Introduction
The U.S. is among countries that are currently dealing with the rising cases of cancer patients. This disease is responsible for many death cases reported among people suffering from long-term sicknesses due to the lack of an evidence-based pain management mechanism in various health facilities in not only America but also other parts of the world. As this paper reveals, the application of Kurt Lewin’s change framework accompanied by cooperation among medical practitioners and nurses in the emergency department (ED), including patients and their families, may help to change this situation. Overall, instances of fatalities reported among people suffering from advanced cancer will be reduced significantly.
The Proposed Change
Although the goal of health facilities is to provide quality services, concerns have been raised regarding delayed attention to patients undergoing pain, especially those presenting with chronic diseases during their admission. Many of them spend a considerable time trying to secure their way to hospital beds. It is alarming that the long waiting time witnessed during the admission process exposes patients to extensive pain because service delivery in a significant number of medical centers begins only after this procedure is completed. In particular, according to a study by Zoëga, Fridriksdottir, Sigurdardottir, and Gunnarsdottir (2013), more than 33% of citizens from Iceland are expected to suffer from cancer.
Currently, approximately 60% of patients experiencing advanced cancer have to battle with extensive pain among other complications associated with this condition (Zoëga et al., 2013). Chances of death resulting from pain among those who need emergency services are high, especially when they cannot be attended to immediately their families or friends bring them to hospitals due to the long queues witnessed in virtually all patient admission points. According to Jho et al. (2014), more than 70000 people in every 200000 patients suffering from advanced cancer in Korea succumb due to pain following delayed service delivery at the admission section.
As a result, the above situation may worsen if the nursing sector does not come up with a mechanism for dealing with pain during patient admission processes in the emergency department. The article by Jho et al. (2014) indicates the degree to which many health facilities have inadequate pain control measures as recorded among roughly 40% of patients who are admitted suffering from advanced cancer.
Although Jho et al. (2014) confirm the possibility of effectively managing pain that is reported among this class of patients, their strategy does not focus on the way this situation is witnessed in many patient admission points. Hence, having a pain management strategy, which emphasizes cancer patients in need of emergency services, may go a long way in assuring them of recovery even before they are admitted, regardless of the hospitals they visit.
How this Solution Aligns with My Organization’s Mission, Vision, and Values
I work as a nurse in Hospital X that is located in Howard County, Maryland, which is among the richest regions in the U.S. This facility’s mission is to provide patients with quality and well-timed services with a view to boosting the standards of health set for Maryland. Its vision is to have zero cases of deaths reported among cancer patients due to the pain associated with this disease, especially when it is found to be in advanced stages.
Hospital X upholds values such as fairness regarding service delivery and confidentiality when handling patients’ records. Being a region dominated by wealthy citizens, Howard County is expected to have a huge number of cancer patients due to the anticipated lifestyle triggers such as feeding on junk foods and the lack of exercise. According to the Maryland Department of Health (2017), almost 30000 new cases of cancer were recorded in 2014. Death cases reduced by almost 2% whereby only about 160 patients succumbed out of a population of 100000 admissions made in the period between 2004 and 2013 (Maryland Department of Health, 2017).
Although pain is not documented as one of the causes of death among cancer patients in Howard County, its proper management immediately they are brought to health facilities’ emergency departments is in line with this organization’s mission of providing well-timed and quality services. According to a study by Gropelli and Sharer (2013), having an operational pain management plan contributes significantly to reducing mortality levels as captured in this medical center’s vision of realizing zero death cases. In addition, attending to all cancer patients in need of emergency services even before they are admitted is an indication of the priority given to these people because of the pain they undergo, especially when they have to be forced to queue to provide their details in the admission point. Adopting this pain management strategy aligns with the values of ensuring fairness when attending to the sick.
Change Model
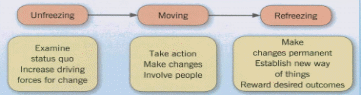
Kurt Lewin’s planned change theory is applicable to the current situation. As shown in Figure 1 below, this framework has three levels of implementing change, namely, unfreezing, moving, and refreezing. The unfreezing phase indicates the extent to which reforms are needed. In the current context, the issue of pain management at admission points among patients suffering from advanced cancer is in this stage because many health facilities lack effective measures.
In the moving phase, transformations begin by executing the proposed strategies (Mitchell, 2013). During the refreezing stage, a state of equilibrium is reached whereby the implemented reforms are regarded as standard measures to be adopted continuously. In this case, the suggested pain management is expected to be embraced and treated as a routine in all healthcare facilities.
Role of Various Individuals
Implementing the proposed change requires the input of several classes of people who include medical practitioners, nurses, patients, and their relatives. For instance, complaints from patients act as the basis upon which agents such as medical practitioners and nurses realize the need for initiating change in the way pain is managed at the admission point. Hence, health centers will implement this reform by allocating doctors and the appropriate equipment to help in attending to cancer patients before they secure admission in the emergency unit.
Nurses will play a key role in managing this change by offering the necessary care while at the same time facilitating the capturing of medical records in the respective hospitals’ computerized systems. This combined effort will enhance the time spent in the admission room, hence reducing instances of death resulting from pain among these patients. Family members will also be required to offer the appropriate material and emotional support to their ailing loved ones to enhance their recovery before and after they are admitted.
Conclusion
Almost all service delivery points in medical facilities welcome ailing people who have to endure the pain brought about by their diverse sicknesses. Delayed service delivery, especially following long queues at the admission point, may increase the number of fatalities recorded. Hence, the implementation of a pain management strategy in the emergency unit to help cancer patients before they are admitted is viewed as a move in the right direction. This measure is in line with Kurt Lewin’s change theory. However, it can only be effective when medical doctors, nurses, patients, and their family members collaborate to ensure smooth service delivery and, consequently, speedy recovery processes.
References
Gropelli, T., & Sharer, J. (2013). Nurses’ perceptions of pain management in older adults. MEDSURG Nursing, 22(6), 375-382.
Jho, H. J., Kim, Y., Kong, K. A., Kim, D. H., Choi, J. Y., Nam, E. J.,… Park, E. J. (2014). Knowledge, practices, and perceived barriers regarding cancer pain management among physicians and nurses in Korea: A nationwide multicenter survey. PLoS ONE, 9(8), 1-7.
Maryland Department of Health. (2017). 2017 cancer data. Web.
Mitchell, G. (2013). Selecting the best theory to implement planned change. Nursing Management, 20(1), 32-37.
Zoëga, S., Fridriksdottir, N., Sigurdardottir, V., & Gunnarsdottir, S. (2013). Pain and other symptoms and their relationship to quality of life in cancer patients on opioids. Quality of Life Research, 22(6), 1273-1280.

