Introduction
According to Carrieri and Bilger (2013), “cervical cancer, or cancer of the cervix, is cancer of the entrance to the uterus (womb). The cervix is the narrow part of the lower uterus, often referred to as the neck of the womb” (p. 243). This condition is predominant in the old women above the age of 30 years. In the UK, the government and other agencies have been proactive in developing policies to aid in the detection, diagnosis, treatment, and prevention mechanisms. These policies are design to aid in primary and secondary intervention at the national, local, and personal levels (Wu 2008).
There is need for extensive research to establish the specific policies have been developed in the UK to prevent cervical cancer among adult women besides measures that are taken to improve the health and well-being of women once diagnosed with the disease. For the sake of this study, the policies to be examined are those developed by the government through its healthcare agency concerned with the cervical cancer management. Through secondary, the research targets secondary data from journals, government sites, and other literature.
Research background
In the last three decades, cervical cancer diagnosis, treatment, and prevention have developed in the UK as the government become more proactive in addressing this health concern. As a result of improved methods of diagnosis and treatment, in terms of research based approaches, the government of the UK has developed series of policies that are designed to prevent cervical cancer among adult women. Besides, several measures have also been taken to improve the health and well-being of women once diagnosed with cervical cancer (Majeed 2009). It is therefore important to examine these policies and measures that have been put in place to manage cervical cancer in the UK. Thus, this research study will explicitly examine the different policies that have been put in place prevent cervical cancer among adult women besides measures that are taken to improve the health and well-being of women once diagnosed with the disease.
Research problem statement
The requirement of efficiency and effectiveness of different policies and other initiatives in the prevention, diagnosis, and management of cervical cancer among adult women is very important in the UK. Since cervical cancer management has become a national concern, it is important it important to review the current specific policies that have been developed in the UK to prevent cervical cancer among adult women besides measures that are taken to improve the health and well-being of women once diagnosed with the disease. This analysis will be important in evaluating their effectiveness and adjustments that should be incorporated to ensure that adult women suffering from cervical cancer are properly served. At the end of the research, relevant agencies; within the UK and other parts of the globe, which are interesting in creating a comprehensive cervical management plan, will have the appropriate mechanisms that guarantees success in providing healthcare to adult women suffering from cervical cancer.
Aims and Objectives
The primary aim of this research paper is to analyse the existing literature and the UK health policies to better understand what the prevention mechanisms of cervical cancer are in the UK and to assess challenges that exist for adult women affected by the disease. The main objectives of the research study are summarized as;
- To inform stakeholders on how to reduce the incidence/mortality from cervical cancer.
- To introduce UK policies on awareness of the need for cervical cancer screening.
- To inform all adult women who are susceptible to cervical cancer.
- To explore the health and well-being of women with cervical cancer.
Research question
From the above aim and objectives, the following research questions were generated to effectively establish the policies and measures applied in the UK in managing cervical cancer among adult women. The research questions are;
- What policies have been developed in the UK to prevent cervical cancer among adult women?
- What measures are taken to improve the health and well-being of women once diagnosed with the disease?
Research significance/Rationale
The study will attempt to explicitly relate different policies and measures in the UK on cervical cancer management among adult women and their effectiveness in managing cervical cancer. The government agencies and other parties involved in cervical cancer management will use the findings of the research to improve on the current policies and other measures designed to manage cervical cancer among adult women in the UK.
Research timeline
The secondary research will take a period of two weeks and will be done through secondary research since the nature of the study is dynamic (Sprinthall 2011).
Literature Review
There are several policies in the UK to prevent cervical cancer among adult women. These policies are designed by the government agency concerned with managing cervical cancer. The first policy is the NHS Cervical Screening Programme which is under the Population Screening Programme. This policy was established by the government in the year 2015 to fast track the process of screening adult women who are at risk of getting cervical cancer.
Under this policy, adult women are encouraged to go for free cervical cancer screening in the government owned hospitals across the UK and is currently available to all women within the age of 25 and 64 years. The government encourages women to visit the screening venues through the GP automated emails and series of government sponsored advertisements and documentaries. Under the policy, women between the age of 25 and 49 years are eligible for alerts after every three years while women above 50 years are invited for screening after every five years (Carrieri & Bilger 2013).
The UK National Screening Committee (UK NSC) is mandated with the duty of assessing the effectiveness of the screening policy in order to make recommendations to the government. The main screening tests offered under the policy include cervical cytology and human papillomavirus. According to Carrieri and Bilger (2013), “cervical screening is a method of preventing cancer by detecting and treating abnormalities of the cervix” (p. 245). In relation to the screening policy, the above testing methods are meant to examine the adult women in terms of their level of exposure to cervical cancer as preventive strategy, since early detection might result in effective treatment and complete recovery of the patient.
The second policy for treating preventing cervical cancer is the Cervical Cancer Vaccination Programme. This program is also managed by the NHS and implemented with a vaccine called the Gardasil, which “protects against four types of HPV, including the two strains responsible for more than 70% of cervical cancers in the UK (HPV16 and HPV 18)” (Sabates & Feinstein 2006, p. 3008). The third policy in managing cervical cancer among adult women is the Stop Smoking Service managed by the NHS agency in the UK. Under this policy, women are encouraged to adopt positive lifestyle behaviours such as quitting smoking since this habit is known to increase chances of contracting cervical cancer (Rodvall, Kemetli, Tishelman, & Tornberg 2009).
Applying Theoretical Model
The health promotion model is often used by agencies to manage and prevent diseases. This model is designed to put in place sustainable balance in the physical, social, and psychological health of the patient. In relation to preventing cervical cancer in the UK, the model has been applied in promoting behavioural changes such as campaign against smoking, excessive alcoholism, safe sex, and continuous screening of adult women. According to Majeed (2009), “health promotion is broader and deals with dysfunction in addition to prevention of a disease” (Majeed 2009, p. 1275).
Integrated intervention model
The integrated intervention model was proposed by Dr. Nola Pender as a critical factor in facilitating creation of optimal well-being level in the society (Wu 2008). With regards to the intervention plan for cervical cancer in the UK, the model encourages positive provision of resources through private-public partnership to ensure that the healthcare personnel are in a position to provide appropriate care (Moser, Patnick, & Beral 2009). The primary objective of the model is to influence behavioural changes and alternatives for preventing cervical cancer. Basically, the model functions on the underlying assumption that adult women at the risk of contracting cervical cancer are active in managing their behaviour and participating in the acceptance of the wellness programme as indicated in the diagram below.
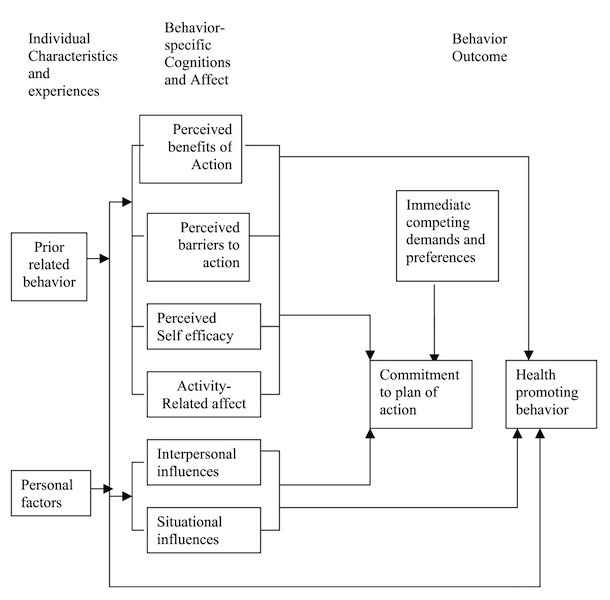
In the cervical cancer intervention for adult women who are diagnosed, the integrated model may be critical in altering and modifying patient behaviour, supporting the strategic treatment plan, and building confidence to ensure that the wellness strategies are holistic. This is achievable “through a mixture of physical, psychological, and lifestyle health education” (Whynes, Philips, & Avis 2007, p. 317). For instance, in the stop smoking campaign, the integrated model has been used to proactively influence positive behaviour chance due to its holistic nature and inclusiveness. However, the campaign has not realised the targeted results since its implementation has not embraced the aspects of personalised approach in trying to convince the adult women to stop smoking.
Conclusion, recommendations, and reflection
From the above secondary research, it is apparent that the policies in the UK on cervical cancer prevention and management have been effective in behavioural change among adult women at the risk of contracting the disease. However, there is need to increase the level of health education among this population to ensure that the current well-being strategies are inclusive and holistic (Wu 2008). The health education may be in the form of social health, environmental health, intellectual health, and physical health among others. This strategy will be instrumental in promoting positive behaviour for complete maintenance, treatment, and restoration of the health of the adult women diagnosed with cervical cancer (Whynes, Philips, & Avis 2007). There is need for unique skills on behavioural challenges, health policies, and interventions strategies, which should be carefully integrated in the unique adult women care environment to eliminate potential discontent (Carrieri & Bilger 2013).
Reference List
Carrieri, V & Bilger, M 2013, “Preventive care: underused even when free. Is there something else at work?” Applied Economics, vol. 45, no. 14, pp. 239–253.
Majeed, F 2009, “Using patient and general practice characteristics to explain variations in cervical smear uptake rates,” BMJ, vol. 308, no. 7, pp. 1272-1276.
Moser, K, Patnick, J & Beral, V 2009, “Inequalities in reported use of breast and cervical screening in Great Britain: analysis of cross sectional survey data”, BMJ, vol. 338, no. 2, pp. 2025-2034.
Rodvall, Y, Kemetli, L, Tishelman, C & Tornberg, S 2009, “Factors related to participation in a cervical cancer screening programme in urban Sweden,” Europe Journal of Cancer, vol. 14, no. 3, pp. 459–466.
Sabates, R & Feinstein, L 2006, “The role of education in the uptake of preventative health care: the case of cervical screening in Britain,” Soc Sci Med, vol. 62, no. 5, pp. 2998–3010.
Sprinthall, R 2011, Basic statistical analysis, Pearson Education, New York.
Whynes, D, Philips, Z & Avis, M 2007, “Why do women participate in the English cervical cancer screening programme”? Journal of Health Economics, vol. 26, no. 7, pp. 306–325.
Wu, S 2008, “Sickness and preventive medical behavior,” Journal of Health Economics, vol. 22, no. 11, pp. 675–689.

