Introduction
Falls are a leading cause of injury, reduced disability-adjusted life years (DALYs), and increased dependence among the elderly. With the rapidly aging population, a growing number of older adults are at risk of falling. Elderly falls have multiple intrinsic or extrinsic causes and key influences. The main risk factors are environmental hazards, poor footwear, and loss of balance due to chronic illness (dementia), medication effects (psychotropic drugs), alcohol use, and muscle weakness due to reduced physical activity (McMahon et al., 2019). However, it is not clear if these causes vary by gender, age, or between community-dwelling versus hospitalized patients.
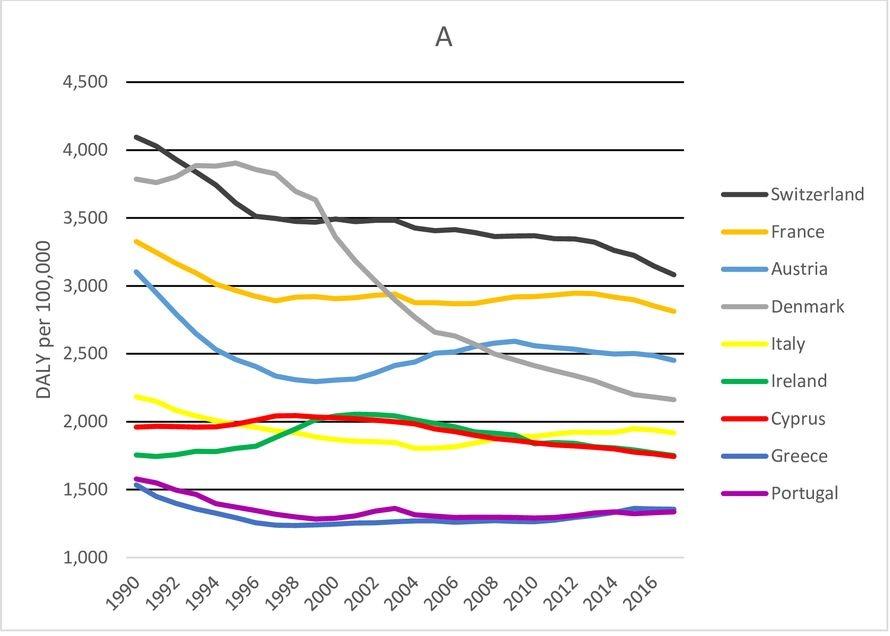
The prevalence of falls varies between countries, as the at-risk population is different. In the United States, an estimated 28.7% of the elderly aged ≥65 years suffer a fall in their homes annually, accounting for 27,000 fatalities and 7 million injuries that need medical attention (Centers for Disease Control and Prevention [CDC], 2020). In Europe, the burden of fall-related injuries (DALYs) is disproportionately high in low- and middle-income nations (Figure 1). The lowest prevalence has been reported in Greece (7.6%) and Portugal (8.1%), while the rate is highest in Norway (19.8%) (Haagsma et al., 2020). The case fatality rate across Europe also follows the same patterns.
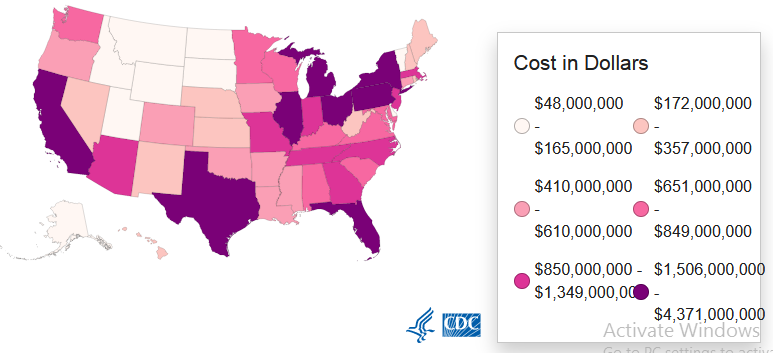
The monetary costs associated with falls in the US are significant. The CDC (2020) estimates that the economic burden of non-fatal fall-related injuries is $50 billion annually in medical expenditure mainly incurred by Medicare and private payers. It excludes indirect costs related to the long-term impact of sustained injuries. States with the highest cost burden (≥$4 billion) include California, Texas, and Florida, while North Dakota and Wyoming spend the least in fall-related medical care (≤$91 million) annually, as shown in Figure 2 (CDC, 2020). Thus, effective community-based interventions are needed to address the consequences of falls, including the high costs.
Advanced Practice Roles and Management Strategies
Advanced Practice Nurses (APNs) are ideally positioned to address modifiable risk factors linked to falls among the elderly in the community. In particular, nurse practitioners practicing in primary care settings: can do screening for fall risk and routine follow-up of high-risk older adults, especially those with comorbidities or under psychotropic medication. A key factor contributing to a high fall incidence in this population is limited family support or living alone (Dellinger, 2017). APNs can meet the geriatric care demands of individuals, including living arrangements and medical treatments. Consistent with their training, APNs can also deliver case management, provide transitional care after discharge, and conduct health promotion (exercise and nutrition) to reduce frailty and delay cognitive impairment. These strategies decrease hospitalizations and falls among high-risk older adults.
Key Community and Social Resources
Multifactorial interventions to reduce falls target risk factors specific to a community. The success of these programs depends on the community and social capital resources. In the US, appropriate 8-12 week exercises delivered in primary care settings, such as the Otago exercise program, can help improve psychomotor performance to reduce injurious falls (Dellinger, 2017). They aim to build leg strength and reverse physical frailty among community-dwelling older adults. Another community resource includes positive media images, campaigns, and outreach programs that enhance the acceptability of group activities and the use of assistive devices. Social support systems, including family, can help older adults achieve health-related goals to reduce the fall risk. Conversely, negative stereotyping, the perceived inevitability of falls in the elderly population, and programs that impact self-image increase this problem.
Changes or Enhancements
Community-related services are crucial for fall prevention practices targeting older persons. A key change to enhance physical activity is education for high-risk elderly individuals and those designing houses and public facilities. Risk-factor assessment by APNs is also critical to inform multifactorial interventions for individuals identified as having a high fall risk profile. Besides environmental risk assessment, addressing footwear and visual problems through assistive devices and reducing medication effects can help lower falls among community-dwelling older persons.
Strategic Plan
Goals
- By June 2022, train 40% of the current community health practitioners on fall risk identification and screening.
- By August 2022, link three community coalitions to trained APNs delivering the Otago exercise program to prevent falls where the elderly live.
Actions
Health literacy
- Nursing staff education on fall risk assessment, intervention, and follow-up.
- Health literacy for high-risk older adults on the correct use of assistive devices after discharge.
- Gait training and exercise programs based on the Otago model.
Socioeconomic factors
- Create informal social and referral networks involving faith-based community members.
- Safety net and better housing for older adults – grab bars, better lighting, and stair railings.
- A review of alcohol use policies and psychotropic medications that increase the fall risk.
Cultural differences
- Informal group educational sessions that involve sharing individual experiences in the older adults’ language.
- Visual aids (leaflets) aligned to the target audience’s cognitive level and culture.
Conclusion
The plan’s goals are to enhance nurses’ capacity to identify and screen for predictors of falling among older adults based on environmental and behavioral risk factors. Further, a collaboration with community coalitions to improve physical activity is considered in this plan. Potential challenges include limited long-term adherence to the program and comorbidities that reduce participation. Progress in reducing fall incidence is likely to be made since the interventions adopted are specific and multifactorial.
References
Centers for Disease Control and Prevention. (2020). Old adults fall data. Web.
Dellinger, A. (2017). Older adults fall Effective approaches to prevention. Current Trauma Reports, 3(2), 118-123. Web.
Haagsma, J. A., Olij, B. F., Majdan, M., van Beeck, E. F., Vos, T., Castle, C. D., Dingels, Z.
V., Fox, J. T., Hamilton, E. B., Liu, Z., Roberts, N. L., Sylte, D. O., Aremu, O., Bärnighausen, T. W., Borzi, A. M., Briggs, A. M., Carrero, J. J., Cooper, C., El-Khatib, Z., … Polinder, Z. (2020). Falls in older-aged adults in 22 European countries: Incidence, mortality and burden of disease from 1990 to 2017. Injury Prevention, 6, i67–i74. Web.
McMahon, S. K., Park, Y. S., Lewis, B., Guan, W., Oakes, J. M., Wyman, J. F., & Rothman, A. J. (2019). Older adults’ utilization of community resources targeting fall prevention and physical activity. Gerontologist, 59(3), 436-446. Web.

