Case Summary
Rapid City Regional Hospital introduced a comprehensive hand-hygiene initiative to meet The Joint Commission’s Patient Safety Goal on reducing healthcare-associated infections. A root cause analysis revealed three main barriers to compliance: time constraints, skin irritation from frequent washing, and a weak safety culture.
The hospital improved access to alcohol-based hand rubs and approved lotions, provided staff education and encouragement, created a hotline to report non-compliance, and increased physician accountability. As a result, hand hygiene adherence rose from 57% to 91%, leading to a 21% reduction in infections and savings of nearly $300,000.
Influence of Organizational Characteristics on Performance
In the healthcare industry, key metrics that evaluate internal processes are closely tied to the institution’s overall performance. The quality of services, as measured by various indicators, directly affects the hospital’s overall reputation and opportunities for long-term development, which are part of a complex, interconnected medical system. In this case, implementing the clean hands policy at Rapid City Regional Hospital (RCRH) resulted in significant cost savings. Consequently, the characteristics of a healthcare organization and system are directly proportional to the institution’s performance.
In this case, the organization’s characteristics were partly altered by management intervention to focus on a specific issue. The precise formulation of problems and the search for practical solutions in each of the chosen areas were generally consistent with recognized models of organizational change, such as the approaches of Kotter and Lewin (Adelman-Mullally, Nielsen, and Chung, 2023).
In many ways, this case is closely tied to organizational culture, particularly in relation to the daily habits of patients and staff. Even one of the identified causes involved a non-supportive culture—there was no demonstrative and generally recognized example that patients and staff would follow. Accordingly, implementing these organizational cultural characteristics required efforts primarily at the individual level, with support from the organization.
Leadership has initiated change by providing an opportunity not only to learn about the potential benefits of this approach but also to provide alcohol sanitizer and hospital-approved lotion to hygiene areas. Each step was aimed at addressing one of the identified problems: using antiseptics and lotion to keep hands soft after washing; establishing a hotline for quality control and compliance; and, finally, providing training and encouragement to foster a supportive culture.
According to the pyramidal model of organizational culture, management underlies the future trust of patients and staff (Helmreich and Merritt, 2019). Consequently, changing the cultural component of the organization’s policy not only enabled it to address problems but also to achieve critical goals across both clinical and financial metrics.
This case at RCRH demonstrated that hygiene processes can significantly impact an organization’s performance. Continuous optimization should always be dictated by the core values of the healthcare system and is an integral part of the institution’s policy. In this case, aligning goals with values expressed in specific metrics, such as HAI from a clinical perspective and financial metrics from an organizational perspective, made it possible to achieve significant success through thoughtful steps.
The implementation of changes affected the culture, which usually complicates the process; however, in this case, the changes were multi-criteria, incorporating both opportunities for staff and control measures that tracked the organization’s performance as a whole. As a result, the medical institution achieved its goals and developed a tool to promote the right hygiene culture by implementing the ‘do things right’ approach.
Methods to Improve Performance
Although the methods of change were specific, for example, the lean approach, it is impossible to accurately attribute this case to the designated methodology. Washing hands costs time, costs money, and brings value. However, such changes in the mentioned organization increased each resource indicator – both time and monetary costs – so that the value brought a much larger and more significant effect.
The lean approach employs a waste-reduction methodology to either reduce the resource costs associated with processes that add little value or eliminate such processes (Sinha and Matharu, 2019). In this case, the process has been optimized, aligning more closely with the Six Sigma methodology, which primarily aims to reduce process variation (Patel and Patel, 2021). Before the adopted changes, ignoring this hygienic action resulted in approximately 20% of infections and a $300,000 increase in costs, which could be a non-competitive indicator.
After the introduced changes, the indicators improved and approached the industry average or even world-class standards, so the jump turned out to be quite significant. While some metrics are still not at their potential peak—91% instead of 100% are now more committed to the process—improvement has paid off in the KPIs and metrics below. In addition, the Six Sigma approach involves greater involvement of human resources, specifically personnel willing to accept cultural and individual changes.
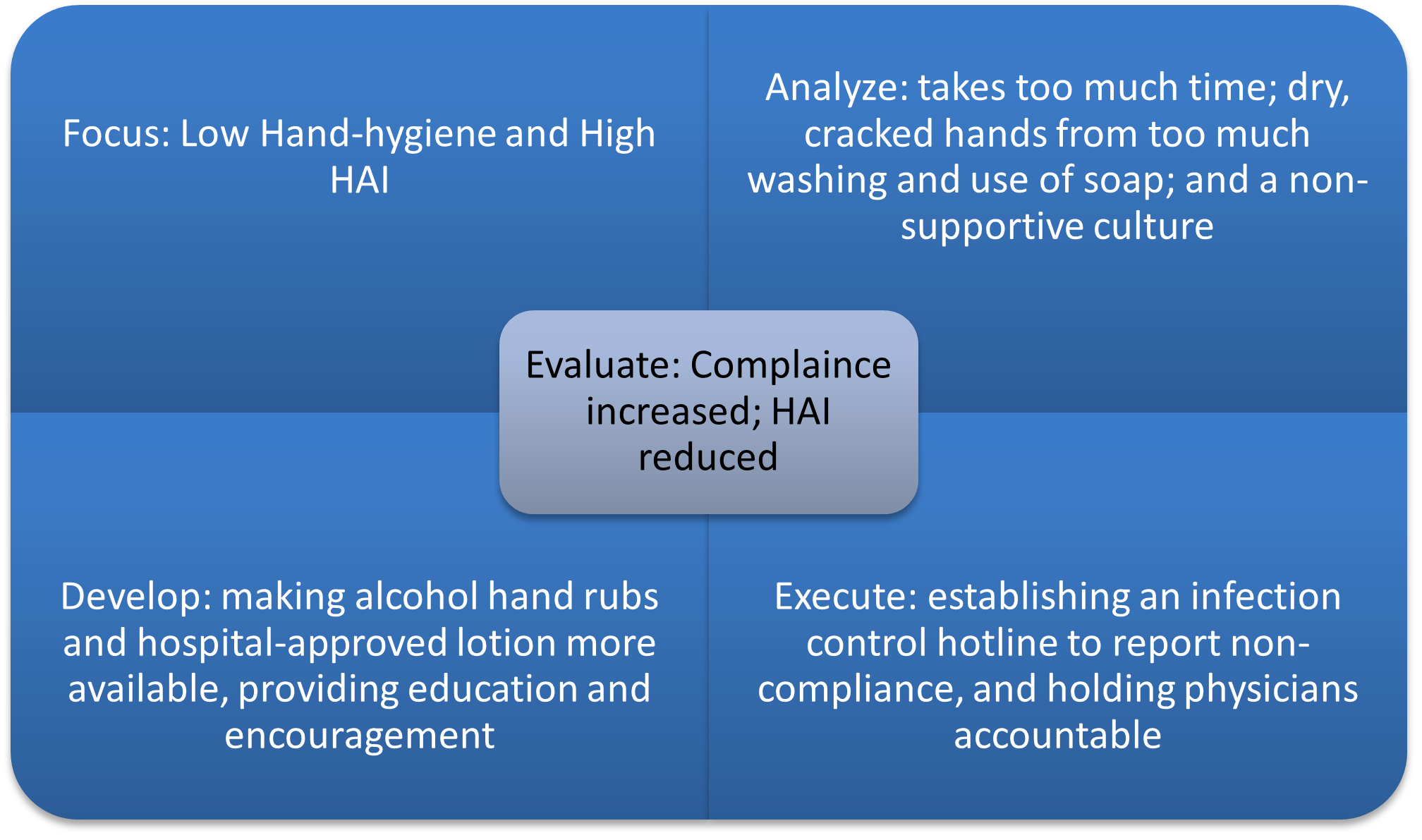
It can be said that RCRH fully implemented the FADE approach, resulting in performance enhancement, as shown in Figure 1. After identifying and focusing on problems and selecting metrics for assessment, the analysis enabled several comprehensive improvement steps, and a control system was introduced in the form of a hotline for receiving complaints. Likely, this case can also be described through the prism of root-cause analysis: the root of the problem lies in personnel hygiene, and a vast array of outcomes could be improved by optimizing the cause.
However, such a technique does not fully capture the full range of actions, ultimately leading to its use at the design stage of these cultural and policy changes. Six Sigma and FADE better describe this case, which involves multiple holistic models and additional steps. Consequently, a root-cause analysis could have been applied in this case; however, it is more likely that thoughtful actions are guided by aspects of Six Sigma or a more general FADE model.
Key Performance Indices Influencing Patient Outcomes
An essential distinction between metrics and KPIs is worth noting: the latter is aimed exclusively at success and constantly evaluates the measured characteristic from a positive or negative perspective. At the same time, the metrics are part of the KPI, expressed as the difference between the current and target values (Bacchi et al., 2022). In this case, RCRH used both clinical and organizational metrics, which have shown significant growth since the changes were implemented, indicating the success of this move.
Clinical KPIs reflect the specifics of the medical industry; the most important and frequently used are distinguished based on the goals set. In the case of RCRH, the clinical metric was chosen in accordance with TJC Patient Safety Goal #7, as the risk of healthcare-associated infections (HAIs) decreased by 21% following the changes.
The choice of this indicator is a clear example of the correct approach to change – it is justified at a sufficiently high level, which, in the case of positive dynamics, leads to improvements in the medical organization’s reputation and overall performance. Perspectively or indirectly, optimizing this value can improve patient satisfaction, reduce readmissions, enhance the effectiveness of care, and other key measures (Tan et al., 2019).
A complex relationship works both ways – with a multi-criteria approach, positive outcomes will be manifested not only in the metrics of the set goal but also in its coincident indicators, which, as a rule, are closely related to each other. Especially when it comes to cultural change, several benefits with the right approach may not even be fully reflected in the metrics under consideration – washing hands outside the institution will create a habit among staff that will maintain health and reduce the risk of disease and, as a result, the number of sick leave and missed work days.
The indicators used in control measures are predominantly quantitative, allowing for more accurate tracking of their dynamics. As mentioned above, RCRH has primarily focused on reducing HAI, a clinical goal because it is related to the patient population. However, given the organization’s close dependence on its efficiency characteristics, this step enabled cost optimization, saving almost $300,000. Therefore, the growth of the medical institution was made possible by these changes. Reducing costs always increases free cash flow and retained earnings, which can then be directed to other improvements or innovations driven by technical or organizational progress (Kimek, 2021).
Although the actual goal of reducing costs was not on the agenda for change, the installation of alcohol-based hand rubs and hand lotions, as well as the establishment of a hotline, required additional costs. However, the coordinated and thoughtful work of management made it possible to achieve success on this indicator as well. In other words, cost optimization initially required investments, which is a common practice with any change. However, these investments not only paid off at the clinical level but also in terms of the resources spent.
Reference List
Adelman-Mullally, T., Nielsen, S., and Chung, S. Y. (2023) ‘Planned change in modern hierarchical organizations: A three-step model’, Journal of Professional Nursing, 46, pp. 1-6.
Bacchi, S., et al. (2022) ‘Automated information extraction from free‐text medical documents for stroke key performance indicators: a pilot study’, Internal Medicine Journal, 52(2), pp. 315-317.
Helmreich, R. L., and Merritt, A. C. (2019). Culture at work in aviation and medicine: National, organizational and professional influences. London, UK: Routledge.
Patel, A. S., and Patel, K. M. (2021) ‘Critical review of literature on Lean Six Sigma methodology’, International Journal of Lean Six Sigma, 12(3), pp. 627-674.
Sinha, N., and Matharu, M. (2019) ‘A comprehensive insight into Lean management: Literature review and trends’, Journal of Industrial Engineering and Management (JIEM), 12(2), pp. 302-317.
Tan, C. N. L., et al. (2019) ‘Measuring the influence of service quality on patient satisfaction in Malaysia’, Quality Management Journal, 26(3), pp. 129-143.

