The older adult participating in the assessment project is the interviewer’s neighbor. The participant, N. M., is a retired police officer, 72 years old, female, widowed. N. M. has been living alone for three years since her husband died, and her children are far away. The project involves using a questionnaire and several physical assessment tools to find out the participant’s disposition to health problems. The comparison between N. M.’s answers and relevant literature is made, and interventions for the identified issues are offered.
Summary of Questionnaire Findings
The questionnaire included 11 obligatory questions and several additional ones. N. M.’s philosophy on living a long life is the refusal of smoking and abusing alcohol, regular exercising, and checking the condition of one’s health at least once a year. For N. M., people are considered “too old” when they cannot cope with such needs as getting dressed, eating, eliminating by themselves without any outside help. From her experience of staying at a hospital, the participant is quite satisfied with the status and treatment of older adults in the modern healthcare system. N. M. admits that she is not a religious person. Still, she partially believes in the concept that people’s diseases are the punishment for their bad deeds. Health promotion activities that N. M. participates in include walking several kilometers every day and eating fresh vegetables and fruit.
When asked about any special things that helped the respondent live so long, N. M. says that it was the love she and her husband had. However, after his death, N. M. feels that her health is deteriorating and there is no more sense in life. N. M.’s children encourage her to take care of herself, and they have arranged for a social worker to come over four times a week to help their mother. N. M.’s parents are still alive, and one of her grandmothers was a centenarian. Thus, the lifespan of the participant’s family members is quite long. There are no dietary traditions in the patient’s culture or any remedies which have been handed down in the family that could be attributed to aiding long life.
N. M. describes her current health status as satisfactory but admits that it has deteriorated in comparison with the past state, which she could have called excellent. The values that guided the participant’s life so far are friendliness, trust, understanding, responsibility, and support. Additional questions were concerned with any changes in memory or cardiovascular system and bad habits. N. M. reports no problems with remembering dates and places. However, she admits occasional difficulty recognizing a person in the street. Also, she had to refrain from driving a year ago because she got distracted and almost caused a car accident. N. M. has noted a recent deterioration of the cardiovascular system that is represented by chest pain. The patient had smoked for thirty years, but she quit smoking ten years ago.
Comparison and Contrast of Client’s Responses with Findings in Current Literature
N. M.’s responses are similar to the data found in current literature. In particular, Perls (2017) remarks that women tend to become centenarians more frequently than men. Taking into account that N. M.’s grandmother lived to be 100 years and that her parents are still alive, it is viable to assume that the client is likely to reach such advanced age. Another scholarly source confirming N. M.’s responses is the article by Howlett (2017) on the effect of aging on the cardiovascular system. Howlett (2017) mentions that there is a high risk of this illness in older adults who smoke or used to smoke. Therefore, it is possible to conclude that participant’s responses coincide with scholarly discussions on the theme of advanced age.
Physical Assessment Results
A comprehensive physical and mental assessment of the patient was performed with the help of the following tools:
- Tinetti balance and gait evaluation (“Tinetti balance assessment tool,” n.d.);
- Katz index of activities of daily living (Shelkey & Wallace, 2012);
- the Barthel index (“Barthel index of activities of daily living,” 1993);
- the assessment of home safety (Olsen & Hutchings, 2006).
The results obtained with the help of four assessment tools indicate that the patient’s ability to take care of herself is satisfactory. N. M. scored 10 out of 16 points in the balance section of Tinetti balance and gait evaluation. The participant scored 21 out of 28 points in the gait section of the tool at the usual pace and 18 out of 28 points at a rapid pace. According to Katz’s index of activities of daily living, N. M. is moderately independent, scoring 4 points out of 6. The Barthel index (15 out of 20) is consistent with the other tools’ results. The assessment of home safety indicates that some areas in N. M.’s house may be regarded as potentially dangerous and should be improved.
The Comparison Between Age-Related Changes and the Expected Changes
All changes recorded in the course of the interview and assessment are consistent with the expected alterations at this age. Some problems with keeping balance have developed, which is a common issue for older adults (Noll, 2013). Also, N. M. admits some complications in the work of the urinary tract, which is regarded as one of the usual problems in older people (Smith & Kuchel, 2017). Another expected change is associated with the cardiovascular system (Howlett, 2017). This complication has also been found during the patient’s assessment. Therefore, age-related alterations in N. M. coincide with the expected changes.
Preliminary Issues
Issue 1: Balance
Based on the findings obtained with assessment tools, N. M. has some balance issues.
Issue 2: Frailty
The lack of strengths was noticed in N. M. as a result of the evaluation.
Issue 3: Cardiovascular System
The patient admits to having problems with her cardiovascular system.
Issue 4: Urinary Tract Dysfunction
Occasional loss of control of the bladder is experienced by N. M.
Suggested Alterations in Health
The primary suggestion for the participant is doing some physical exercises advised by the physician. These exercises should be aimed at increasing the patient’s physical health and eliminating unpleasant feelings related to the cardiovascular system. The second piece of advice is to spend more time in the open air and communicate with other people. N. M. seems to be spending too much time alone without any social interaction. The third suggested alteration is consuming vitamins or medications that will promote strength in N. M.’s body system as well as make her feel more energetic and enthusiastic.
Interventions for the Identified Problems
Issue 1: Balance
To enhance N. M.’s balance issues, it is recommended to increase physical activity. Also, osteopathic treatment may be a viable solution upon consideration. Apart from these changes, it is crucial to equip N. M.’s house with grab bars where necessary. The following interventions are offered:
- Increased physical activity (Bherer, Erickson, & Liu-Ambrose, 2013);
- Installing sturdy grab bars in the house;
- Osteopathic manipulative treatment (Noll, 2013).
Issue 2: Frailty
To eliminate the feeling of weakness, N. M. should spend more time outdoors and eat healthy food. Also, pharmacological interventions may be a good solution. The following options are suggested:
- Nutritional interventions;
- Pharmacological approaches;
- Exercising (Clegg, Young, Iliffe, Rikkert, & Rockwood, 2013).
Issue 3: Cardiovascular System
Problems with the cardiovascular system at this age may lead to serious consequences, so it is crucial to managing them as soon as they develop. The management plan may involve the following options:
- Lifestyle behavior modification;
- Exercising (Lavie et al., 2015);
- Mobile applications (results could be sent to the physician or the social worker) (Logan, 2013).
Issue 4: Urinary Tract Dysfunction
Although this system does not bother N. M. frequently, the problem is rather serious since it creates discomfort and may lead to low self-esteem. To eliminate issues with urinary tract dysfunction, the following options may be tried:
- Designing a toileting program;
- Lifestyle modifications (change in fluid intake);
- Mobility enhancement (Jung, Kim, & Cho, 2015).
Conclusion
The project was aimed at performing a thorough assessment of an older adult and suggesting interventions for the issues identified as a result of the evaluation. It has been found that the participant is prone to cardiovascular system problems, urinary tract dysfunction, frailty, and balance issues. The recommended interventions include physical activity, lifestyle modifications, and an increased social activity. The patient’s cultural awareness and competency do not create any obstructions to the implementation of the suggested options.
References
Barthel index of activities of daily living (ADL index). (1993). Occasional Paper (Royal College of General Practitioners), 59(24).
Bherer, L., Erickson, K. I., & Liu-Ambrose, T. (2013). A review of the effects of physical activity and exercise on cognitive and brain functions in older adults. Journal of Aging Research, 2013, 1-8.
Clegg, A., Young, J., Iliffe, S., Rikkert, M. O., & Rockwood, K. (2013). Frailty in elderly people. Lancet, 381, 752-762.
Howlett, S. E. (2017). Effects of aging on the cardiovascular system. In H. M. Fillit, K. Rockwood, & J. Young (Eds.), Brocklehurst’s textbook of geriatric medicine and gerontology (8th ed.) (pp. 96-100). Philadelphia, PA: Elsevier.
Howlett, S. E. (2017). Effects of aging on the cardiovascular system. In H. M. Fillit, K. Rockwood, & J. Young (Eds.), Brocklehurst’s textbook of geriatric medicine and gerontology (8th ed.) (pp. 96-100). Philadelphia, PA: Elsevier.
Jung, H. B., Kim, H. J., & Cho, S. T. (2015). A current perspective on geriatric lower urinary tract dysfunction. Korean Journal of Urology, 56, 266-275.
Lavie, C. J., Arena, R., Swift, D. L., Johannsen, N. M., Sui, X., Lee, D., … Blair, S. N. (2015). Exercise and the cardiovascular system: Clinical science and cardiovascular outcomes. Circulation Research, 117(2), 207-219.
Logan, A. G. (2013). Transforming hypertension management using mobile health technology for telemonitoring and self-care support. Canadian Journal of Cardiology, 29(5), 579-585.
Noll, J. R. (2013). Management of falls and balance disorders in the elderly. The Journal of the American Osteopathic Association, 113(1), 17-22.
Olsen, R. V., & Hutchings, B. L. (2006). Home safety assessment checklist. Web.
Perls, T. T. (2017). Successful aging: The centenarians. In H. M. Fillit, K. Rockwood, & J. Young (Eds.), Brocklehurst’s textbook of geriatric medicine and gerontology (8th ed.) (pp. 16-21). Philadelphia, PA: Elsevier.
Shelkey, M., & Wallace, M. (2012). Katz index of independence in activities of daily living (ADL). Try This: Best Practices in Nursing Care to Older Adults, 2.
Smith, P. P., & Kuchel, G. A. (2017). Aging of the urinary tract. In H. M. Fillit, K. Rockwood, & J. Young (Eds.), Brocklehurst’s textbook of geriatric medicine and gerontology (8th ed.) (pp. 133-137). Philadelphia, PA: Elsevier.
Smith, P. P., & Kuchel, G. A. (2017). Aging of the urinary tract. In H. M. Fillit, K. Rockwood, & J. Young (Eds.), Brocklehurst’s textbook of geriatric medicine and gerontology (8th ed.) (pp. 133-137). Philadelphia, PA: Elsevier.
Tinetti balance assessment tool. (n.d.). Web.
Appendix A
Patient Identification
- Age: 72 years old
- Profession: retired police officer
- Gender: female
- Marital status: widowed
Appendix B
Tinetti Balance and Gait Evaluation
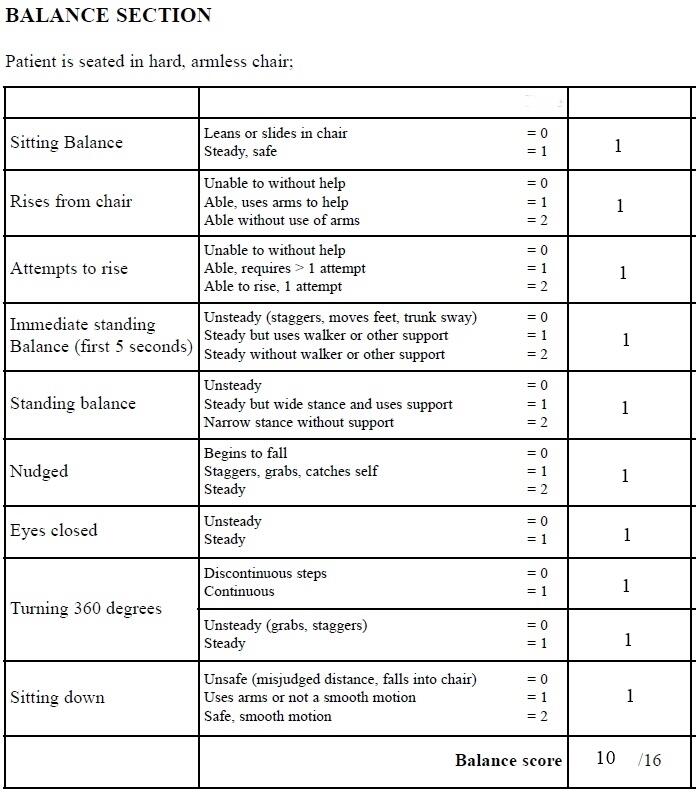
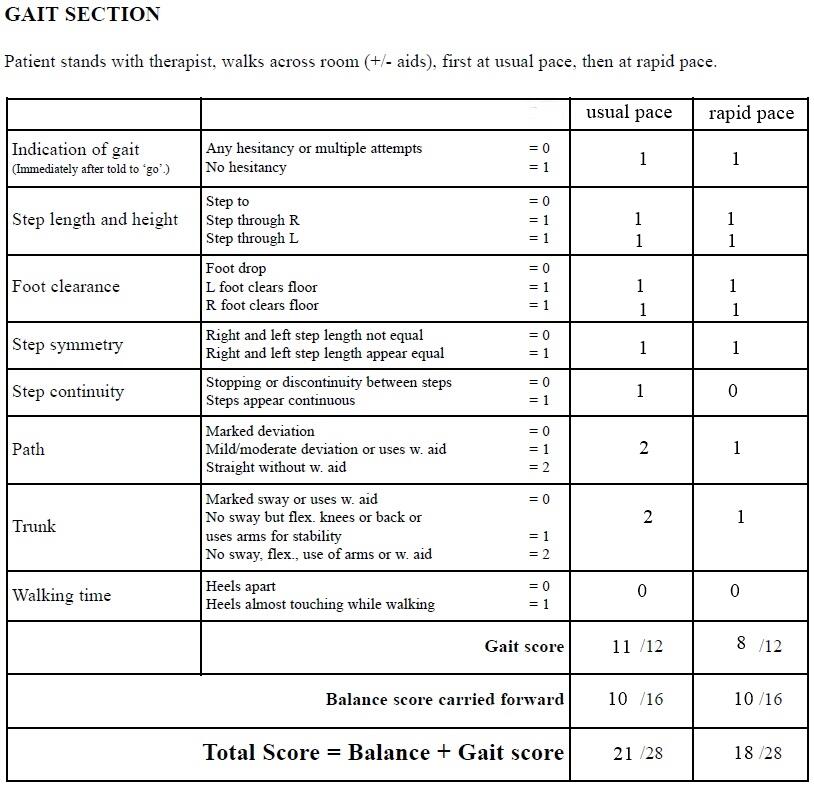
Appendix C
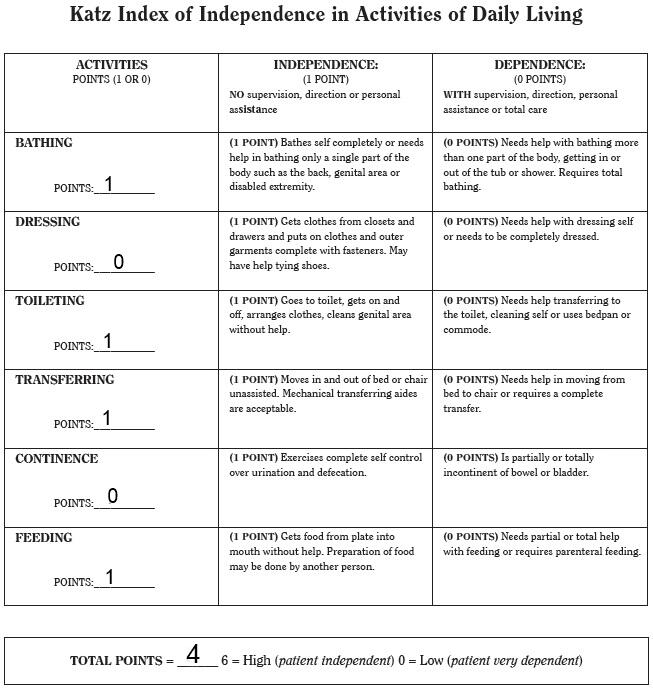
Appendix D

Appendix E
The Assessment of Home Safety
Entry to the Home
Lighting
Is there adequate lighting in the following areas:
Y N Driveway?
Y N Garage?
Y N Walkways?
Y N At all doors?
Y N Near the trash area?
Y N Any other areas of the yard that are used after dark?
Driveway
Y N Is the driveway smooth and evenly paved?
Y N Is the transition between the driveway and surrounding surfaces (such as the yard), smooth and even, free of ruts and other things (rocks) that could cause tripping?
Y N Is the slope of the driveway low enough that it does not cause a problem?
Walkways
Y N Are walkways smooth and level (no cracks, gaps, or other tripping hazards)?
Y N Are steps along walkways clearly visible?
Y N Do they have handrails?
Y N Are transitions between different surfaces (a patio and sidewalk, concrete and asphalt, walkway and grass, etc.) even and level?
Y N If there are steeply inclined walkways, do they have sturdy, easy to grasp, handrails?
Y N Are shrubs, bushes, and grass trimmed back or removed so that they do not infringe on or obstruct the walkway (potential tripping hazard)?
Steps to the Doors
Y N Do all steps (even single steps) have sturdy, easy to grasp (cylindrical) rails on both sides?
Y N Are the risers on stairs and multiple steps of equal height?
Y N Are the stair treads sturdy, level, and in good condition?
Y N Have small single steps (that could cause tripping) been mini-ramped?
Garage
Y N Are there adequate overhead lights in the garage?
Y N Is there a clear pathway to walk through?
Y N Do entry stairs or ramps to the house have railings?
(If Applicable) – not applicable
Y N Are ramps rising at a minimum slope of 12:1 (12 inches of ramp length for every 1 inch of height is standard. However, 16:1 is recommended.)
Y N Do ramps have sturdy rails on both sides?
Y N Are the rails cylindrical for easy grasping?
Y N Do ramps have smooth transitions from ramp surface to ground surface?
Y N Do ramps have non-skid surfaces or have non-skid strips been added?
Y N Do ramp railings extend beyond the ramp to help people transition off the ramp?
Y N Do ramps have sufficient width of at least 36” between handrails?
Entry Landings
Front Rear
Y N Y N Have all potential tripping hazards been removed?
Y N Y N Is the landing wide and deep enough to safely open the door?
Y N Y N Is there a clearly visible, easily reachable doorbell?
Y N Y N Do porches and decks have railings or barriers to prevent someone from stepping or falling off? (Are the railings secure?)
Y N Y N Does the decking have secure, even floorboards with no protruding nails?
Y N Y N Is there a non-skid surface on the porch/deck/landing?
Y N Y N Do doormats have non-skid backing with no upturned corners?
Exterior Doors
Front Rear
Y N Y N If necessary, are doorways wide enough to accommodate wheelchairs?
Y N Y N Are locks in good working order and easy to use?
Y N Y N Are latches and door handles in good condition and easy to use?
Y N Y N If someone has trouble turning a doorknob, are there lever handles?
Y N Y N Do the doors open and close easily without sticking?
Y N Y N Do doors on springs close slowly enough (so they don’t close on someone going through the door)?
Y N Y N Is the threshold at the door less than one inch high?
Y N Y N Do glass sliding doors have decals at eye level?
Other Outdoor Area Concerns
Y N If there is a patio or deck, is it level, smoothly surfaced and free of tripping hazards?
Y N Are walkways around the house, smooth and free of obstacles and overgrown shrubbery, grass, and weeds that could cause tripping?
Y N Are garbage and recycling areas well lighted?
Y N Do these areas have safe, accessible stairs and railings?
Inside the Home
Entry Ways and Vestibules
Front Rear
Y N Y N Have throw rugs (potential tripping hazards) been removed?
Y N Y N Is there a clear pathway (devoid of clutter) through the entry hall?
Y N Y N Are all cords and wires out of the pathway?
Y N Y N Are thresholds low enough so someone does not trip over them?
Y N Y N Is there adequate lighting?
Y N Y N Is the light switch at the entrance to the room?
Y N Y N If necessary, is the entryway wide enough for a wheelchair/walker?
Hallway(s)
Y N If people need support, are there handrails along the hall?
Y N Are halls free of clutter and other tripping obstacles?
Y N Are carpet runners tacked down or have anti-skid backing?
Y N Are thresholds less than one inch so they are not tripping hazards?
Y N If necessary, are halls wide enough for a wheelchair/walker?
Y N Is there adequate lighting?
Y N Is there a light switch at both ends of the hall?
Doors/Doorways
Y N Do all doors open easily?
Y N Are thresholds less than one inch?
Interior Stairs
2nd Fl. Base. Other
Y N Y N Y N Do stairs have sturdy rails on both sides?
Y N Y N Y N Do rails continue onto the landings?
Y N Y N Y N Are the stair treads sturdy, not deteriorating or broken?
Y N Y N Y N Are edges of stair treads clearly visible (no dark, busy patterns)?
Y N Y N Y N Are stair pads in good repair (tacked down, in one piece)?
Y N Y N Y N (If bare wood) Are stair treads slip-resistant?
Y N Y N Y N (If carpeted) Is carpet securely attached, not worn/frayed?
Y N Y N Y N Are top and bottom steps highlighted?
Y N Y N Y N Are stairs free of clutter?
Y N Y N Y N If stairs have a low, overhanging beam that people could bump their heads on, has it been padded?
Y N Y N Y N Are stairs and landings well lit, with light switches at both top and bottom?
Living/Dining/Family/Other Rooms
LR DR FR Other
Y N Y N Y N Y N Is the lighting adequate?
Y N Y N Y N Y N Is there a light switch at the entrance to the room?
Y N Y N Y N Y N Is there a clear, unobstructed path through the room (no clutter, cords, wires, baskets, and other things to trip over)?
Y N Y N Y N Y N Are thresholds minimal and carpet binders tacked down?
Y N Y N Y N Y N Are carpets in good condition (not frayed or turned up, torn, or with worn spots that someone could trip over)?
Y N Y N Y N Y N Are plastic runners/carpet protectors tacked down (not folded or turned up at edges)?
Y N Y N Y N Y N Do throw rugs have anti-skid backing and no upturned corners?
Y N Y N Y N Y N Is tile/linoleum free of chips, tears, and not slippery?
Y N Y N Y N Y N Are bare wood floors slip resistant?
Y N Y N Y N Y N Is there at least one comfortable chair people can get in and out of safely and easily?
Y N Y N Y N Y N Do tables have rounded edges that are clearly visible (no sharp edges or made of glass)?
Y N Y N Y N Y N Do windows open easily?
Y N Y N Y N Y N Are shades and blinds easy to open?
Y N Y N Y N Y N Are they securely attached?
Bathrooms
General Considerations
Bath1 Bath 2
Y N Y N Is there a light switch at the entry?
Y N Y N Is there adequate lighting overall?
Y N Y N …..At the sink?
Y N Y N …. Over the tub/shower?
Y N Y N Is there a night light?
Y N Y N Is the door threshold less than one inch?
Y N Y N Is the room free of clutter and tripping hazards?
Y N Y N Is the flooring non-slip/non-skid (including throw rugs)?
Y N Y N Are there grab bars in other areas of the room as needed?
Y N Y N Is the room kept warm during bathing (heat lamp, towel warmers, etc.)?
Sinks
Bath1 Bath2
Y N Y N Are sink faucets easy to reach and read?
Y N Y N Is it easy to determine where the hot and cold areas of the faucet are?
Y N Y N Is it easy to mix the temperature?
Y N Y N If necessary, have anti-scald devices been installed?
Y N Y N Is the sink wheelchair accessible or can someone sit at the sink?
Y N Y N Are mirrors at an appropriate height?
Tub/Shower
Bath1 Bath2
Y N Y N Are there sturdy grab bars in the tub and/or shower, if needed?
Y N Y N Is the shower curtain bottom out of the way so it is not a tripping hazard?
Y N Y N Are toiletries in the tub easily reached from sitting and standing positions?
Y N Y N Is there a non-skid bathmat in the bathtub?
Y N Y N Is there a hand-held shower head?
Y N Y N Are tub/shower faucets easy to use and read (hot & cold clearly marked)?
Y N Y N If needed, is there a tub or shower seat?
Toilet
Bath1 Bath2
Y N Y N Are there sturdy grab bars at the toilet (or toilet arms and a raised seat)?
Y N Y N Is toilet paper easily reachable from the toilet seat?
Y N Y N Is the toilet seat in good condition and securely fastened?
Kitchen
Y N Are frequently used items visible and easily reached (front of pantry and refrigerator)?
Y N Are sink faucets easy to reach and read?
Y N Is it easy to determine where the hot and cold areas of the faucet are?
Y N Is it easy to mix the temperature?
Y N If necessary, have anti-scald devices been installed or the hot water temperature lowered?
Y N If necessary, have timers been installed on the oven and cook top?
Y N Are burners and control knobs clearly labeled and easy to use?
Y N Are the controls on the front of the stove, not the back?
Y N Is there a close resting place nearby for hot vessels coming out of the oven?
Y N Is glass cookware being used so person sees food is being cooked?
Y N Is the microwave easy to read, reach, and operate?
Laundry Room
Y N Is there a light switch at the entry?
Y N Is there sufficient lighting?
Y N Is the route to the laundry room (stairs) safe?
Y N Are the appliances at the right height so it easy to get clothes in/out of the washerand dryer?
Y N Are the control knobs easy to reach, read, and operate?
Y N Are laundry supplies easy and safe to reach?
Y N Is there a non-slip floor surface?
Y N Are tripping hazards off the floor (laundry basket or dirty clothes)?
BR1 BR2
Y N Y N Is there a light at the entrance to the room?
Y N Y N Is a light reachable from the bed?
Y N Y N Can bureau drawers be reached (height of the drawer) and opened easily?
Y N Y N Is there a clear, unobstructed path through the room (clutter and furniture are out of the way)?
Y N Y N Are cords and wires off the floor?
Y N Y N Do throw and area rugs have non-slip backing and no upturned corners?
Y N Y N Are wood and linoleum floors non-skid?
Y N Y N Is carpet smooth (no folds or holes) and tacked down?
Y N Y N Are curtains and bed coverings off the floor so they are not tripping hazards?
Y N Y N Is there support for getting in and out of bed, if needed?
Y N Y N Is there a place to sit and get dressed, if needed?
Y N Y N Are windows easy to open and close?
Y N Y N Are window blinds and shades working properly and easy to open?
Y N Y N Are blinds and shades properly secured?
Closets
Clo 1 Clo 2
Y N Y N Are shelves and clothes poles easy to reach?
Y N Y N Have closet organizers been installed to maximize use of space?
Y N Y N Are closets organized so clothes are easy to find?
Y N Y N Are clutter and other tripping hazards off the floor?
Y N Y N Do closets have lights that are easy to find and reach?
Y N Y N Are closet door easy to open?
Y N Y N If closet has sliding doors, do they stay on track?
General Home Safety Concerns
Y N Can an older person contact someone in an emergency (medi-alert, names and numbers by phone, picture telephone, etc.)?
Y N Are smoke detectors and carbon monoxide alarms installed and working?
Y N Is there a fire extinguisher in the house?
Y N Is there a safe place outside to hide a key to the house for emergency entry?
Specific Checklist for Alzheimer’s Disease and Other Dementias – Not Applicable/Not Needed.

