Introduction
Reproduction among human beings is essential since it ensures the continuity of future generations. The male and female genital systems are involved in reproductive activities. In females, the system’s anatomy includes the external and internal genitalia.
Hormones are produced for the effective functioning of the female genitals. Additionally, they boost ovulation and menstruation, which are critical physiological processes. Poor nutritional and lifestyle choices can lead to infections and poor functioning of the body’s systems. This report discusses the anatomy, physiology, and factors associated with a healthy female reproductive system.
Anatomy and Physiology of the Body System
Female Reproductive System Structure and Functioning
The female genitalia are structurally complex but divided into external and internal parts. The external part of the system consists of a vulva, while the internal parts are the oviduct, ovaries, uterus, vagina, and cervix (Hoare and Khan, 2020). While external parts can be observed, specialized machines and instruments are needed to see internal parts. As a branch of science, anatomy helps identify and understand the structure of the different parts of the female reproductive system. Therefore, the following sections present the anatomy and functions of the female genitalia.
External Genitalia
The vulva is made up of the labia majora, labia minora, clitoris, hymen, and urethral opening, which protects the internal genitalia. The labia majora, also known as the major lips, enclose and prevent infections of the external genitals (Feng and Liu, 2022). They are capable of fulfilling their purposes because they have hair, sweat, and oil-secreting glands.
Meanwhile, the labia minora have thin skin that reacts to anything that comes into contact with them, leading to swelling or irritation (van der Vaart et al., 2022). Labia minora and majora meet at the clitoris, which has a prepuce on it, which is easy to stimulate. On the other hand, females pee through an opening to the urethra. Figure 1.0 below shows the anatomy of the external female genitalia.
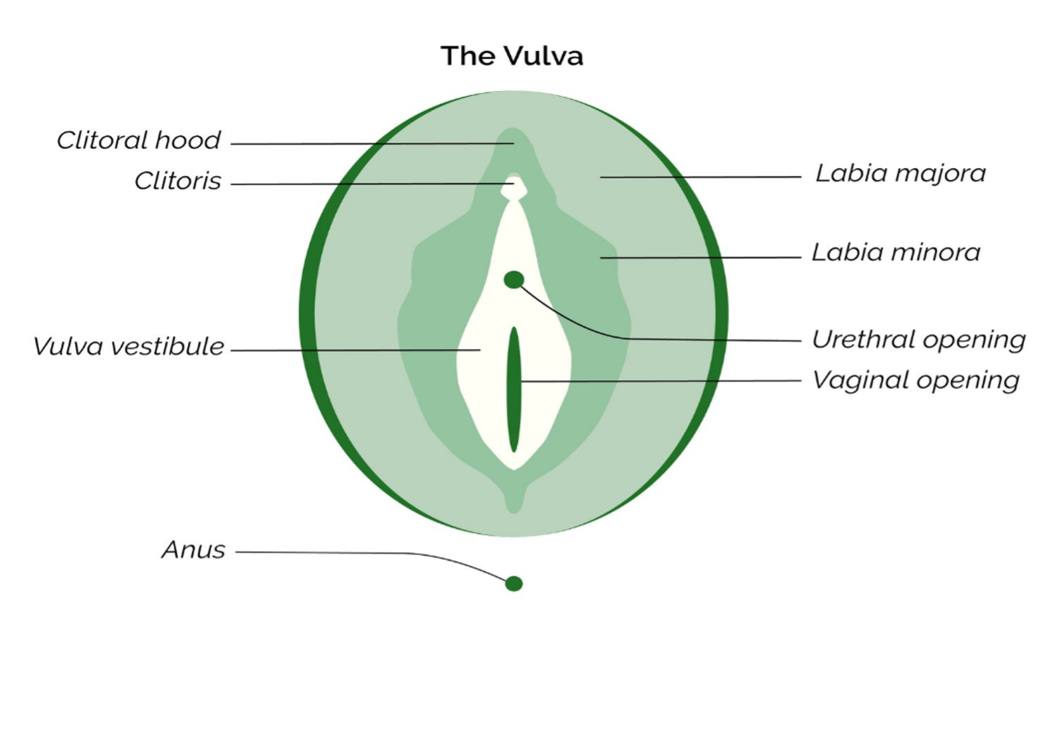
Internal Genitalia
The internal female genitalia are essential for physiological processes such as ovulation and menstruation. The first internal genital is the vagina, which has a muscular canal that joins the uterus to the outside body (Septadina, 2023). The vagina widens for easy delivery and has membranes that produce mucus to reduce friction along its length (Hoare and Khan, 2020). Sperm enters the uterus, and menstrual flow leaves the uterus through the second part, called the cervix. This organ prevents tampons and other objects from entering the body. It is important to note that during vaginal childbirth, the cervix is also responsible for dilatation.
The uterus is the third internal structure of the female genital tract and consists of the mucosa, myometrium, and serosa. The part is structurally specialized for holding the fetus during pregnancy. The uterus is a hollow, pear-shaped organ with an expanding body that comfortably accommodates the growing fetus.
On both sides of the uterus, the ovaries are small, located, and form the fourth genitalia (Feng and Liu, 2022). The eggs and the hormone progesterone are formed in the ovary and are essential for fertilization and menstruation. The fallopian tubes, or oviducts, are the last internal genitalia that connect the ovaries to the uterus. Eggs produced by the ovaries travel through the fallopian tubes, where they are fertilized before moving to the uterus.
Figure 2.0 below shows the internal anatomy of the female genitalia.
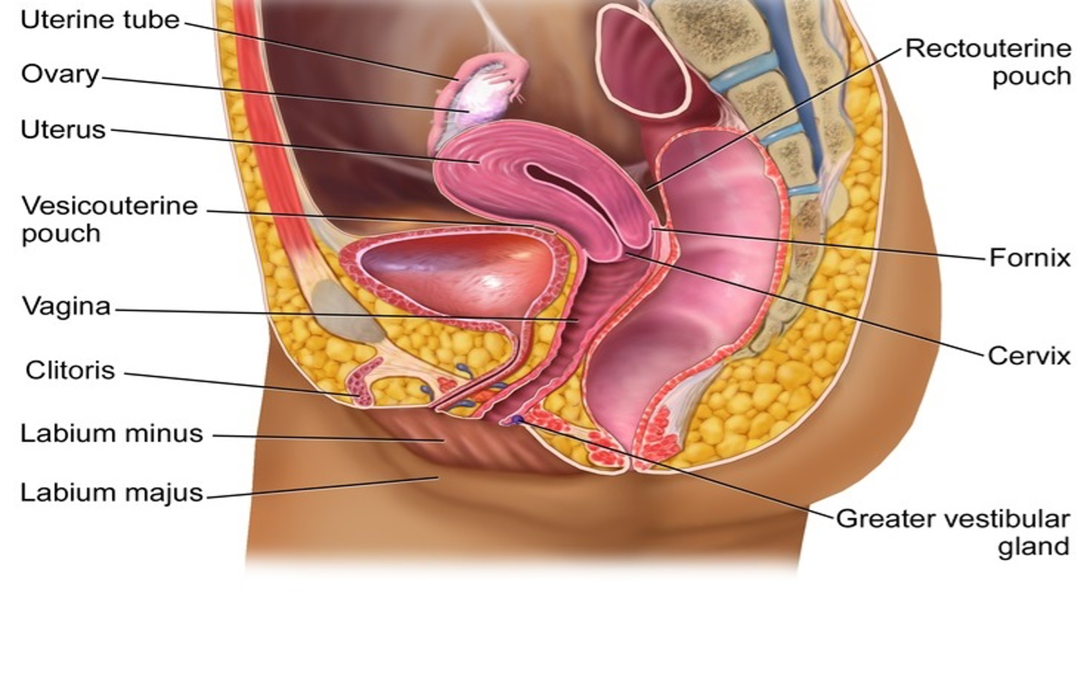
Physiology and Functioning of the Reproductive System
The functioning of the body system involves the ovarian and menstrual cycles and hormonal regulation. The changes in the ovaries through which the follicle matures, and the ovum is shed, with the corpus luteum developing, are referred to as the ovarian cycle. The process occurs within an average of 28 days and involves two interrelated processes, initiating changes in the female’s oocytes and ovarian follicles (Chen et al., 2022). Oogenesis and folliculogenesis are the two interrelated processes that occur during the ovarian cycle.
Female gametes are crucial for the reproduction process and sexual intercourse among women. Oogenesis is the initial stage of the ovarian cycle that involves the actual production of the female gametes. The phase begins with the formation of oogonia, which are ovarian stem cells (Feng and Liu, 2022).
The latter are formed during fetal development and undergo mitosis, a process similar to spermatogonia in the testes (van der Vaart et al., 2022). Primary oocytes are formed in the ovary before birth and are later arrested in meiosis I. The stage resumes once a person reaches puberty and continues until near menopause.
Physical and emotional changes in women often begin at puberty, the onset of reproductive maturity. Puberty begins when the ovary releases an oocyte: a process called ovulation (Septadina, 2023). Before the start of ovulation, luteinizing hormones are released to trigger a resumption of meiosis in the primary oocyte.
The latter transitions to a secondary oocyte, which involves two unequal cells, with the smaller one disintegrating (Feng and Liu, 2022). If a woman engages in sexual intercourse, a sperm may penetrate the secondary oocyte barrier. Therefore, the meiosis of the secondary oocyte is completed, leading to the formation of an ovum.
The union of a haploid sperm and a haploid ovum results in fertilization. The latter leads to the formation of a diploid cell, the zygote, which grows into a new offspring. It is essential to note that haploid sperm contribute only to the genetic composition of the new offspring (Chen et al., 2022). Therefore, the cytoplasmic organelles that support the zygote to develop into an embryo come from the mother. Additionally, the mitochondria, which supply the developing embryo with energy, are of maternal origin.
Oocytes and their surrounding cells, which form the ovarian follicle, undergo a process called folliculogenesis. The process leads to ovulation and death of multiple follicles after every 28 days (Septadina, 2023). Folliculogenesis involves the transition of the primordial follicle to the corpus luteum.
The degeneration of the corpus luteum triggers endometrial disintegration, leading to menstruation if fertilization does not occur. However, if the haploid ovum is fertilized, the corpus luteum maintains the endometrium for implantation and pregnancy (Chen et al., 2022). Hormones regulate the growth of follicles and menstruation in females.
The anterior pituitary gland of the human hypothalamus produces the gonadotropins that initiate ovulation and menstruation. Follicle-stimulating hormone (FSH) and luteinizing hormone (LH) are responsible for the processes. FSH stimulates follicular growth and increases follicular diameter (Feng and Liu, 2022). On the other hand, LH stimulates the production of estradiol hormone by the theca and granulosa cells (Septadina, 2023). Additionally, LH stimulates estrogen production, increasing plasma estrogen concentration.
Another vital hormone produced during ovulation is progesterone, which is essential for maintaining pregnancy. The increased LH levels cause changes in granulosa and theca cells, leading to the formation of the corpus luteum (Feng and Liu, 2022). Progesterone is produced by the luteinized granulosa and theca cells.
The increased progesterone levels are associated with negative feedback that suppresses LH and FSH production, halting folliculogenesis and ovulation. If pregnancy fails to occur within 10 to 12 days, the corpus luteum degenerates, reducing progesterone levels (Daghash et al., 2022). Reduced progesterone stimulates FSH and LH production, initiating new tertiary follicles, and the process repeats in cycles.
Menstruation
Menstruation involves cyclic changes in the production of hormones, and it is evident during the first stage of puberty. Once pregnancy fails to occur, the levels of estrogen and progesterone are reduced. The latter leads to the production of prostaglandins, which constrict spiral arteries (Septadina, 2023). Consequently, blood and oxygen supply to the endometrium are cut due to the continuous spasms along the uterine walls.
The absence of oxygen on the outer lining of the endometrium causes it to die. The contraction of spiral arteries can trigger blood clotting, which is then broken down by the enzyme plasmin. The blood and dead matter flow out through the vagina within 2 to 6 days. The process is repeated monthly in cycles of hormonal production.
Factors Associated with Female Reproductive Health
Nutritional Factors
Reproductive health is of the essence for the proper functioning of the human body. Various nutritional and lifestyle factors are associated with a healthy female reproductive system. Sufficient nutrients are needed for hormonal balancing, reproductive disease prevention, and the overall well-being of females. There are various requirements for the essential physiological processes that take place within the system (Antony, Vora, and Karmarkar, 2022). Although there are general nutrient requirements for females, these may vary with age, underlying health conditions, and other factors.
Neural tube defects (NTDs) can be detrimental to the brain and spine development of the fetus. NTDs are associated with insufficient folate and Vitamin B nutrients in the female reproductive system. Folate and Vitamin B are essential for DNA repair and synthesis, thereby preventing NTDs (Antony, Vora, and Karmarkar, 2022).
Women are encouraged to take up leafy green vegetables, legumes, and fortified cereals, among others, for good reproductive health. Excess bleeding during menstruation and childbirth is another problem with the body’s system. Consequently, foods rich in iron, including red meat and fish, can help in hemoglobin production (Lindberg, Bell, and Kantor, 2020). Iron-rich nutrients are essential for a sufficient oxygen supply in the reproductive system.
Other nutritional factors important for female reproductive health include calcium and Vitamin D. These nutrients are crucial for healthy bones that support the various organs of the system. Bone density loss is common during adolescence and menopause, and can lead to poor support and movement (Lindberg, Bell, and Kantor, 2020). Therefore, females are advised to consume nutrient-rich foods such as dairy products and fish to support strong bones in the reproductive system.
Additionally, exposure to the sun strengthens bones, as it is a source of Vitamin D. Hormones FSH, LH, and progesterone, on the other hand, can be improved by eating foods rich in protein (van der Vaart et al., 2022). Females should consider taking sufficient amounts of iron, vitamins B and D, and calcium to maintain a healthy reproductive system.
Lifestyle Factors
Physical activity, stress and weight management, sleep, and substance use and abuse are major lifestyle factors that determine the health of a female reproductive system. Women are encouraged to engage in physical activities for weight management, stress reduction, and to counter conditions such as polycystic ovary syndrome (PCOS) (Chávez, Jaworsky, and Basu, 2023). Additionally, the positive effects of physical activity on mental health support adequate reproductive hormone production (Marinelli et al., 2022). Although physical exercise promotes health, excessive physical activity without proper nutrition can disrupt the menstrual cycle (Marinelli et al., 2022). Therefore, the lifestyle factor can only be considered when one consumes sufficient nutrients.
Stress and various other traumatic situations are associated with irregular menstrual cycles. Consequently, engaging in stress management activities such as meditation, yoga, and mindfulness helps maintain hormonal balance and supports a healthy menstrual cycle (Marinelli et al., 2022). Similarly, weight management activities such as a balanced diet, regular exercise, and sufficient sleep help prevent PCOS and its associated problems during ovulation (Chávez, Jaworsky, and Basu, 2023). Furthermore, involvement in substance abuse, including smoking and excess alcohol consumption, can hinder hormonal production and regulation, exacerbating risks of infertility (van der Vaart et al., 2022). A healthy lifestyle is associated with consistent menstrual cycles and reduced cases of miscarriage.
Conclusion
The female reproductive system plays a central role in reproduction and sexual intercourse. The system’s anatomy comprises the external and internal genitalia. While the vulva is the only external part, the internal ones are the vagina, cervix, fallopian tube, and uterus, each with a specialized function. The system’s physiological processes involve ovulation and menstruation, which occur in cycles. Fertilization of the ovum leads to pregnancy, while failure causes menstruation. Nutritional and lifestyle factors should be considered for optimal system function.
Reference List
Antony, A.C., Vora, R.M. and Karmarkar, S.J. (2022) ‘The silent tragic reality of Hidden Hunger, anemia, and neural-tube defects (NTDs) in India‘, The Lancet Regional Health – Southeast Asia, 6.
Chávez, G., Jaworsky, K. and Basu, A. (2023) ‘The effects of plant-derived phytochemical compounds and phytochemical-rich diets on females with polycystic ovarian syndrome: A scoping review of clinical trials’, International Journal of Environmental Research and Public Health, 20(15), pp. 6534–6534.
Chen, Y.-Y. et al. (2022) ‘Single-cell transcriptomics of staged oocytes and somatic cells reveal novel regulators of follicle activation‘, Reproduction, 164(2), pp. 55–70.
Daghash, S.M. et al. (2022) ‘Histological and hemodynamic characterization of corpus luteum throughout the luteal phase in pregnant and non-pregnant buffalos in relation to nitric oxide levels based on its anatomical determination‘, Frontiers in Veterinary Science, 9.
Feng, T. and Liu, Y. (2022) ‘Microorganisms in the reproductive system and probiotic’s regulatory effects on reproductive health‘, Computational and Structural Biotechnology Journal, 20, pp. 1541–1553.
Hoare, B.S. and Khan, Y.S. (2020) Anatomy, Abdomen and Pelvis, Female Internal Genitals. Treasure Island (FL): Stat Pearls Publishing.
Lindberg, L.D., Bell, D.L. and Kantor, L.M. (2020) ‘The sexual and reproductive health of adolescents and young adults during the COVID‐19 pandemic‘, Perspectives on Sexual and Reproductive Health, 52(2).
Marinelli, S. et al. (2022) ‘Female obesity and infertility: outcomes and regulatory guidance’, Acta Bio Medica: Atenei Parmensis, 93(4), p. e2022278.
Septadina, I.S. (2023) ‘An overview of the female reproductive system: A narrative literature review’, Sriwijaya Journal of Obstetrics and Gynecology, 1(1), pp. 16–23.
Smart, O. (2023) The Nu Guide to Anatomy 101. Nu Intimate Balm.
van der Vaart, L.R. et al. (2022) ‘Female sexual functioning in women with a symptomatic pelvic organ prolapse; a multicenter prospective comparative study between pessary and surgery‘, The Journal of Sexual Medicine, 19(2), pp. 270–279.

