Abstract
The focus of this paper is on one of the mortal diseases which recently demonstrated an increased incidence. It is liver cancer which has high mortality rates and different causes of its development. The paper studies the pathophysiology of liver cancer and outlines the leading causes of the disease. Major clinical manifestations and assessments are described and analyzed. It also presents the diagnostic studies which help to diagnose the disease. Moreover, the strategies of clinical management and treatment for liver cancer are provided. The paper also gives some attention to liver cancer modalities. Finally, the possible treatments are assessed and the possible interventions aimed at patient education and safety are suggested.
Introduction
Cancer is among the leading causes of death worldwide. It is considered that the risk of developing cancer increases with age. Moreover, the incidence of cancer depends on gender, lifestyles, ethnicity, infection, and genetics (McCance & Huether, 2014). At present, there exist over one hundred cancer diseases. The risk of developing cancer and the reaction to treatment interventions is affected by the interaction of the environment, heredity, and behavior. Cancer is “a well-organized tissue from a defined organ or tissue” (Gu, 2012, p. 1). It can include cancer cells, fibroblasts, vasculature cells, immune cells, and stroma. The mentioned constituents in the cancer tissue form a specified milieu which is defined as a “cancer microenvironment” (Gu, 2012, p. 1).
The term cancer is commonly used to refer to a malignant tumor (McCance & Huether, 2014). Malignant tumors are characterized by rapid growth, no encapsulation, invasion of local structures and tissues, high mitotic index, and the ability to spread distantly. However, the development of cancer is specific for every patient and depends on the cell or tissue of origin. In 2016, there were 1,685,210 new cases of cancer and 595,690 cancer deaths registered in the United States (Siegel, Miller, Jemal, 2016, p. 7). Although the cancer death rates have decreased, some cancers develop more often than in the previous decades. For example, the incidence of liver cancer has increased. In 2016, 39,230 new cases of liver cancer were detected in the United States, and 27,170 people died because of this disease (Siegel, Miller, Jemal, 2016, p. 9). Thus, this paper studies pathophysiology of liver cancer, peculiarities of its diagnosing and treatment, evaluates their efficiency and provides implications for patent education and safety.
Pathophysiology of Liver Cancer
There are two major dangerous conditions connected with the liver. They are cirrhosis and liver cancer. These hepatic pathologies are the primary causes of death because of liver diseases worldwide and the prognoses are not optimistic (Muriel, 2017). Figure 1 depicts statistical data on global mortality because of viral hepatitis, liver cancer, and cirrhosis.
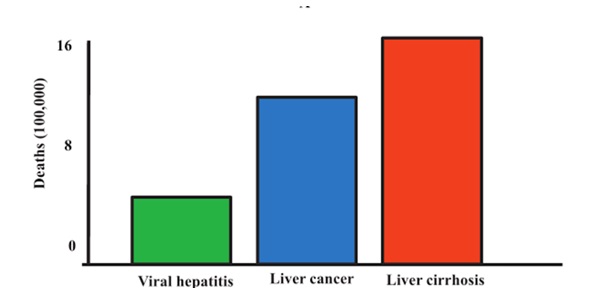
The most frequent type of liver cancer is hepatocellular carcinoma. It is also known as primary liver cancer and is “the fifth common liver cancer worldwide and the second leading cause of cancer mortality” (Muriel, 2017, p. 10). It is crucial to understand the pathophysiology of hepatocellular carcinoma (HCC) to provide timely diagnosing and treatment because HCC patients usually have a poor prognosis and the ratio of mortality is 0.95.
There is no clear picture of HCC pathophysiology. Nevertheless, it is influenced by many factors (Cicalese, 2017). After linking the hepatitis B virus (HBV) infection and HCC development in 1981, it was considered a primary cause. Still, further investigations did not prove that HBV infection was a dominant independent risk factor for HCC. Moreover, the studies revealed the fact that the majority of HCC cases were recorded among patients with cirrhotic liver disease of diverse etiologies. Also, some of those patients had negative markers for HBV infection (Cicalese, 2017). Thus, HBV is only one of the possible causes for HCC together with cirrhosis and some other health issues.
A cirrhotic liver is characterized by “inflammation, necrosis, fibrosis, and ongoing regeneration” which have an impact on the development of HCC (Cicalese, 2017, papa. 17). In their turn, patients with HBV can develop HCC in “livers that are not frankly cirrhotic, underlying fibrosis is usually present, with the suggestion of regeneration” (Cicalese, 2017, papa. 17). The process of disease development can follow different schemes, but all of them lead to malignant transformation. This process is exposed to the influence of many external and environmental factors and can cause genetic changes that “delay apoptosis and increase cellular proliferation” (Cicalese, 2017, papa. 18). Although different nodules are often found in cirrhotic livers, they do not always progress into HCC. The researches prove that the appearance of small-cell dysplastic nodules is a sign of a higher HCC risk. At the same time, large-cell dysplastic nodules are not related to the higher HCC risk.
Description of the Clinical Manifestations and Assessments
The incidence and prevalence of liver cancer in general and HCC as its major type have increased recently. That is why it is crucial to notice the first symptoms and diagnose the disease for timely and suitable treatment. Similar to other kinds of cancer, liver cancer clinical manifestations differ from patient to patient and thus make diagnosing more complicated. People with cancer or cirrhosis in family history should be more attentive to the possible cancer symptoms.
Cancer Treatment Centers of America (n.d.) singles out the following clinical manifestations that can be evidence of liver cancer development. Their assessment can be a reason to recommend blood tests or radiology investigations to check the patient’s condition. Thus, one of the possible symptoms of liver cancer is the loss of weight not preceded with alterations in lifestyles or diet. It can also be characterized by the loss of appetite. The first signs of liver problems can be nausea and vomiting of unidentified etiology. Continuous general weakness and fatigue should also be disturbing factors. One more sign which is a reason to consult the doctor is the fever that is not related to any known health conditions. Location of pain on the right side of the upper abdomen or close to the right shoulder blade can also be a symptom of liver cancer development. Other reasons to have a consultation with a specialist are the enlarged liver, enlarged spleen, and abdominal swelling or bloating in the abdomen (Cancer Treatment Centers of America, n.d.). An evident manifestation of the problems in liver functioning is the yellowing of the eyes and skin that are known as jaundice.
Many of the possible liver cancer symptoms coincide with the manifestations of other liver problems. A typical sign of cancer is the further development of these symptoms and the worsening of the patient’s condition. It is necessary to visit a specialist to consult on the disturbing symptoms which can be the signs of cancer or other liver diseases. Rarely, some other dangerous conditions can be caused by the development of liver cancer. The awareness of the possible relation of these syndromes to liver cancer can help diagnose the disease. Thus, the syndromes include hypercalcemia (characterized with high levels of blood calcium); hypoglycemia (low blood sugar levels); erythrocytosis (increased red blood cell count), and hypercholesterolemia (high cholesterol levels) (Cancer Treatment Centers of America, n.d.). The proper assessment of these clinical manifestations is key to timely diagnosing and, as a result, better patient outcomes.
Diagnostic Studies
The success of treatment and patient outcomes greatly depends on the early detection of liver cancer and proper interventions. Consequently, the choice of diagnostic studies and tests is crucial for the patient’s well-being and clinical outcomes. There are some major approaches to diagnosing liver or other cancers. They include radiology, blood tests and tumor markers, and biopsy (Carr, 2014). Radiologic screening for HCC is noninvasive. It uses ultrasound, computed tomography, and magnetic resonance imaging (Reau & Poordad, 2012).
Ultrasound abdominal scanning is extensively applied for screening due to its comparatively low costs, lack of ionizing radiation, and availability in most of the countries. Ultrasound is a useful tool in assessing the condition of patients with hepatic cirrhosis. Contrast-enhanced ultrasound (CEUS) with microbubble ultrasound contrast agents (UCAs) “offers ultrasound the ability to characterize focal liver lesions based on vascularity” (Reau & Poordad, 2012, p. 48).
However, ultrasound cannot be precise enough if a suspicious liver nodule is found on screening. In this case, a more definitive evaluation is needed. It can be provided with the use of computed tomography (CT) or magnetic resonance imaging (MRI) scan (Carr, 2014). The choice of method usually depends on the availability of the institution with suitable equipment and the presence of experts able to interpret the results of a scan.
Multidetector CT (MDCT) crucial for the imaging of cirrhosis and the detection and description of focal hepatic lesions. Multidetector row CT scanners appeared in the 1990s which empowered the reduction of imaging times (Reau & Poordad, 2012). Moreover, the increased sensitivity of new tools improves the detection of HCC. Thus, the ability of CT scanners to provide smaller slice thickness results in a sensitivity of 76% on 2.5-mm images, 73% on 5-mm images, and 67% on 7.5-mm images (Reau & Poordad, 2012, p. 49). CT is also helpful in detecting macronodular changes because they distort the hepatic surface contour.
Magnetic resonance imaging is a perfect tool for the identification and specification of focal hepatic lesions. Reau and Poordad (2012) state that “The development of fast gradients, parallel imaging, and employment of higher field strengths allow for breath-hold imaging and dynamic contrast exams (50). The recently introduced imaging techniques such as diffusion-weighted imaging (DWI) proved to be suitable in imaging HCC. What is more important, MRI, in contrast to CT, does not expose the patients to ionizing radiation. Consequently, it is more suitable for the screening of high-risk patients who cannot be regularly examined using CT.
Blood tests that define tumor markers are also applied in diagnosing cancer. A widely used alpha-fetoprotein (AFP) test is simple and cheap, but its effectiveness in HCC patients if only 50% (Carr, 2014). It is nor sensitive enough to detect small new HCC while is efficient in assessing individual patient’s reactions to therapy. There were developed some more HCC-specific tests which are applied in the general clinical practice. They are a glycosylated form of AFP (which is a fetal form of albumin) known as AFP-L3, and des-gamma carboxy prothrombin (DCP) (Carr, 2014). They both are approved by the US Food and Drug Administration and are available in many healthcare facilities. As for the tumor markers, they are not common in detecting liver cancer. Some new hepatocellular carcinoma tumor markers are the subjects of the current investigations and evaluation, but they are not yet introduced into wide clinical practice.
Finally, biopsy as a way to detect cancer is a matter of debate. Its contradictors focus on the invasive character of the method and suggest the application of non-invasive procedures such as ultrasound or CT. Nevertheless, in the common oncology practice, a biopsy is the only tool that can provide a certain diagnosis. A biopsy is a safe procedure that is executed by a professional. Its evident advantage is a certain diagnosis, especially when the radiological characteristics are not typical for HCC or the AFP levels are low” (Carr, 2014, p. 19). The avoidance of biopsy can result in the wrong diagnosis and the following potentially toxic or invasive therapy which is unnecessary.
Clinical Management and Treatment
At present, there are diverse opportunities for cancer treatment. In the case of liver cancer and HCC in particular, the possible treatments include “surgical resection, radiofrequency ablation, percutaneous ethanol ablation, transcatheter chemoembolization, Yttrium-90 radioembolization, and liver transplantation (Reau & Poordad, 2012, 45). The selection of the treatment strategy depends on the stage of the disease, the patient’s condition, and the possibilities of a healthcare facility. Some of them are characterized by minimal invasion and others are more invasive while all therapies can be efficient. Their curative effect often depends on the peculiarities of the patient’s organism and its response to the selected strategy. Nevertheless, the major factor influencing the positive lasting outcomes and successful HCC surveillance is the early detection of the disease and timely intervention (Reau & Poordad, 2012).
Liver Cancer Modalities
Liver cancer modalities include diverse types of screening such as ultrasound, magnetic resonance imaging, or computed tomography. Each of these diagnostic modalities uses “a different technique to examine the hepatic parenchyma with differing levels of accuracy for lesion detection” (Reau & Poordad, 2012, p. 45). Frequently, one modality does not provide a reliable result. Then, some modalities can be necessary to reveal and describe focal hepatic lesions to provide an appropriate diagnosis. It is important to introduce a working knowledge concerning the possible types of lesions that cab develops in hepatic cirrhosis because for some lesions there is a possibility of images overlapping.
Evaluation of Treatments
Current evaluation of treatment strategies is provided on the example of hepatocellular carcinoma which is the most frequent liver cancer. Thus, the choice of therapy is conditioned by some factors which include the extent of the tumor, its aggressiveness (biology), and the degree of liver dysfunction (hepatitis or cirrhosis or both) (Carr, 2014). Thus, HCC can be treated through surgery intervention applying resection of liver transplantation. Also, local ablative therapies can be used such as cryosurgery, radiofrequency ablation, microwave ablation, or percutaneous ethanol injection. There are also regional therapies which include transarterial chemotherapy, embolization, chemoembolization, and radiotherapies (internal liver radiation), conformal external beam radiation, and some others. Finally, there exist systemic therapies, such as molecularly targeted therapies, immunotherapy, chemotherapy, and hormonal therapy (Carr, 2014). Any of these interventions also demands a supportive therapy.
The choice of intervention depends on the treatment perspective. Thus, there are potentially curable cases, those that are treatable with intent to prolong survival, and palliation (Carr, 2014). For potentially curable cases, ablation or resection makes the first possible choice in case the tumor is small and the liver is functioning well. This intervention provides the expected survival of 40–70% at 5 years (Carr, 2014). Another way-out for potentially curable HHC is liver transplantation that is suitable for a small number of tumors or a single tumor not bigger than 6.5 cm in diameter. The condition of the liver is not significant for this approach.
The expected survival rate is 70–80% at 5 years (Carr, 2014). Strategies aimed at survival prolongation include hepatic arterial therapies (such as TACE, chemoembolization, and radioembolization), and systemic therapy, predominantly sorafenib. Hepatic arterial therapies are used for “large, widespread, or multiple tumors without metastases or PVT (but patients with PVT can receive radioembolization)” (Carr, 2014, p. 29). The expected survival is estimated at 5–30% at 2 years. Systematic therapy is more suitable for managing metastases or in case of PVT presence and failure of TACE/chemoembolization or radioembolization. Its safety is proved for patients with CP cirrhosis. The average survival is about eleven months. Finally, palliative, symptomatic care can be used in case none of the above-mentioned strategies can be used or appeared to be not successful.
Patient Education and Safety
Apart from the development and implementation of cancer treatment strategies, attention should be given to the enhancement of patient education and the promotion of safety. Patient education should be aimed at informing the population about the risk factors for liver cancer, its clinical manifestations, the necessary tests to take if any disturbing symptoms are revealed, etc. Another intervention that can be useful in the prevention of liver cancer, is hepatitis therapy. Since hepatitis is one of the causes of liver cancer, its timely and proper treatment can help to reduce the risk of cancer development. Similar intervention can address popularizing healthy lifestyles to avoid cirrhosis that also is one of the determinants of liver cancer. Patient education should also comprise work with family members of people diagnosed with cancer. Their task is to provide support and stimulate treatment compliance. The psychological aspect and a person’s intentions are often decisive in the process of treatment.
Conclusions
On the whole, the issue of cancer has been a subject for many investigations. The development of successful treatment strategies is more complicated due to the diversity of cancer types and the ambiguity of their etiology. Although the major reasons such as heredity, lifestyles, and the environment are generally accepted to be decisive, cancer is one of the diseases that cannot be confidently predicted or prevented. Consequently, the best way to successful treatment is early detection of the disease. In the case of liver cancer, diagnosing can be complicated because of the similarity between cancer and other liver diseases. Thus, it is important to be aware of then specific pathophysiology of liver cancer and timely assess the present clinical manifestations. After that, the choice of the diagnostic studies and tests will help to prove the diagnosis and apply the suitable treatment. It is important to evaluate the benefits and dangers of the selected interventions considering the condition of every patient.
References
Cancer Treatment Centers of America. (n.d.). Liver cancer symptoms. Web.
Carr, B.I. (2014). Understanding liver cancer: A tale of two diseases. London, UK: Springer.
Cicalese, L. (2017). Hepatocellular carcinoma. Web.
Gu, J. (2012). Primary liver cancer. Challenges and perspectives. Hangzhou, China: Zheijang University Press.
McCance, K.L., & Hueter, S.E. (2014). Pathophysiology: The biologic basis for disease in adults and children (7th ed.). St. Louis, MO: Elsevier.
Muriel, P. (2017). Liver pathophysiology: Therapies and antioxidants. London, UK: Academic Press.
Reau, N., & Poordad, F.F. (Eds.). (2012). Primary liver cancer: Surveillance, diagnosis and treatment. New York, NY: Springer.
Siegel, R.L., Miller, K.D., Jemal, A. (2016). Cancer statistics, 2016. Cancer Journal for clinicians, 66(1), 7-30. Web.

