Background and explanation
Oregon Community Health Information Network (OCHIN)
A healthcare IT NGO headquartered in Portland, Oregon United States. It is managed by a board of directors (majorly volunteers from member clinics). A membership of approximately 70 providers (with more than 300 clinics). Initiated in 2001 to facilitate integration of IT and communal HER. EHR centrally located and connected to member clinics.
Community health center (CHC) and community advocates in Oregon initiated OCHIN to enable the incorporation of IT in health care provision. Most importantly, CHCs were seeking for a common electronic health record (EHR) to augment safety and reduce the cost of health care. OCHIN, therefore, is a milestone in care delivery, and it received preliminary funds from the U.S. Department of Health and Human Services’ Health Resources and Services Administration (HRSA).
OCHIN has realized growth over time, transforming into a health care information technology hub. The success is attributed to aspects such as good governance (board of directors), economies of scale, and commitment to mission and goals (DeVoe & Sears, 2013). Thus, OCHIN has approximately 70 members serving more than 900,000 patients in more than ten states in the US (Arkind, et al., 2015).
The Healthcare Delivery Model
Availability of data and informatics expertise is vital for inclusive care provisions. However, getting IT resources is challenging, especially to individual small-scale clinics (Bazemore, et al., 2015). As such, OCHIN adopts a “patient-centered medical village” model to harness resources to improve IT in health care in member clinics.
The OCHIN model of health care delivery is one of the shared IT resources and learning models (DeVoe & Sears, 2013). The model gives the member clinics an opportunity to share IT expertise, information resources, and data. Consequently, member clinics can make use of advanced and innovative technologies to augment health care (DeVoe & Sears, 2013).
Additionally, the model reduces the cost incurred on research and increase the validity and reliability of research. Specifically, the OCHIN model facilitates research over wide data and practiced based research. For instance, OCHIN enhances community-based partnership and consequently uses health IT to come up with community-tailored IT solutions (DeVoe & Sears, 2013).
The Structure of the Organization
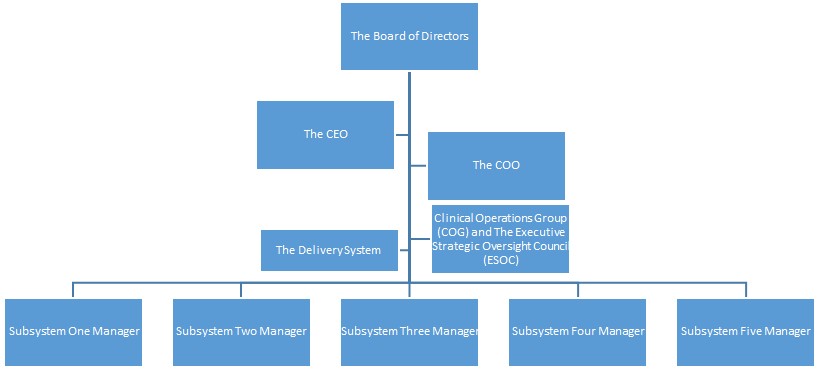
The Oregon Community Health Information Network (OCHIN as other states joined) structure consists of the Board of Directors, the CEO, the COO and Clinical Operations Group (COG) and the Executive Strategic Oversight Council (ESOC) (DeVoe & Sears, 2013).
The Board is made up of communities that emanate across the country, and it is responsible for making strategic business decisions. All members uniquely collaborate to ensure shared decisions of EHR, further improvements on clinical decision support tools, and the ways data collected are utilized.
The COG consists of clinical leaders drawn from all community member organizations. COG is responsible for reviewing suggested changes to the shared EHR and guiding quality improvement processes and public health initiatives across the country.
The ESOC is responsible for providing strategic direction on critical factors that influence clinical activities. Collaborative processes guide decision-making often made through consensus. The COO runs the delivery system alongside several managers responsible for subsystems.
The Communication Patterns Identified Throughout the Process
OCHIN established a collaborative communication system to achieve its purpose of ‘providing technology information and solutions to the medically underserved’. Consequently, it was able to create a community of solutions for its target partners.
Internally, the leadership team initially delegated communication to the COO to facilitate communications with associates that had worked with OCHIN from the start. The executive leadership team later took ownership of communication. It is widely acknowledged that the success of any institution largely relies on the effectiveness of communication that emanates from senior executives, as well as interaction among all stakeholders (Wagner, Bezuidenhout, & Roos, 2015).
The weekly schedules are meant to facility consultation and collaboration. It is also imperative to recognize that all communications remained transparent to develop trust among stakeholders.
The IT communication platforms were designed to promote easy, safe, and secure communication between stakeholders. As such, electronic healthcare records were secure while physicians leveraged fast processes to improve out comes.
Further, OCHIN promoted flexible adaptive communication while striving to identify organizational needs and learning more about personality intelligence to promote change and limit resistance.
The Negotiation Strategies Applied & Opportunities for Relationship Building Across Departments
OCHIN engaged in strategic collaborative processes to ensure that all decisions made supported stakeholders’ interests so that all could benefit. In fact, all strategic decisions on data usage, system improvement and external relations were based on collaborative, consultative processes.
The organization relied on a give and take approach to facilitate a learning organization while stressing the importance of individual roles to integrate people into the new system. Further, it demonstrated that all stakeholders were responsible for the success of the organization.
Several opportunities were available for OCHIN to build relationships across its department. For instance, sustained learning had ensured that employees could identify strengths in other to build productive partnership.
Employees were encouraged to know how to find solutions and ask for help when necessary as they shared information to enhance learning. In addition, OCHIN encouraged team, inclusivity and urged employees to embrace diversity and learning while making favorable decisions for all stakeholders.
How the Organization’s Performance Changed as a result of the Initiative
It is imperative to recognize the OCHIN performance improved after its transformation from primarily an electronic health record installation company to a health information and technology provider. As such, several improved processes and collaboration were noted on shared learning, clinical readiness, a change in workflow, improved provider and staff training, system hosting, implementation, optimization, reporting, billing, and efficient use of EHR systems for strategic clinical operational and financial objectives. The decision-making processes became more data-driven.
Changes in performances have also been noted in diabetic patient care, clinical readiness, workflow changes, provider and staffing training, quality improvement processes, interpersonal development, and data-driven decisions on patient management (DeVoe, et al., 2011). These are new metrics, which define performances at OCHIN.
Laws, Regulations, Accrediting Bodies, and Practice Standards for Consideration as Part of the Initiative
OCHIN is recognized under the not-for-profit provision 501(c)(3) with its board of directors. It must conform to the Health Insurance Portability and Accountability Act (HIPPA) privacy rules and ensure that it allows sharing patient data between covered bodies. OCHIN also conforms to the Organized Health Care Arrangement that is generally recognized under HIPPA to ensure effective management and benefits of all stakeholders.
OCHIN received Connect Accreditation from Epic, which is the US top organization recognized for EHR software.
The Connect Accreditation ensures that OCHIN adopts the best practices and quality standards as it shares common health information with other bodies while creating synergy between EHR and information sharing (Gold, et al., 2015). In addition, the Agency for Healthcare Research and Quality (AHRQ) ensures that OCHIN is independent and is focused on community research.
References
Arkind, J., Likumahuwa-Ackman, S., Warren, N., Dickerson, K., Robbins, L., Norman, K., & DeVoe, J. E. (2015). Lessons Learned from Developing a Patient Engagement Panel: An OCHIN Report. Journal of the America Board of Family Medicine, 28(5), 632-638.
DeVoe, J. E., & Sears, A. (2013). The OCHIN Community Information Network: Bringing Together Community Health Centers, Information Technology, and Data to Support a Patient-Centered Medical Village. The Journal of the American Board of Family Medicine, 26(3), 271-278.
DeVoe, J. E., Gold, R., Spofford, M., Chauvie, S., Muench, J., Turner, A.,… Nelson, C. (2011). Developing a Network of Community Health Centers with a Common Electronic Health Record: Description of the Safety Net West Practice-based Research Network (SNW-PBRN). The Journal of the American Board of Family Medicine, 24(5), 597–604.
Gold, R., Burdick, T., Angier, H., Wallace, L., Nelson, C., Likumahuwa-Ackman, S.,… DeVoe, J. E. (2015). Improve Synergy Between Health Information Exchange and Electronic Health Records to Increase Rates of Continuously Insured Patients. eGEMs (Generating Evidence & Methods to improve patient outcomes), 3(1), 1-7.
Otte-Trojel, T., de Bont, A., van de Klundert, J., & Rundall, T. G. (2014). Characteristics of patient portals developed in the context of health information exchanges: early policy effects of incentives in the meaningful use program in the United States. Journal of Medical Internet Research, 16(11), e258.
Wagner, J.-D., Bezuidenhout, M., & Roos, J. (2015). Communication satisfaction of professional nurses working in public hospitals. Journal of Nursing Management, 23(8), 974–982.

