Introduction
Several technologies exist that help create detailed images of the internal body structures. Computerized tomography is one such technology, and CT images are created using X-rays. CT scanning is applied to diagnose and control multiple conditions and diseases, such as cancer, bone and joint problems, heart and lung diseases, and different kinds of injuries.
It is also used to evaluate the progression of conditions and assess the patient’s state before surgical interventions. In general, computerized tomography is a machine that emits X-rays on one side and receives them on the other; the received data is later processed to create an image. Though highly effective, CT is only recommended when necessary, as patients are exposed to a radiation dose.
Equipment and Image Production
CT equipment consists of several parts, with a large, doughnut-shaped machine serving as the basis. The patient lies on a table that moves them through the X-ray machine. In general, the process of CT scanning involves a CT doughnut-shaped machine emitting a narrow X-ray beam aimed at the patient (Computed Tomography (CT), 2022, para. 1). As these rays are rotated, they produce signals that are later processed by a computer. After processing is complete, a cross-sectional image is created by combining the received data (CT, 2022, para. 2). The image can be viewed from different angles and reconstructed into a 3D image.
The primary difference between traditional X-rays and CT scans is the rotation of the X-ray beam. It is precisely the rays’ rotation around the patient’s body, emitted through the tube, that helps create high-resolution 3D images (Seeram, 2022, p. 20). The table moves the patient while the rays are emitted and rotated; this way, the patient’s internal body structures can be observed from different angles later.
The figure below illustrates the process of the rays rotating around the body inside the tube. It also demonstrates how the rays are emitted from multiple sources, pass through the patient’s body, and are detected by various detectors (Withers et al., 2021, p. 4). Modern CT technology, featuring increased gantry rotation speed and additional detector rows, enhances image resolution and yields more detailed results (Lell & Kachelrieß, 2020, p. 8).
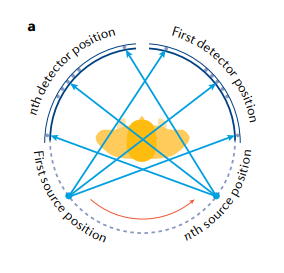
In some cases, professionals also use contrast agents to improve the visualization of specific areas of the patient’s body. These are substances that are either injected or administered orally to the patient before the procedure (Seeram, 2022, p. 98). The material in the agent absorbs X-rays; this is reflected in the received image. This procedure helps clarify the image when there are doubts about the patient’s diagnosis.
Safe Working and Radiation Legislation
Due to the ionizing radiation involved in CT scanning, specific guidelines must be followed to ensure the procedure is as safe as possible for both the patient and the professionals. Firstly, it is essential to accurately assess the patient’s medical history, including information about allergies or kidney problems, in case the use of contrast is planned (Singh and Sandean, 2023, para. 5). Secondly, it is crucial to provide the patient with all necessary information regarding the scan in advance. This includes asking the patient to remove all metal objects and abstain from eating and drinking for several hours before the procedure. Lastly, it is necessary to follow radiation safety protocols.
In the United Kingdom, radiation safety protocols are established by the Ionizing Radiation Regulations 2017. The regulations require the professionals to always present the justification for the use of radiation (The Ionizing Radiation Regulations 2017, para. 5). This means that CT must only be resorted to when strictly necessary. The benefits and risks must be assessed properly each time healthcare providers consider CT scanning. The radiation dosage must be accurately tracked, and the patient must be closely monitored for potential adverse effects. In general, unnecessary radiation exposure should be avoided when possible.
Risks and Benefits to the Patient
CT is not a completely harmless technology to apply, which is why its use is limited to strictly necessary cases. In these cases, the benefits of applying this scanning method must outweigh the risks. The primary benefit of computerized tomography is that it is a non-invasive procedure that causes no physical pain or discomfort to the patient.
Moreover, this procedure does not take much time to carry out. Being a non-invasive scanning method, it provides comprehensive data on the patient’s condition; nonetheless, the CT images are detailed and high-resolution. It is also a relatively accessible procedure.
Despite the apparent benefits, there are significant risks that limit the use of this technology. The most critical risk for patients’ health is exposure to ionizing radiation. Although recent technologies have reduced radiation exposure, the risk of radiation-related consequences remains.
One risk associated with ionizing radiation is carcinogenicity (Callahan et al., 2018, p. 21). The risk, however, is directly related to the dosage: “biologic injury from ionizing radiation is directly proportional to dose; that risk increases with cumulative exposure” (Callahan et al., 2018, p. 22). This indicates that the technology should be limited in its application. At the same time, children are also at higher risk of negative radiation consequences, such as cancer development; thus, the radiation dosage should be lower for them.
Conclusion
Computerized tomography is an effective diagnostic and monitoring tool for various conditions. It is a non-invasive method that involves activating a machine in the form of a tube, which emits and rotates X-rays around the body of a person lying on a moving table. After the detector perceives the rays, the computer processes the received data and creates a highly detailed image.
There are multiple benefits to applying CT, including high effectiveness with minimal time and invasion required. There are, however, risks related to ionizing radiation; frequent exposure, in particular, creates a disposition for cancer development, especially in children. This is why safety rules must be followed at all times, and the radiation-related norms set out in UK legislation must be complied with.
Reference List
Callahan, M. J. et al. (2018) ‘Ionizing radiation from computed tomography versus anesthesia for magnetic resonance imaging in infants and children: patient safety considerations’, Pediatric Radiology, 48(1), pp. 21–30.
Computed tomography (CT) (2022). NIH.
Computed tomography (CT) scans and cancer (2019). National Cancer Institute.
Lell, M. M. and Kachelrieß, M. (2020) ‘Recent and upcoming technological developments in computed tomography’, Investigative Radiology, 55(1), pp. 8–19.
Seeram, E. (2022) Computed tomography: Physical principles, patient care, clinical applications, and quality control. 5th edn. Philadelphia, PA: Elsevier Inc.
Singh V. and Sandean DP. (2023) ‘CT patient safety and care’, In StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing.
The Ionizing Radiation Regulations 2017 (2017). Legislation.gov.uk.
Withers, P. J. et al. (2021) ‘X-ray computed tomography’, Nature Reviews Methods Primers, 1(18), pp. 1–21.

