Description and Objectives
Fall prevention is a critical issue that needs to be addressed as a complex nursing problem. Because of the dire effects that it has on patients’ well-being, including the development of other conditions, falls have to be handled as a phenomenon in aging patients. The goals of the program titled “No More Falls” include reducing the number of falls in the elderly, as well as encouraging patient education, communication between the vulnerable group and nurses, and the introduction of patient independence into the specified setting. By integrating the latest technological innovations for monitoring patients’ well-being with the traditional fall prevention strategies and patient education, one will attain the expected results.
Interventions
There are numerous tools for reducing the instances of falls among the elderly, the choices of which depends on the factor contributing to the fall. Among the causes of a fall, the following reasons are typically identified: poor vision, troubles keeping balance, decreased strength, and use of other drugs that may affect their sense of balance (Coppedge, Conner, & Se, 2016). However, there are other changes in a patient’s health that may cause the propensity toward falls, including age, dizziness, depression, and functional limitations (Lee, Lee, & Khang, 2013).
Moreover, elderly patients may develop orthostasis, suffer from low weight, cognitive impairment, and diabetes, which will cause them to fall often (Carande-Kulis, Stevens, Florence, Beattie, & Arias, 2015). Each cause of fall requires a unique management tool, which implies that the range of strategies for fall prevention in the elderly is truly vast.
Some of the most common approaches toward fall prevention include the provision of walking aids, removal of clutter in a room, reorientation strategies, the use of a bell, changes to patients’ footwear, and use of comfort rounds (Hamm, Money, Atwal, & Paraskevopoulos, 2016). Furthermore, patient education, bed alarms and the drop in the number of restrains used on a patient can be regarded as viable strategies for managing the problem of falls in elderly patients (Growdon, Shorr, & Inouye, 2017).
The strategies involving spatial changes, in turn, can be seen as rather effective since they help to create the setting in which the exposure to immediate threats will be reduced immediately. Particularly, the removal of clutter and the rearrangement of the setting suggests that patients are provided with a greater space for maneuvering, which leads to fewer instances of tripping or stumbling over the elements of the setting. However, the proposed approach can also be regarded as temporary since it does not involve the promotion of patients’ independence in managing their health concerns.
The application of walking aids, in turn, should be deemed as a more effective tool for reducing the propensity to falls among the elderly. When combined with the approach described previously, it creates opportunities for encouraging patient education and promoting independence among the vulnerable group, at the same time allowing them to adjust to the changes in their setting.
A bell, in turn, should be seen as a critical item in managing the needs of patients with the propensity to fall. While encouraging patient independence is critical, the target demographic also needs to receive all available support and assistance of nurses due to the physical limitations of the elderly. The application of a bell will assist patients in calling for help and receiving qualified care. However, it could be argued that the specified approach toward encouraging a patient-nurse contact is rather outdated. Instead of a physical bell as the means of signaling a fall, a patient may need to resort to digital tools such as monitoring devices that require a push of a button to ask for help.
Training
The introduction of the specified programs will require enhanced training. Specifically, nurses will need to acquire the skills of communicating with the elderly, including the provision of instructions, the design of teaching strategies, and the management of misunderstandings that may occur in the process. For this purpose, nurses will need to acquire teaching strategies that inform their choices of approaching the vulnerable demographic.
The training will involve both the strategies that prevent falls in the elderly and the approaches toward assisting the patients that have experienced a fall. The latter skills also include the ability to introduce patient education tools into the selected setting and encourage patients to acquire skills and knowledge associated with managing and preventing falls. Thus, comprehensive care will be provided to the specified demographic.
Tools
In order to implement the program, one will require several tools that will assist the patients in their transition to a new mode of moving across their setting. For instance, walking aids should be regarded as an important addition to the existing array of devices for helping the elderly with the prevention of falls (Coppedge et al., 2016). Furthermore, devices that allow for an immediate dialogue between a patient and a nurse have to be integrated into the program for fall prevention. The specified type of objects ranges from basic bells to much more intricate devices such as digital tools for monitoring patients’ well-being (Growdon et al., 2017).
The proposed strategies are likely to have a vastly positive effect on the problem of falls among the elderly. With a combination of the consistent patient support and the encouragement of independence among the elderly, a positive shift is expected. In addition, the fact that modern tools of monitoring patients’ well-being provide numerous opportunities for enhancing patient-nurse communication deserves to be addressed.
Marketing Plan
In order to promote the suggested strategy, one should consider incorporating both traditional and digital media into the marketing plan. Organizations that focus on addressing the needs of senior citizens should be viewed as the target audience since the program will have to be implemented at the institutional, administrative, and organizational levels. The SMART goals of the plan include attracting the attention of an influential healthcare organization, increasing the use of the proposed tool for fall management by 20%, introducing a positive shift in the management of falls, improving the quality of life among the elderly, and implementing the program within the next three months. In addition, it is critical to take the current opportunities and threats into account (see Fig. 1).
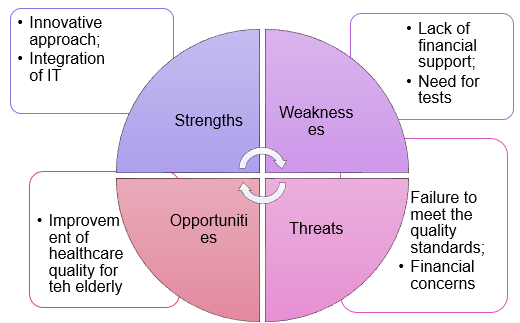
As the SWOT analysis shown above indicates, the suggested intervention is likely to face significant financial constraints due to the incorporation of innovative technologies into the framework thereof. Nonetheless, the program provides an innovative approach toward managing falls by integrating the existing strategies and adopting a patient-centered approach. Therefore, it is reasonable to pursue the available opportunities for improving the quality of care by investing in the further promotion of the proposed intervention to healthcare organizations. As a result, the levels of well-being among patients will rise, and the elderly will avoid developing additional health issues associated with falls.
Estimated Cost
It is expected that the project will require a total of at least $10,000,000. The specified amount of money will ostensibly suffice for building a comprehensive program, purchasing the necessary resources, recruiting participants, creating the setting for interdisciplinary cooperation, and attracting partners. Specifically, $1,000,000 will be required to pay the salaries to nurses and healthcare experts involved in the project. $5,000,000 will be needed to facilitate the necessary technology and ensure that the data management techniques are coherent and appropriate. The specified expenses also involve the costs for communication and data management.
Furthermore, to deploy all available resources and ensure that the program incorporates opportunities for both nurses and patients to use the available educational resources, $3,000,000 will be required. It is expected that the process of patient education should involve innovative techniques and be adjusted to the needs of the elderly. Finally, one should consider investing $1,500,000 in marketing. It is critical to attract the attention of influential patrons, who will offer extensive chances for improving healthcare services and preventing falls among senior citizens.
Conclusion
To build a sustainable program for improving the health rates among the elderly by reducing the threat of falls among them, one should consider incorporating the elements of spatial rearrangement, patient education, and communication enhancement between a nurse and a patient. The specified changes are expected to produce a positive shift in the present-day dynamics in the healthcare environment. By maintaining communication with nurses and at the same time experiencing a certain degree of independence in managing their health needs, the elderly will feel empowered, which will increase their chances for avoiding falls, whereas nurses will exert tighter control over the vulnerable demographic.
References
Carande-Kulis, V., Stevens, J. A., Florence, C. S., Beattie, B. L., & Arias, I. (2015). A cost–benefit analysis of three older adult fall prevention interventions. Journal of Safety Research, 52, 65-70. Web.
Coppedge, N., Conner, K., & Se, S. F. (2016). Using a standardized fall prevention tool decreases fall rates. Nursing, 46(3), 64-67. Web.
Growdon, M. E., Shorr, R. I., & Inouye, S. K. (2017). The tension between promoting mobility and preventing falls in the hospital. JAMA Internal Medicine, 177(6), 759-760. Web.
Hamm, J., Money, A. G., Atwal, A., & Paraskevopoulos, I. (2016). Fall prevention intervention technologies: A conceptual framework and survey of the state of the art. Journal of Biomedical Informatics, 59, 319-345. Web.
Lee, A., Lee, K. W., & Khang, P. (2013). Preventing falls in the geriatric population. The Permanente Journal, 17(4), 37. Web.

