A diagram of fishbone
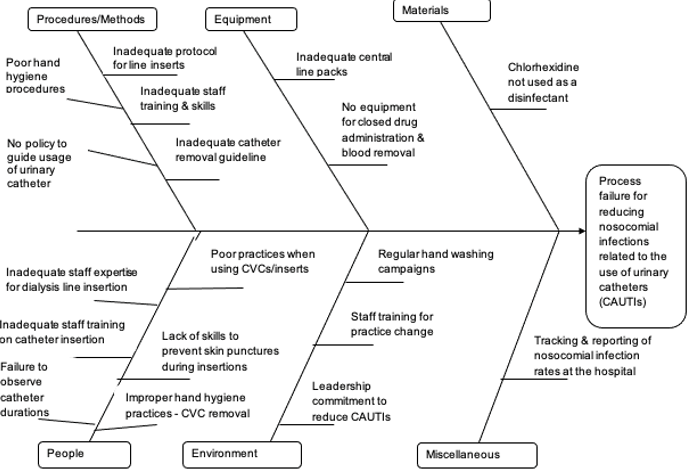
The high rate of nosocomial infections, e.g., catheter-associated UTIs (CAUTIs), indicates a process failure at the Kendall Regional Medical Center. The possible root causes of hospital-acquired infections in the facility are illustrated in the Fishbone diagram below.
Summary
A rise in hospital-acquired infections, including CAUTIs, is a basis for Medicare non-payments; hence, it is a significant performance/quality improvement issue. According to Halpin, Milstein, Shortell, Vanneman, and Rosenberg (2011), the Medicare non-payment policy affects hospitals reporting a quarterly rise in the rate of hospital-acquired infections such as pneumonia and UTIs. Thus, CAUTIs is an issue of quality/performance improvement.
The host of steps/root causes contributed to the high rate of CAUTIs at Kendall. Inadequate protocols and procedures for hand hygiene practices and urinary catheter insertion and removal increase the risk of CAUTIs. Additional root causes include the lack of specialized equipment for closed IVs and blood removal, non-utilization of chlorhexidine antiseptic solution, and inadequate staff skills and best practices (McHugh, Martin, Orwat, & Van Dyke, 2011).
Possible recovery steps at Kendall included surgical safety checklists to minimize errors during urinary catheter insertion and removal. Another recovery step may have involved an antibiotic administration protocol in the surgical unit. Kendall might also have implemented hand-washing procedures for indwelling catheters.
I would use systematic root-cause analysis (RCA) to identify quality problems and undesired events related to CAUTIs at the facility. These problems may occur in areas related to equipment/software, personnel, method/practice, or measurement. I would perform a SWOT analysis to identify process/practice hurdles and improvement opportunities to prevent CAUTIs. I would use FMEA principles to formulate a list of hazards that increase the rate of CAUTIs (failure mode causes) and identify preventive actions.
One of the barriers to using a Fishbone diagram relates to the difficulty of representing interrelationships between the root causes of a healthcare performance issue. Also, a large space is required to draw a detailed diagram to indicate relationships between process variables.
Hospital-acquired infections constitute an area of focus of quality improvement efforts of most healthcare organizations. Hospital strategies to reduce nosocomial infections include collaboration to develop “best practices and peer learning” and support unit-level safety initiatives (Reese, Gilmartin, Rich, & Price, 2014, p. 599). Further, rural hospitals use hand hygiene protocols and surveillance cultures to prevent nosocomial infections (Stevenson et al., 2014).
Other strategies for reducing catheter-associated infections include removing unessential catheters and the use of chlorhexidine solution (Haun et al., 2014). The similarities between these strategies and my approach include continuous monitoring of CAUTIs at the hospital and best practices in hand hygiene and catheter insertion and removal. They differ with respect to collaborative partnerships in safety programs.

