each one requires a unique approach. The issue is especially problematic when it comes to ill infants, and high percentages that vary from sixteen to twenty-seven are not acceptable (Scheans, 2015). This trend has an influence on the implementation of the project because several guidelines should be developed.
Approaches
Analysis of an article by Dealey et al. (2015) has shown that such terms as pressure and risk are mentioned most often. Therefore, it is possible to state that the authors are trying to identify all possible causes, and suggest measures that should be taken to reduce it. Skin is another term that can be seen throughout the paper. This finding suggests that it is reasonable to focus on such aspects as the level of dryness or moisture. Another fascinating aspect that should be highlighted is that researchers argue that all pressure ulcers may be prevented, and this idea does not change over the years. New techniques and approaches are being introduced over the years, and it is possible to get a better understanding of processes that lead to such issues. It is stated that most approaches do not help to address the pressure caused by devices (Dealey et al., 2015). Such risk is enormous because new technologies are used more commonly, and it may be hard to predict possible consequences. Another trend that needs to be discussed is that pressure ulcers remain a significant problem even when preventive measures are taken. Therefore, it is possible to state that the approaches suggested are not as efficient as they should be, or health care professionals do not devote enough attention to this problem. Furthermore, the impact of such findings is enormous because it is necessary to consider numerous internal and external factors.
Conclusion
In conclusion, it is possible to state that the trends identified have a tremendous influence on the project, and they should not be overlooked. It is necessary to take them into account because it may complicate the process of implementation of new approaches. The biggest risk that is present is the questionable effectiveness of assessment tools. The introduction of new technologies may also be quite problematic, and it is reasonable to keep track of the latest developments. It is not likely that they will be improved anytime soon because the ones that were developed long time ago are still viewed as the most useful. Overall, it is necessary to review and analyze all the available data and fill in current gaps to ensure that the process of implementation is successful.
References
Aslan, A., & Van Giersbergen, M. Y. (2016). Nurses’ attitudes towards pressure ulcer prevention in Turkey. Journal of Tissue Viability, 25(1), 66-73.
De Chesnay, M. (2014). Nursing research using data analysis: Qualitative designs and methods in nursing. New York, NY: Springer Publishing Company.
Dealey, C., Brindle, C., Black, J., Alves, P., Santamaria, N., Call, E., & Clark, M. (2015). Challenges in pressure ulcer prevention. International Wound Journal, 12(3), 309-312.
Delmore, B., Lebovits, S., Baldock, P., Suggs, B., & Ayello, E. A. (2011). Pressure ulcer prevention program: A journey. Journal of Wound, Ostomy and Continence Nursing, 38(5), 505-513.
Kottner, J., & Balzer, K. (2010). Do pressure ulcer risk assessment scales improve clinical practice? International Wound Journal, 3(1), 103-111.
Posthauer, M. E. (2014). Nutrition: Fuel for pressure ulcer prevention and healing. Nursing, 44(12), 67-69
Qaseem, A., Mir, T. P., Starkey, M., & Denberg, T. D. (2015). Risk assessment and prevention of pressure ulcers: A clinical practice guideline from the American College of Physicians. Annals of Internal Medicine, 162(5), 359-369.
Scheans, P. (2015). Neonatal pressure ulcer prevention. Neonatal Network, 34(2), 126-132.

