Nursing Project
Patient safety is a key element during transitions in care. Medication omissions and dosing errors during changes of care settings can be sources of avoidable patient harm. The occurrence of errors can be substantially reduced through medication reconciliation, which can be described as “the task of bridging discrepancies in a patient’s medical history after a care setting changes” (Ferdandes & Shojania, 2012, p. 43). This paper aims to outline a research project proposal on the improvement of medication reconciliation practices.
Problem
The quality of health care delivery during both within-hospital and external transfers hinges on the elimination of medication discrepancies that can lead to the occurrence of adverse drug events, discontinuity of treatment, and dosing errors. According to Mueller, Sponsler, Kripalani, and Schnipper (2012), the frequency of the occurrence of adverse drug events fall in the range from 5 percent to 40 percent for hospitalized patients and 12 percent to 17 percent for post-discharge patients. These are extremely high rates that indicate a serious underlying issue troubling national health care facilities—the inadequacy of medication reconciliation practices. At present, medication discrepancies affect almost 70 percent of patients at some point in transitional care (Mueller et al., 2012).
Furthermore, the significance of addressing the issues associated with facilitating medication safety during the transfer should be brought up as one of the reasons for concern. There is no secret that transitional care, as well as a patient handover, is fraught with numerous threats to the patient’s safety. Particularly, the lack of nurses’ understanding of the patient’s needs during the transfer needs to be recognized as a crucial problem that must be managed accordingly (Storm et al., 2014).
Given the scope of the problem, it is necessary to join the efforts of the Joint Commission, which has identified the enhancement of medication reconciliation quality as a national goal (Ferdandes & Shojania, 2012). The extant literature on the topic indicates that medication reconciliation the process that can be divided into three important steps (Hassali et al., 2012). The first step is the verification process that involves the collection of accurate medication history records.
The next step is the comparison of medication lists through the medication history. The final step is the reconciliation of records followed by documentation of all changes. This process helps to reassure that preventable errors associated with medications and doses are eliminated. Currently, not all health care organizations have effective procedures for medication reconciliation at each point of transitional care that involve the collaboration between such parties as physicians, nurses, patients and their families, and pharmacists among others (Hassali et al., 2012).
Significance of the Problem to Nursing
The significance of the nursing problem is evident in the fact that the Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey has been expanded by the addition of the Care Transition Measures (DelBoccio et al., 2015). Furthermore, the Joint Commission and other similar organizations have developed recommendations for safe transition practices that include medication reconciliation.
The heightened awareness of the problem of inadequate medication reconciliation procedures suggests that there is a pressing need for action. Given that the medication history is formed by contributions from multiple sources that include, but are not limited to, “the patient, primary care physician, medical specialists, outpatient medical records, hospital discharge summaries, and community pharmacies” (Hassali et al., 2012, p. 78), it is necessary to ensure that errors eliminated at all data nodes.
The significance of the issue for nursing is also underscored by the fact that medication errors occur not only during the transitions from emergency departments, which are characterized by substantial time-pressures but across all points of transitional care. A study on the perceptions among health care practitioners towards the implementation of a comprehensive medication reconciliation program shows the willingness of nurses to participate in the improvement of patient safety (Hassali et al., 2012).
Purpose of the Research
The research aims to determine the most effective practices that can be used for improving medication safety across all points of transitional care. The research will help to better understand the complexity of the current medication management process as well as typical organizational failures leading to the occurrence of errors. The research will be instrumental in the development of a program for the integration of proper medication reconciliation protocols into all pertinent clinical processes and addressing the major implementation challenges, thereby ensuring safety and positive patient outcomes.
Research Questions
The review of the extant literature on the topic has helped to formulate the following research questions:
- Q1: What are the most effective strategies for the reduction of medication errors during the medication reconciliation process?
- Q2: Which health care professionals contribute the most to the homogeneity of medication history records?
These questions will help to understand all critical elements in transitional care that might facilitate the occurrence of discrepancies between prescriptions and other medication errors.
Master’s Essentials
The following Essentials of Master Education in Nursing are aligned with the project: organizational and systems leadership, quality improvement and safety, translating and integrating scholarship into practice, interprofessional collaboration for improving patient and population health outcomes, and clinical prevention and population health for improving health (AACN, 2011). The research project will help to address the issue of the extremely high rates of medication error occurrence across all points of transitional care. The project is aligned with five out of nine Essentials of Master Education in Nursing that are extremely important in graduate education.
Design Phase 2
The avoidance of medication error is vital to the quality of care and safety of the patients (Storm et al., 2014). Medical error denotes an avoidable, undesirable result of healthcare, whether apparent, concealed, harmful, or harmless to the patient. A medical error may entail a wrong or imperfect diagnosis or prescription of illness, parturition, syndrome, contagion, or any other disorder (Nadin, 2017).
A medication error arises when a medical practitioner selects an unsuitable means of care or wrongly implements a suitable process of care; in healthcare, medical errors are usually expressed as human inaccuracies (Petronio, Helft, & Child, 2013).
Nevertheless, the definition of medical error has been under debate since numerous kinds of medication errors that range from insignificant to far-reaching exist, and causality is frequently poorly verified (Watson et al., 2013). This research project will discuss the improvement of medication reconciliation practices aimed at ensuring patient safety. All medical professionals and health institutions should strive to reduce the occurrence of medical errors and ensure that they effectively identify their causes, set up resolutions, and gauge the triumph of improvement.
Literature Review
Medication errors symbolize stern public health care concerns and create a threat to the wellbeing of patients (Petronio et al., 2013). Medical errors are the leading causes of death in the United States since between 45000 and 99000 patients are believed to die every year due to medication errors (Andel, Davidow, Hollander, & Moreno, 2012). Medication errors are accounted to cost the United States between $18 billion and $30 billion every year in lost revenue, disability, reduced productivity, and further medical costs (Andel et al., 2012). On this note, there is a need to support correct assessments of the occurrence of medical errors as a fundamental prerequisite for their avoidance.
As medical institutions ascertain “error” as a medical and study precedence, the resolution of possibly the vital inquiry remains elusive (Storm et al., 2014). When answering the question of what can be done to reduce medical errors and ensure the prevention of their occurrence, anchored in vivid and consistent definitions and crucial requirements for successful action, one should keep in mind that several opportunities are possible (Watson et al., 2013). Institutional and systems management, quality enhancement, patient safety, interpreting and incorporating research into practice, collaboration, and prevention of medication errors are crucial for boosting patient care (Ignjatović-Ristić, Vasiljević, Rančić, & Ristić, 2014).
According to the quantitative survey by Hripcsak, Sengupta, Wilcox, and Green (2007), health departments, especially the emergency unit, signify a considerable shift of care for patients and the comprehension of the longitudinal patient health situation (for instance, allergies, medicines, challenges, diagnoses, previous procedures, and pending tests) is vital to the formulation of a suitable strategy for care. Since most visits to the emergency departments are impromptu and urgent, the health conditions of the patients might not be issued beforehand to the caregivers. Even in cases that the information is availed to the caregiver, time constraints may limit their ability to pursue it (Hripcsak et al., 2007).
Such information gaps could result in not just poor quality of care, but also inefficiencies in care, like redundant tests, care impediments, medication errors, and less successful treatments stipulated instead of more modified interventions as a preventative measure when vital information is not accessible. Improvements in the healthcare sector could result in positive effects not only on the patients but also the health professionals in the respective organizations (Carayon et al., 2014).
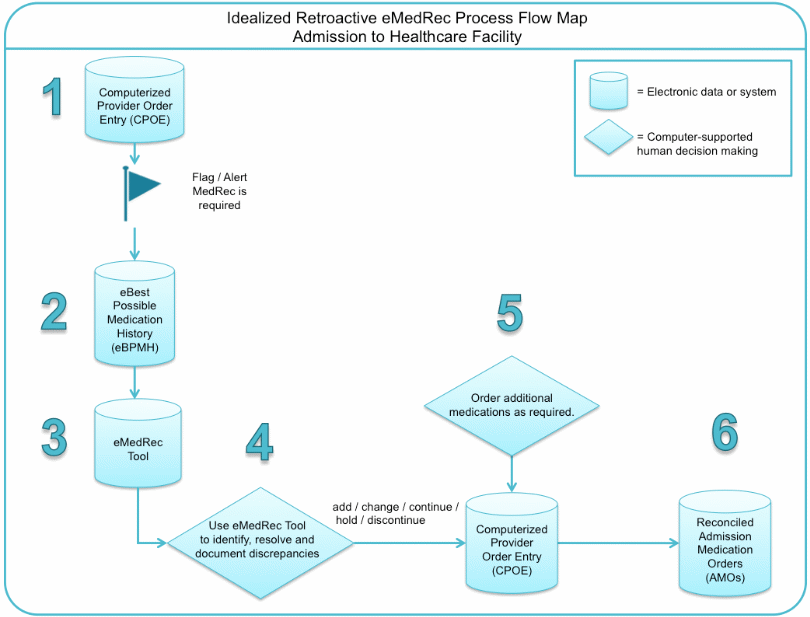
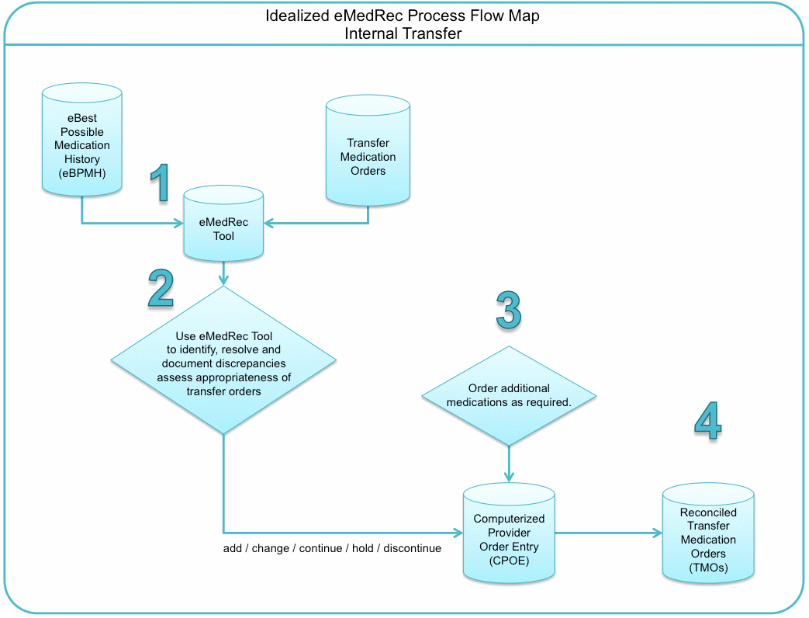
The objective of Hripcsak et al. (2007) was to examine how medical data from earlier visits is presented by the longitudinal electronic patient record and applied in the emergency department. The authors employed comprehensive user inspection logs to gauge access to dissimilar forms of data. A longitudinal electronic patient record was found mostly applicable in the diagnosis by the health professionals and provision of radiology and laboratory data, which proved valuable in most occurrences (common forms of details were utilized in 5 to 20 percent of the instances) (Hripcsak et al., 2007).
Information was accessed in less than half of the incidences (from 20 to 50 percent of the situations) even in occurrences that the user was informed of the existence of data (Hripcsak et al., 2007). The degree of access demonstrates that the medical information exchange programs ought to be conservative in approximating how regularly shared information will be employed. Moreover, the broad range of the accessed data signifies that though a medical summary has the potential of being valuable, a perfect solution will necessitate offering a wide scope of information and advocating for its use by health professionals in an effort of avoiding medication errors and ensuring quality care and patient safety (Raban & Westbrook, 2014).
Methodology
Research Design
This study will exploit the primary means of data collection where information will be acquired from Tisch Hospital, in New York City. The type of research design that will be employed in this project is a qualitative study. Qualitative analysis, mainly ethnographic research, will allow collecting and analyzing a large amount of narrative data that will be collected from the target population. Semi-structured interviews will be used as the main tool for collecting the relevant data for further analysis.
Population and Sample
The population for this study will be the health professionals and patients in Tisch Hospital. To recruit the participants for the study, one will have to consider submitting a written application for the selection of the study participants, as well as composing a letter of informed consent that will be distributed among the members of the target population. The Chief of Hospital Operations will receive the said documents for further acceptance. Before the research is launched, possible issues should be discussed with the members of the nursing staff; thus, conflicts and misconceptions, as well as possible threats to patients’ well-being, will be addressed.
Sampling Strategy
The non-random sampling strategy will be used as the primary design for data collection in the study. The accessibility to the information and the ease of use are the primary factors contributing to the choice of the sampling approach. The research participants will be contacted with the help of the Chief of Hospital Operations, who will send them letters suggesting that the target population should participate in the study. Twenty participants (5 healthcare experts, 8 male patients, and 7 female patients) will be selected for the study. It is expected that the identified approach will contribute to securing the patients’ private data and, therefore, promote confidentiality and non-disclosure.
Data Collection Plan
As soon as the participants are recruited for the study, they will take part in semi-structured interviews with open-ended questions. Thus, the premises for retrieving essential information that would not have been gathered otherwise will be built. Particularly, the intrinsic factors affecting the patients’ well-being will be discovered. The choice of the open-ended questions can also be explained by the fact that the identified approach supports the assay format that will allow the participants to provide the required number of details in their responses. The use of the survey framework, in turn, will become the foundation for the identification of the details that will, later on, be used as the foundational concepts for building a comprehensive practice framework (Goniewicz, Lingas, & Hajek, 2013).
Instrumentation
Before starting an interview, one should consider explaining every stage of the data collection and analysis process to the participants. Thus, the premises for efficient cooperation can be built. Particularly, the participants should be aware of the goals of the research, the number of questions (five), the type of questions that they will be asked, the areas that will be addressed in the course of the interview, and the time that they will have to answer these questions (30 minutes). Furthermore, the fact that a tape recorder will be used throughout the interview will have to be mentioned to the participants (the transcription of the participants’ answers will be used to carry out a detailed analysis). Thus, maximum cooperation will be achieved, and a range of misconceptions will be cleared.
Data Analysis
The data analysis approach for this research project will depend on the study technique and form of data collected. For this study, a qualitative means of data analysis will be employed. The assessment of the nominal facts for this study will be descriptive and will have a vital task in backing a better understanding of the intricacy of the present medication management practices in addition to characteristic organizational flaws resulting in the incidence of errors.
The rising insight of the incidence, causes, and effects of medical error strengthens the necessity to boost the comprehension of the problem and create practical resolutions and prevention policies. This research project will be influential in the creation of a program for the incorporation of appropriate medication reconciliation practices into all relevant medical processes, and handling execution challenges to ensure patient safety, quality care, and positive outcomes.
Nursing Project Phase 3: Implementation
The problems of medication error and issues about drug reconciliation play a highly adverse role in the contemporary medical care setting. It is stated that adverse drug events take place in the percentage of cases that fall within the range from 5% to 40% for hospitalized patients, and within the range from 12% to 17% for post-discharge patients (Mueller, Sponsler, Kripalani, & Schnipper, 2012). Medical errors are also very costly; it is estimated that in 2008, for example, they cost the U.S. nearly $19.5 billion (Andel, Davidow, Hollander, & Moreno, 2012).
Thus, it is paramount to find out what leads to medication errors to be able to take action to address these causes and decrease the frequency of medication error occurrence in the medical setting. Therefore, this paper details the implementation of a research project aimed at uncovering the reasons for drug errors and problems with medicine reconciliation in the hospital setting.
A Step by Step Instruction for Implementation
On the whole, it is possible to implement the medication error and medication reconciliation research project in five main steps. These steps will include the creation of questionnaires for the interviews; contacting the Chief of Hospital Operations of the target hospital; gathering the sample of participants who will be interviewed for the proposed project; conducting the interviews, and analyzing the data which will be gathered throughout the project. More details related to each phase of this procedure are provided below.
Phase 1
At this step, the researcher will have to create the questions for the interviews which will be conducted with the participants of the study. It is paramount to stress that, since the sample will include two main types of participants, that is, health professionals and patients, it will be required to create two different questionnaires – one for each type of the participants.
These questionnaires will be comprised of five open questions each, formulated in a manner that will prompt the respondents to reflect upon their experiences about the medication error and the problems which caused issues with medicine reconciliation, and give a textual answer to these questions (Denzin & Giardina, 2016). It should also be stressed that at the beginning of the questionnaires, a form will be included that will ask for the informed consent of the participants to take part in the study.
Phase 2
After the creation of the questionnaires, it will be needed for the researcher to contact the Chief of Hospital Operations of the target hospital (the Tisch Hospital, which is located in New York City, NY). The researcher will make a phone call to the Chief of Hospital Operations and will ask for a face-to-face meeting aimed at discussing the details of the research with the hospital’s official and gaining his or her permission to carry out the study.
On the agreed date and time, the researcher will go to the office of the Chief of Hospital Operations, explain to him or her the nuances of the study, its importance, and significance, and ask for permission to conduct the research. It is expected that the Chief of Hospital Operations will allow to carry out the study; in the (unlikely) case of failure to obtain the permission, the researcher will have to choose a different hospital for the study.
Phase 3
After the permission to conduct the study will be obtained, the researcher will contact the potential participants (nearly five doctors, eight male patients, and seven female patients) by giving them requests to take part in the study (via the Chief of Hospital Operations). The explanation of the crux of the problem and the research study will be provided to the potential participants, and they will be asked to help with unveiling the causes of the frequent medication errors in the health care system. Once enough individuals will agree to take part in the study, the recruiting process will be ceased.
It should also be noted that, once the first participants are recruited, it will be possible to start the interviewing process, for not all the respondents need to be interviewed simultaneously, and some of them might become unavailable at a later date.
Phase 4
Once at least some participants are recruited, they will be interviewed by the researcher using the previously created surveys. The interviewees will be asked to provide their answers to the questions in an essay format. In addition to that, the interviews will also be tape-recorded to permit gathering more precise information from them. It is expected that each interview will last for nearly 30 minutes, but the participants will be allowed to take their time answering the questions if they desire to, to ensure that they provide full answers which comprehensively describe their opinions about the issues in question.
Phase 5
Finally, after the interviews are conducted, the researcher will be able to analyze the data gathered throughout the study. It will be needed to employ the qualitative methods for data analysis (Denzin & Giardina, 2016). In particular, it might be decided that coding will be an appropriate technique for data analysis, in which case the texts gained during the interviews will be subjected to coding techniques to identify the main themes emerging in the responses of the participants (Saldaña, 2013), which may be employed to explain the potential causes of medication errors and the problems related to drug reconciliation in the given setting.
The timeframe of the Project
Table 1 below presents the detailed timeframe of the project, explaining how much time is expected to be required to carry out the steps outlined in the previous sections of this paper.
Table 1. A detailed timeframe of the project.
Required Budget
On the whole, it is possible to implement the proposed project without any substantial financial investment (which also means that it can be implemented by a student); the only necessary spending will be to cover the costs of printing questionnaires and forms. However, if the researcher decides to transcribe part of or all the audio recordings made during the interviews, this will require additional funding, depending on how much of the recording will need to be transcribed.
It is also possible to pay the participants some money for the interview, but giving them much money should probably be avoided to ensure that they participate because they have what to say, and not simply because they want to make some additional money.
Other Resources Needed
It is expected that apart from the time, the access to the phone, the computer, and the Internet, as well as some money to cover the stationery needs of the research, no other resources will be required for the implementation of the proposed project. On the whole, it should be stressed that medication errors and problems with drug reconciliation lead to highly adverse outcomes for the patients, and cost the U.S. considerable amounts of money. The proposed study might help uncover the reasons for these problems. To conduct the study, a five-step process will have to be implemented, which is expected to take several months to complete.
Nursing Project Phase 4: Results
The primary goal of the research was to answer two questions:
- What are the most effective strategies for the reduction of medication errors during the medication reconciliation process?
- Which health care professionals contribute the most to the homogeneity of medication history records?
Demographics of the Sample Population
The sample population studied in the course of the research includes patients and health professionals at Tisch Hospital, New York City. Since the study design is qualitative and the researcher used questionnaires and interviews as instruments for data collection, it is crucial first to mention the demographic characteristics of the sample population. By using non-random convenience sampling (since it was the most accessible), the researcher ended up with a sample of 20 individuals (five doctors, eight male patients, and seven female patients) to interview and survey during the study. Within the sample of five physicians, two of them were male, and three of them were female.
The cultural characteristics of the study are the following: seven White Americans (one doctor and six patients), five African Americans (two doctors and four patients), three Hispanic patients, and five patients of another ethnic background (Asian and Indian). As to the educational level of study participants, all five doctors reported holding a Medical Degree (two Doctors of Medicine, one Master of Medical Science, and two Masters of Clinical Medicine).
The educational background of the patients enrolled in the study was more diverse: one female patient held a Doctor of Philosophy Degree, three male and one female patient held a degree in Economics, two male patients reported holding a degree in engineering, two female patients were studying at college at the time of the research, three female and three male patients only graduated high school and did not have a professional degree. Among the patients that did not have a degree and only graduated high school, African American and Hispanic ethnicities were the most prevalent, which points to the unequal distribution of educational resources within the community.
The income level of the study participants is divided into three distinct categories differentiated by annual earnings. Within the sample population, two patients and five doctors reported a salary between $60,000 and $150,000 per year, which placed them in the upper-middle-class category, five patients reported an annual salary between $32,500 and $60,000 and were placed in the middle-class category, eight patients reported their annual salary below $32,500, which puts them in the lower-middle-class category.
As to the occupational characteristics of the study participants, six participants (including five doctors) worked in the medical profession, three participants reported working in marketing and sales, two members were involved in the sphere of education, three participants worked in the service industry, two participants reported to have their own business, and four participants reported being unemployed at the time of the research.
The marital status of the sample population was divided equally: ten participants reported to be married or engaged while ten participants were single. Lastly, when asked about their religious identity, fourteen participants identified as Christian, two participants identified as Buddhist, two identified as Muslim, and two identified as atheists.
Descriptive Data Points Interpretation
Questionnaires
In surveys, study participants were asked to give honest answers to questions about the occurrence of medication errors during the process of medication reconciliation as well as the role of healthcare professionals in contributing to the homogeneity of medication history records. The questionnaires focused on two distinct themes that directly referred to the initial research questions. Therefore, to provide respondents with options to answer the posed questions, the Likert-type scale was used.
This means that respondents had to answer the questions by choosing one option from the scale (Strongly Disagree, Disagree, Neutral, Agree, Strongly Agree). Each question in the survey contained a statement regarding medication errors and medication history records, with which the respondents had to either agree or disagree.
To report the results of the questionnaires more clearly, the table below shows exact answers respondents gave to the posed questions:
Overall, it can be concluded that the research participants emphasized the role of the health care providers as the ones that should be responsible for the management and completion of documentation reconciliation for avoiding errors in medication prescription. However, previous findings show that patients can also play an important role in preventing errors in medication through being educated about what they are prescribed (Barnsteiner, 2008).
The questionnaire showed that the participants saw potential in the clear identification of responsibilities and standardization when it comes to effective documentation reconciliation. Moreover, respondents met the idea of collaboration between patients and health care providers with mixed opinions; however, the majority (11 respondents) agreed that such cooperation was needed for avoiding medication errors.
Interviews
During the interviews, study participants were not confined to strictly answering the questions they were asked. On the contrary, they had more freedom to give their opinions in an essay format and thus provided answers with sufficient details without any constraints. The results of the interviews with both healthcare providers and patients can be divided into three themes, such as the impact of medication errors, responsibilities of the healthcare provider, and the role of patients.
If to present the findings of the interviews with doctors, it is crucial to mention that all five participants indicated that the increased workload limits professional’s effectiveness in documentation management, as evidenced by previous research (Child Welfare Information Gateway, 2016). Moreover, doctors pointed out that a high percentage of patients lack knowledge about the medication that they are prescribed, which subsequently leads to errors in medication. Health care providers agreed that medication errors and improper documentation reconciliation presented a threat to the well-being of patients (Petronio, Helft, & Child, 2013), so there was a high need for the standardization and clear identification of responsibilities, as well as the active participation and contribution of patients.
Patients, on the other hand, referred to the process of documentation reconciliation as the responsibility of doctors and were hesitant regarding their role. A prevailing theme of the interviews was patients admitting to having insufficient knowledge about the prescribed medication (Grossmann, Goolsby, Olsen, & McGinnis, 2012); however, they felt that it was the responsibility of their health care providers to provide education on medication they prescribe to patients. Similar to doctors, patients agreed that medication errors and improper documentation reconciliation were threatening to their well-being, although they did not know how the errors could be eliminated effectively.
Research Limitations
The research was limited in two areas: the choice of the sampling technique and the final size of the sample. While non-probability convenience sampling is the most accessible since the researcher could select the most convenient units, results derived from this sampling technique have known generalizability only to the studied sample (Bornstein, Jager, & Putnick, 2013). This means that the initial research questions that were addressed with the help of convenience sampling are limited to the sample itself, which was relatively small. Another disadvantage associated with the choice of convenience sampling is linked to the small percentage of underrepresented sociodemographic subgroups, which results in the lack of sufficient power to determine differences in sociodemographic factors (Mosadeghrad, 2014).
Conclusion
The research provided an extensive learning experience. The study indicates that patients lack education concerning the needs that they may have in the process of the medication reconciliation process. Furthermore, the lack of initiative on the patients’ side can be viewed as a legitimate problem since the identified phenomenon impedes the process of providing adequate services. Thus, based on the Essentials of Master’s Education in Nursing, the strategies for improving the communication process during the administration of the required medications and the processes associated with handling the patients should be introduced along with the tools for increasing the leevsl of patients’ awareness.
Implications for Future Research
The results of the research showed that there are differences in the way patients and health care providers perceived medication errors and documentation reconciliation. Therefore, future research may focus on the development of an action plan to combine the efforts of health care providers and their patients for eliminating medication errors and reducing the limitations associated with the reconciliation of documentation. For example, an intervention where one group of patients will have to collaborate with their healthcare providers can be designed. Then, the patient outcomes regarding medication prescription can be compared with the outcomes of the second group that did not collaborate with their doctors.
References
AACN. (2011). The essentials of Master’ Education in Nursing. Web.
Andel, C., Davidow, S. L., Hollander, M., & Moreno, D. A. (2012). The economics of health care quality and medical errors. Journal of Health Care Finance, 39(1), 39-50.
Andel, C., Davidow, S. L., Hollander, M., & Moreno, D. A. (2012). The economics of health care quality and medical errors. Journal of Health Care Finance, 39(1), 39-50.
Barnsteiner, J. (2008). Medication reconciliation. In R. Hughes (Ed.), Patient safety and quality: An evidence-based handbook for nurses (pp. 386-401). Rockville, MD: Agency for Healthcare Research and Quality.
Bornstein, M., Jager, J., & Putnick, D. (2013). Sampling in developmental science: Situations, shortcomings, solutions, and standards. Developmental Review, 33(4), 357-370.
Carayon, P., Wetterneck, T. B., Rivera-Rodriguez, A. J., Hundt, A. S., Hoonakker, P., Holden, R., & Gurses, A. P. (2014). Human factors systems approach to healthcare quality and patient safety. Applied Ergonomics, 45(1), 14-25.
Child Welfare Information Gateway. (2016). Caseload and workload management. Web.
DelBoccio, S., Smith, D., Hicks, M., Lowe, P., Graves-Rust, J., Volland, J.,…Fryda, S. (2015). Successes and challenges in patient care transition programming: One hospital’s journey. OJIN, 20(1), 19-34.
Denzin, N. & Giardina, M. (Eds.). (2016). Qualitative inquiry: Past, present, and future: A critical reader. New York, NY: Routledge.
Ferdandes, O., & Shojania, K. (2012). Medication reconciliation in the hospital: what, why, where, when, who, and how? Healthcare Quarterly, 15(1), 42-49.
Goniewicz, M. L., Lingas, E. O., & Hajek, P. (2013). Patterns of electronic cigarette use and user beliefs about their safety and benefits: An Internet survey. Drug and Alcohol Review, 32(2), 133-140. Web.
Grossmann, C., Goolsby, A., Olsen, L., & McGinnis, M. (2012). Engineering a learning healthcare system. Washington, DC: The National Academies Press.
Hassali, M., Al-Hadda, M., Shafie, A., Tangiissuran, B., Saleem, F., Atif, A.,…Al-Qazaz, H. (2012). Perceptions among general medical practitioners toward implementation of medication reconciliation program for patients discharged from hospitals in Penang, Malaysia. Journal of Patient Safety, 8(1), 76-80.
Hripcsak, G., Sengupta, S., Wilcox, A., & Green, R. A. (2007). Emergency department access to a longitudinal medical record. Journal of the American Medical Informatics Association, 14(2), 235-238.
Ignjatović-Ristić, D., Vasiljević, S., Rančić, N., & Ristić, B. (2014). Difficulties in proving medical errors: Where do we stand? Vojnosanitetski Pregled, 71(4), 390-394.
Mosadeghrad, A. (2014). Factors influencing healthcare service quality. International Journal of Health Policy and Management, 3(2), 77-89.
Mueller, S., Sponsler, K., Kripalani, S., & Schnipper, J. (2012). Hospital-based medication reconciliation practices. Archives of Internal Medicine, 172(14), 1057-1069.
Mueller, S., Sponsler, K., Kripalani, S., & Schnipper, J. (2012). Hospital-based medication reconciliation practices. Archives of Internal Medicine, 172(14), 1057-1069.
Nadin, M. (2017). Medicine: The decisive test of anticipation. Anticipation and Medicine, 1(1), 1-27. Web.
Petronio, S., Helft, P. R., & Child, J. T. (2013). A case of error disclosure: A communication privacy management analysis. Journal of Public Health Research, 2(3), 175-181.
Petronio, S., Helft, P. R., & Child, J. T. (2013). A case of error disclosure: A communication privacy management analysis. Journal of Public Health Research, 2(3), 175-181.
Raban, M. Z., & Westbrook, J. I. (2014). Are interventions to reduce interruptions and errors during medication administration effective? A systematic review. BMJ Quality & Safety, 23(5), 414-421.
Saldaña, J. (2013). The coding manual for qualitative researchers (2nd ed.). Los Angeles, CA: Sage.
Storm, M., Groene, O., Testad, I., Dyrstad, D. N., Heskestad, R. N., & Aase, K. (2014). Quality and safety in the transitional care of the elderly (phase 2): The study protocol of a quasi-experimental intervention study for a cross-level educational programme. BMJ Open, 4(7), e005962. Web.
The Electronic Medication Reconciliation Group. (2017). Paper to electronic MedRec implementation toolkit (2nd ed.). Web.
Watson, A. J., Redbord, K., Taylor, J. S., Shippy, A., Kostecki, J., & Swerlick, J. (2013). Medical error in dermatology practice: Development of a classification system to drive priority setting in patient safety efforts. Journal of the American Academy of Dermatology, 68(5), 729-737. Web.

