Abstract
Pressure ulcers are restricted skin or fundamental tissue harm resulted by long-term tension or shear. The most widely recognized portrayals are those that happen on the external layers of the coccyx, hips, elbows, lower legs, and knees. Approximately 2.5 million individuals in the United States experience the aftereffects of bedsores across all medical services facilities. 0.4% to 38% of them are in intense consideration medical clinics, 0% to 17% in primary care, and 2% to 24% in extensive care (Ahn et al., 2016). By 1860s, Florence Nightingale demonstrated, that it is a medical attendant’s fault for an out of commission patient to create bedsore (Mccullough, 2019). Subsequently, the prior researchers assumed basic parts in the momentum information and controls. In the nineteenth century, a French physician known as Jean-Martin Charcot who examined illnesses saw that patients created sores on different body parts and passed on after a specific period. Jean-Martin Charcot was the first one to describe that pressure ulcers can be prevented in case of proper management and timely diagnosis.
Katzengold and Gefen propose the utilization of doughnut molded gel head supports to help prevent the pressure on the heads of patients while lying in clinic. The mechanical practices of the gel substance in the doughnut molded head were estimated for eight subjects in a research facility in Massachusetts. The mathematical measurements demonstrated that the doughnut molded gel head uphold does not work in a way that is better than simple clinical foam. The issues causing issues in the combining preventive measures in clinical practice are caused by factors such as diagnostic and treatment methods, diet, ethical concerns during care, and cultural beliefs about the condition. For better outcomes, the prevention procedure need to include clinical informatics to combine with social discernments.
Introduction
Pressure ulcers are generally situated in the skin and hidden tissues, over a bone layer, brought by sustained pressure, shear, as well as the combination of these. These wounds are a significant general medical problem and affects overall wellbeing of the country because of its epidemiological, monetary and socio-cultural aspects. The decrease and avoidance of cases are one of the principle goals in wellbeing associations. Condition awareness and appropriate analysis are key perspectives for the avoidance of pressure ulcers.
The establishments of present-day medical care depend on treating patients with decency, respect, and keeping their dignity. There are several challenges when coping with the incidence and severity of the disease. Some of them incorporate resistance from the patients and their cultural conviction frameworks. Furthermore, the authorities experience issues deciding on the correct conventions to follow because of the questionable literature. To completely battle the pervasiveness of pressure ulcers injury, it is essential to consider both the moral and cultural elements since the treatment requires an interdisciplinary approach. The objective of this paper is to introduce a reasonable cultural viewpoint and mathematical measurements on the conventions for management of the injuries. It gives the factual data on the event of bedsores and analyzes whether there are methods which can be utilized in forestalling pressure ulcers.
Prevention Protocol for Pressure Ulcers
The topic area of this study is the prevention and management of pressure ulcers. Pressure ulcers are skin injuries, which can bleed or produce a poisonous substance. These sore areas usually appear in bony spots such as hips, tailbone, ankles, and heels. Symptoms of pressure ulcers include changes in skin color, temperature, and swelling. Emergency departments have special protocols detailing the preventative measures and treatment for patients with such injuries. The subject of this study is the development of pressure ulcers. The problem is that older people have a high risk of developing pressure ulcers. Blood flow obstruction, precipitated by long periods of immobility and poor hydration, can lead to excessive pressure on the skin, ultimately damaging it. The population of this study incorporates people older than 60 years who are likely to have risk factors for pressure ulcers. The subsequent thesis is: the implementation of an appropriate pressure ulcer protocol may reduce the risk of getting these lesions within three days. The most common way of developing a pressure ulcer is by applying too much static pressure on a certain part of the body without changing the point of pressure. Most of these processes happen while a patient is either sitting or lying for an extended period of time (Baron et al., 2016). Older people have a higher risk of developing a pressure ulcer since their overall mobility is limited. Subsequently, blood flow does not reach pressured areas, which results in a lesion (Kwong et al., 2016). The goal is to create a protocol in a hospital emergency department that would relieve patients of sore areas developing into pressure ulcers within three days.
The reason why this topic is worthy of note lies in the apparent easiness of preventing pressure ulcers. If lesions occur after the obstruction of blood flow, it may be possible to resolve this issue without any medical assistance by simply changing the lying position so that bone pressure would shift to another area. However, in most cases, patients report pain only after a pressure ulcer has developed (Baron et al., 2016). This means that it is too late for preventative measures. Therefore, a protocol should be written that would specifically pinpoint risk factors and ways of managing them, as, under normal circumstances, it is easy to miss the warning signs. Accomplishing this goal would empower nursing staff with the knowledge of pressure ulcer risk factors. When delivering care to older patients, medical personnel focuses on the most immediate issues, for instance, spinal cord injuries. However, the treatment for such traumas is immobility, which is the primary risk factor (Kwong et al., 2016). Exploring this issue would raise awareness of such complications and prevent many older patients from blood flow obstructions.
The target population incorporates nurses who gain knowledge and the old patients who are relieved of the risk of struggling with a pressure ulcer. Nurses benefit because they learn to spot warning signs before patients start feeling pain. In their turn, older people will be able to spend a long time lying without the risk of developing a pressure ulcer. Both these groups will be prime beneficiaries of the implementation of the preventative protocol. Altogether, it should be evident that treatment that necessitates prolonged immobility may result in skin injuries. They happen due to the lack of attention drawn to the sufficient blood flow and distribution of bone pressure. Once the protocol for preventing pressure ulcers is implemented, both the medical personnel and the older patient will experience improvement since no unexpected injuries will appear due to a long time spent lying.
Historical and Mathematical Perspectives of Inquiry: Prevention of Pressure Ulcers
This paper is written to deliberate on a condition known as pressure ulcers, also called pressure sores or bedsores. They are injuries to the skin and underlying tissue, caused by prolonged pressure on the skin area. They can occur to anyone, but usually affect patients who lie in bed or sit in a chair for extended periods of time. They remain a major health condition which a significant population of adults can face. Hospitalization cases resulting from the condition have been on the steady rise in recent times among the ageing population. A report by Ahn et al. (2016) indicates that over 2.5 million people in the United States suffer from bedsores across all healthcare facilities. This population consists of 0.4% to 38% in acute care hospitals, 0% to 17% in home-bases care, and 2% to 24% in long term care facilities (Ahn et al., 2016). Therefore, a concerted effort should be made in preventing their occurrence to avert the treatment costs and postoperative difficulties experienced by some patients.
The objective of this essay is to present a clear historical and mathematical perspective on the topic under study. The level one historical question to be answered in the paper is what the history of pressure ulcers is. On the other hand, the level two historical question to be answered is what the existing protocols for averting the development of the lesions are. The level one mathematical question to be answered in the essay is what the statistical pieces of evidence of the occurrence of bedsores are. Similarly, the level two mathematical question to be responded to is whether there are protocols which can be used in preventing pressure ulcers.
Historical Perspective
Pressure ulcers have been viewed as a disease since a long time ago. An article by Mccoulough (2019) reports that the condition was observed in ancient Egyptian women about five thousand years ago. The Egyptians would use remedies such as honey, mouldy bread, meat, animal and plant extracts, copper, and zinc (Mccoulough, 2019). Another French surgeon, Ambrose Pare (1510-1590), perceived that man can only treat a wound but the healing process is done by God (Mccoulough, 2019). Ambrose later joined the army and used his medical knowledge in curing wounded soldiers of pressure ulcers by recommending good nutrition, pain relief, and debridement. Therefore, there is a rich background of useful knowledge in mathematics and other technical disciplines such as medicine.
Referring to the Brown-Sequard syndrome theory by Mauritian physiologist known as Charles Brown-Sequard (1817-1894), pressure inhibits blood circulation which results in bedsores. Brown-Sequard proved that avoidance of pressure in guinea pigs with injured spinal cords and the lesion does not develop, and that present ulcer heals when pressure is withdrawn (Mccoulough, 2019). The founder of present-day nursing, Florence Nightingale adhered to stringent repositioning of bend-bound patients while nursing them. Mccoulough (2019) reports that Florence Nightingale indicated in 1859, that it is a nurse’s fault for a bedridden patient to develop bedsore. Thus, the earlier scientists played critical roles in the current knowledge and disciplines.
In the nineteenth century, a French doctor known as Jean-Martin Charcot who studied diseases noticed that patients developed lesions on various body parts and died after a certain period. According to Zaidi and Sharma (2020), the doctor opted to name the condition “decubitus ominous” by which he meant death was inevitable for someone who developed lesion. In Charcot’s perspective, there were other causative factors of bedsore alongside pressure. He described a model known as neurotrophic theory which maintained that central nervous system damage directly caused bedsore (Zaidi & Sharma, 2020). This framework formed the basis of modern-day prevention or diagnosis of pressure ulcers due to its emphasis on risk factor assessment and proactive response to bedsore cases. Furthermore, the theory underscored the fact that not all pressure ulcers cases result in death since the condition can be mitigated.
Mathematical Perspective
Although medical practitioners recommend frequent repositioning of bed-bound patients in order to prevent them from developing bedsores, other scholars argue that the practice can be unreliable. For instance, Katzengold and Gefen (2019) state that the method has limitations based on “the required body posture during operation, mechanical ventilation, and connection to other life-support equipment” (pp. 1398-1399). Furthermore, nurses sometimes use inappropriate techniques and materials to reposition certain parts of patients such as the head and neck. They often use blankets and towels. This essay will, therefore, propose a technique used by the research done by Katzengold and Gefen to highlight the mathematical perspective of preventing bedsores.
Katzengold and Gefen propose the use of donut-shaped gel head supports to support patient heads while lying in hospital. Acceding to Katzengold and Gefen (2019), “by so-called “off-loading” the occiput, that is, shifting the head-weight forces from the central occipital region to other more peripheral head regions.” (p. 1399). The modelled geometry of the medical devices in research done by Katzengold and Gefen (2019) are shown in Figures 1 and 2.
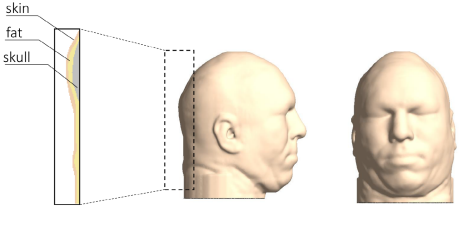
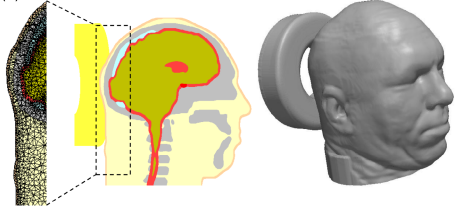
The research adopted the mechanical behavior of the skin and fatty tissues of the scalp and skull bone. Each tissue type was represented by the Mooney-Rivlin constitutive model:
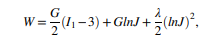
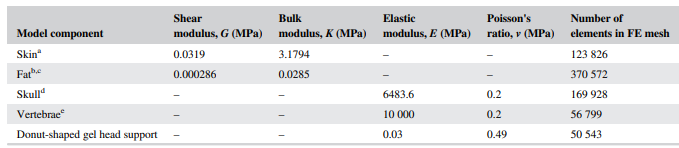
Where W represent the strain energy density, I1 is the first invariant of the right Cauchy-Gree deformation tensor, J is the determinant of the deformation gradient tensor, G is the shear modulus and λ is Lame’s first parameter that can be converted to other frequently used elastic properties shown in Figure 3: elastic modulus E, the bulk modulus K, and Poisson’s ratio ν.
The elastic modulus is given as:
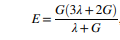
While the bulk modulus is calculated as follows:
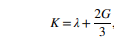
Whereas the Poisson’s ratio is calculated by the following formula:
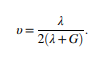
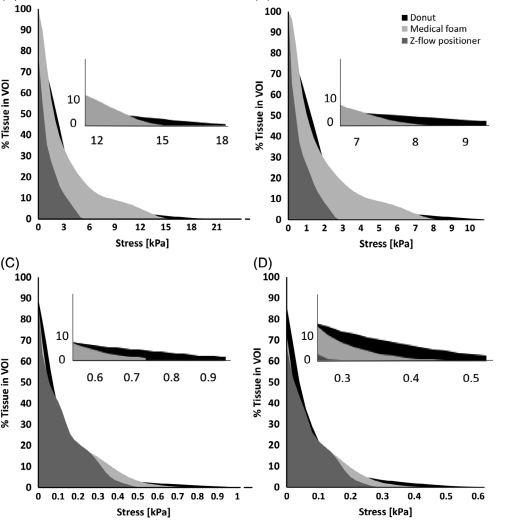
The mechanical behaviors of the gel substance in the donut-shaped head support were measured for eight subjects in a laboratory in Massachusetts. The pressure distributions of the back of the head are represented in the Figure below:
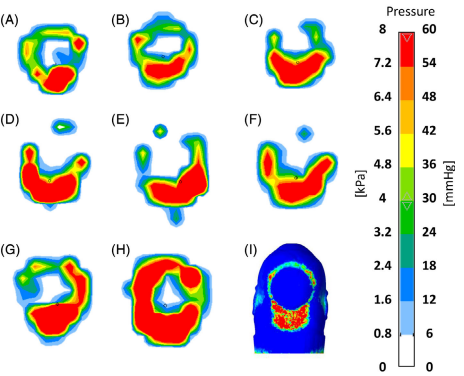
Figure 5 comprises of different graphs of stress level of the skin and fat tissue when positioned with different head supports.
Cultural and Ethical Perspectives of Inquiry: Prevention of Decubitus Sores
Pressure ulcers are localized skin or underlying tissue damage as a result of long term pressure on body parts with bony prominence. The most common representations are those that occur on the outer layers of the coccyx, hips, elbows, ankles, and knees. They occur because of the pressure on soft tissues resulting in partial or complete obstruction of blood flow to that area. Moreover, shear can equally play a significant role by pulling on vessels that supply blood to the skin. It is common in individuals who are not regularly moving as those bedridden or in wheelchairs. However, other factors can influence skin’s tolerance to shear which eventually lead to pressure ulcers. Such factors include microclimate, protein-calorie, and diseases that reduce skin sensitivity or fluid flow to the skin (Atkinson & Cullum, 2018). It is often preventable and treated although it is somewhat difficult for critically ill patients. Cultural and ethical perspectives have shaped the prevention and treatment of pressure sores because of the challenges that they present in the implementation of clinical practices.
This paper will present cultural and ethical perspectives of inquiry on the management of decubitus sores and the challenges surrounding it. The level one cultural question is on the current challenges from people’s way of life and beliefs. On the other hand, the level two ethical question aims to explain the ethical dilemmas involved in prevention or treatment mechanisms. The former concern involves the collective role of all the stakeholders in addressing the problem. The latter focuses on identifying the moral shortcomings that prevent the smooth implementation of policies.
Cultural Perspective of Inquiry: Prevention of Pressure Ulcers
In contemporary society, considerable dogma drawn from cultural standpoints has overrun evidence-based results in preventing this health condition. The therapeutic measures towards its treatment are mostly empirically drawn from anecdotal experience. Essentially, the treatment process of pressure ulcers is somewhat problematic due to multiple comorbidities of ill persons and the relatively long duration of chronic pressure ulcers. Moreover, difficulties arise because of a physician’s unfamiliarity with the available approved treatment options (García‐Sánchez et al., 2019). The issues causing dilemmas in the integration of preventive measures in clinical practice are primarily due to risk assessment, treatment, diagnosis procedures, and nutritional support.
In the implementation of some of the precautions such as pressure relief, some health officers faced resistance from the patients. The recommendations to change the position of patients after every two or four hours is problematic for long term practices. In nursing homes, the caregivers have an easier time identifying the triggers early because they are familiar with the needs of the patients (Lavallée et al., 2018) However, some residents are opposed to the routines especially at night. They feel that it is a disturbance from the stuff constantly repositioning them. Moreover, others also resist adherence to nutritional directives. The patients refuse to take the meals, fluids, or prescribed barrier creams. Some were non-compliant due to incapacitated mental function such as those suffering from brain injury (Lavallée et al., 2018). However, others understood the essence of the procedures but still opted to follow the guidelines.
Other measures that can be used include triggering a cultural change to invoke the required response. One such way is through education, from the nurses to the patients themselves about the diagnosis, prevention, treatment, and fatalities of decubitus ulcers. In conducting the training, there is a need for enforcement and support from the senior management thus boosting professional growth. Despite the idea that increased education does not play a significant role in the development of useful practices, it increases awareness. Consequently, the clinicians can successfully identify risks through the application of such tools as Norton and Braden scale (Stadnyk et al., 2018). The quality care and prevention protocols thus involve clinical informatics to blend with cultural perceptions for better results.
Ethical Perspective of Inquiry: Prevention of Pressure Sores
Pressure ulcer prevention protocols and management require an interdisciplinary technique. Some sections of the available measures are highly routinized although customization is necessary to address the needs of individual patients. For health professionals involved either directly or indirectly, numerous ethical concerns may arise. The issues usually originate from accountability which can be about policies and clinical perspectives (Carlson & Gunningberg, 2017). It is therefore imperative for clinicians to integrate ethical theories and principles to design frameworks that will address the ethical dilemmas. Most organizations are currently striving to meet the bare threshold of ethical clinical practices (Carlson & Gunningberg, 2017). However, there are issues with understaffing which lead to poor care of the vulnerable members. As a result, the care is substandard and provides a suitable environment for the development of skin injuries.
However, the theories have been criticized to be rather general and basic, which cannot fully address all the concerns. Alternative approaches include experimental learning and virtue ethics which provide comprehensive guidance inclusive of a pluralistic approach to solving the challenges (García‐Sánchez et al., 2019). There are cases where the patients’ or their family’s beliefs hinder the prevention of decubitus ulcers. One such case is when the family believes that miracles do happen. Thus, in the case of fatalities, they are reluctant to accept clinical advice from healthcare professionals. As such, the caregivers are forced to administer a treatment which does not help in the management of the illness (Lavallée et al., 2018). Others opt for nutraceuticals which are not approved by regulatory bodies or whose effectivity or side effects are unknown. Moreover, some physicians are reluctant to perform surgery for chronic cases such as diverting colostomy. The hesitation is due to the slim chance of success of such kind of procedure after analyzing the risk-to-benefit ratio.
Other controversies are arising from different literature on some preventive mechanisms. One such contentious issue involves nutrition especially on the best mode of nutritional assessment for patients at risk. For instance, there is no agreed-upon specification on the value of serum albumin where some researchers claim that low levels increase risk while others do not (Karpegard & Mordoch, 2019). The AHRQ bedsore prevention directive states that albumin of less than 3.5gm/dl raises risk. However, another study suggests that dietary protein consumption is a somewhat independent predictor of the stated value (Lavallée et al., 2018). The clinicians are thus faced with a dilemma on which side to choose and which will be less detrimental to the patient. Other conflicting texts involve the role that protein-calorie malnutrition plays in the promotion of decubitus ulcers.
Conclusion
Pressure ulcers happen due to the tension on delicate tissues bringing about hindrance of blood stream to a particular region to some extent. Additionally, shear can similarly impede vessels that supply blood to the skin. The pressure ulcers estimation delineated that skin tissue are ordinarily exposed to more prominent pressure esteems that the fat layer. Cultural and moral viewpoints have molded the counteraction and treatment of pressure ulcer wounds as a result of the difficulties that they present in the usage of clinical practices. Most associations are at present endeavoring to meet the exposed limit of moral clinical practices (Carlson &Gunningberg, 2017). Be that as it may, there are issues with understaffing which lead to helpless consideration of the weak individuals. In conclusion, from the experiment it was established that the skin tissue was at the pressure scale of 4 kPa while the fatty tissues were at the 0-0.5 kPa range. This meant that skin tissue are normally subjected to greater stress values that the fatty one. The test proved that the donut-shaped gel head support does not work better than simple medical foam. Therefore, this finding reveals that the fluidized positioner was not placed at the same scale of stress-exposure-associated risk to scalp tissue health. The illness possess a threat to the health and life of persons in conditions that trigger its development and thus necessitates a corrective measure to counter its prevalence. The foundations of modern healthcare are based on treating patients with honesty, fairness, dignity, and recognizing their rights. There are various obstacles in addressing the concerns, some of which include non-compliance from the patients and their diverse belief systems. Additionally, the policymakers have difficulties choosing the right protocols to follow due to the controversial literature available. To fully combat the prevalence of pressure injury, it is imperative to consider both the ethical and cultural factors since the solution requires an interdisciplinary approach.
References
Ahn, H., Cowan, L., Garvan, C., Lyon, D., & Stechmiller, J. (2016). Risk factors for pressure ulcers including suspected deep tissue injury in nursing home facility residents: Analysis of national minimum data set 3.0. Advances in Skin & Wound Care, 29(4), 178-190. Web.
Atkinson, R. A., & Cullum, N. A. (2018). Interventions for pressure ulcers: A summary of evidence for prevention and treatment. Spinal Cord, 56(3), 186-198.
Baron, J., Swaine, J., Presseau, J., Aspinall, A., Jaglal, S., White, B., Wolfe, D., & Grimshaw, J. (2016). Self-management interventions to improve skin care for pressure ulcer prevention in people with spinal cord injuries: A systematic review protocol. Systematic Reviews, 5(1), 150−158. Web.
Carlsson, M., & Gunningberg, L. (2017). Unavoidable pressure ulcers at the end of life and nurse understanding. British Journal of Nursing, 26(Sup20), S6-S17.
García‐Sánchez, F. J., Martínez‐Vizcaíno, V., & Rodríguez‐Martín, B. (2019). Conceptualisations on home care for pressure ulcers in Spain: Perspectives of patients and their caregivers. Scandinavian journal of caring sciences, 33(3), 592-599.
Katzengold, R., & Gefen, A. (2019). Modelling an adult human head on a donut‐shaped gel head support for pressure ulcer prevention. International Wound Journal, 16(6), 1398-1407. Web.
Karpegård, E., & Svalstedt, J. (2019). Registered nurses’ experiences of preventing pressure ulcers at a person receiving care at a hospital in Peru: A qualitative study.
Kwong, E. W., Hung, M. S., & Woo, K. (2016). Improvement of pressure ulcer prevention care in private for-profit residential care homes: An action research study. BMC Geriatrics, 16(1), 1−14. Web.
Lavallée, J. F., Gray, T. A., Dumville, J., & Cullum, N. (2018). Barriers and facilitators to preventing pressure ulcers in nursing home residents: A qualitative analysis informed by the Theoretical Domains Framework. International Journal of Nursing Studies, 82, 79-89.
Mccoulough, S. (2019). The history of pressure ulcers. Osca. Web.
Stadnyk, B., Mordoch, E., & Martin, D. (2018). Factors in facilitating an organizational culture to prevent pressure ulcers among older adults in health-care facilities. Journal of wound care, 27(Sup7), S4-S10.
Zaidi, S. R. H., & Sharma, S. (2020). Decubitus Ulcer. StatPearls Publishing

