Introduction
According to Burns and Grove (2010), various methods have been proposed to use to expand the use of evidence based practices in healthcare care delivery. Some of the proposed methods include integrating patient values and preferences with clinical experience based on the best scientific evidence, preparing and sustaining staff knowledge about EBP, enabling interdisciplinary teamwork, Leadership support, and establishing EBP expansion objectives.
Patient values and preferences
Integrating patient values and preferences enables the nurses and other professionals to consider the benefits of practising clinical service delivery on evidence, making it an exception rather than a rule (Burns & Grove, 2010). That is in addition to assessing the limitations that occur in the provision of healthcare services, barriers and the human factors that cause them, organizational factors that limit expansion of EBP, determining their causes, and eliminate them.
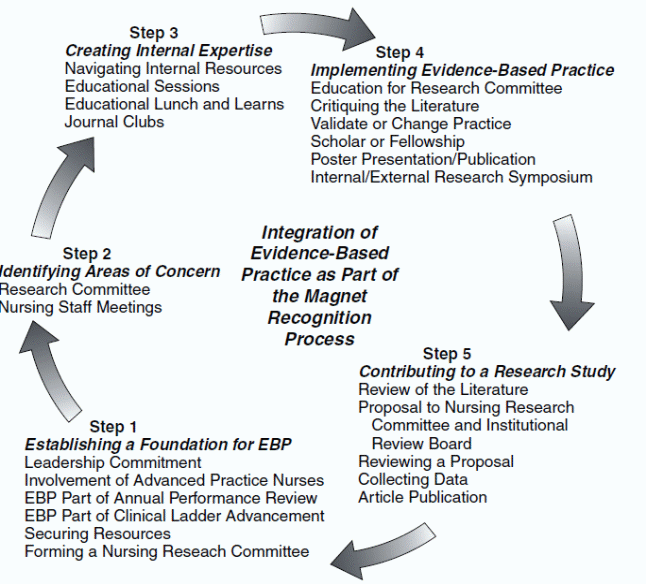
To address the barriers that negatively affect the expansion, the nurses should implement a program to provide training and professional support to the nurses to enhance their knowledge and skills in EBP. In addition, the process is used to facilitate leadership and institutional support for the EBP, and develop policies and procedures based on structured charts that show how to implement EBP and clinical practices (Burns & Grove, 2010). There should not lack leadership commitment based on an established EBP foundation. The use of EBP contributes to research studies and the creation of internal expertise on the effective and efficient use of resources.
Use of scientific evidence
The next approach that has widely been recommended is the use of scientific evidence based practice. This is where a professional nurse provides high quality services to the patient using decisions that are based on scientific evidence (Burns & Grove, 2010). Expansion of the EBP can only be effective if the services are of high quality. Clinical services should incorporate scientific evidence when making various treatment and therapeutic decisions. Robust scientific evidence is consistent with professional consensus in addressing patient needs.
Preparing and sustaining staff knowledge about EBP
Staff needs to be prepared not only on how to administer services, but also on how to use technology such as how to interact with information systems to conduct research on the internet for new information on the services being offered (Grol & Grimshaw, 2003). Regular tests need to be conducted on educational interventions to ensure accountability. That is besides encouraging nurses and other professional support staff to complete an annual research competency that underpins the hospital’s strong commitment to advancement in knowledge and evidence-based practice.
Enabling interdisciplinary teamwork
The contribution of multiple disciplines and trans-disciplinary teams provide the foundation to expand without the need to challenge disciplinary boundaries. Nurses need to be prepared to work in teams that are stymied to provide high quality services (Grol & Grimshaw, 2003). That is in addition to working to improve patient care outcomes and healthcare delivery services. Besides, multiple disciplines enable complex solutions to problems, narrowing of knowledge gap between knowledge transaction and translation, and effective collaboration.
Leadership support
Leadership is one of indispensable instruments that facilitates culture shift that is necessary for implementing the expansion of evidence-based practice. Here, system change and expansion can be implemented by offering symbolic and concrete support through the operations, management, human resource, and staff development support (Grol & Grimshaw, 2003). The core leadership competencies include understanding the practice, enthusiasm for search, ability to communicate future vision and mission statements, and capacity to communicate positive outcomes. That is besides establishing staff development resources in the expansion of the EBP. Educational resources needed for the expansion of the EBP include journal clubs, evaluation tools, research mentors, workshops, and fellowships (Grol & Grimshaw, 2003). That is besides the use of information systems (IS) consisting of reference databases, clinical data repositories, and decision support software.
Developing EBP expansion Objectives
Sometimes written statements provide a description of the strategies for acquiring skills that are indispensable for expanding evidence based practice. The rationale for the objectives is on how to change the attitude of nurses, enhance psychomotor objectives, and improve cognitive objectives to achieve higher thinking skills (Houser & Oman, 2011). Besides, there is need to conduct a needs assessment to determine the gap between current and future need of the proposed EBP system. Once the objectives have been established, it is important to nominate an appropriate expansion model to use. Despite the models having common elements such as practice questions, current research practices, national standards, guidelines and existing clinical research, and data quality outcome data, there is need to determine the best model to integrate into EBP model.
Example is the Colorado Patient-Cantered Inter-professional Evidence Based Practice Model. In this model, leadership, facilitation, organizational support, and mentorship form the core components of the system (Houser & Oman, 2011).
Conclusion
To expand the use of evidence based practices in healthcare, various methods and models have been suggested for nurses to nominate to expand the EBP. Besides, the use of technology has been with special emphasis on information systems has been proposed to store data that is later accessed and used to professionally implement the EBP.
References
Burns, N., & Grove, S. K. (2010). Understanding nursing research: Building an evidence-based practice. New York: Elsevier Health Sciences.
Grol, R., & Grimshaw, J. (2003). From best evidence to best practice: effective implementation of change in patients’ care. The Lancet, 362(9391), 1225- 1230.
Houser, A., & Oman, K. S (2011). Evidence-Based Practice: An Implementation Guide for Healthcare Organizations. Sadbury: Kevin Sullivan

